Sunflower Code Code on the ICD 10. The extension process in the abdominal cavity is dangerous. Prevention of adhesive disease
RCRZ (Republican Center for Health Development MD RK)
Version: Clinical protocols MOR RK - 2014
Pelvic peritoneal spikes in women (N73.6)
obstetrics and gynecology
general information
Short description
Approved on the expert commission
On health development
Ministry of Health of the Republic of Kazakhstan
Spikes - These are subtle trenches, films and fits arising between neighboring bodies. The emergence of the adhesive process is the irritation of the peritoneum - a kind of shell covering internal organs from side abdominal cavity. Factors leading to the formation of adhesions in a small pelvis: preceding operations on abdominal organs and small pelvis (laparotomy, laparoscopy), inflammatory diseases of the uterus, outer genital endometriosis [2, 3,4,5,6].
I. Introductory part
Protocol name: Pelvic peritoneal spikes
Protocol code
Code (s) μb-10:
Abbreviations used in the protocol:
Ultrasound ultrasound examination
MRI - magnetic resonance tomography
OMT - small pelvis organs
OAK - Common Blood Analysis
Asat - Aspartate Transaminase
Alat - Alaninotransferase
ECG - electrocardiogram
RW - Wasserman Reaction
HIV - human immunodeficiency virus
UD - level of evidence
Protocol development date: year 2014.
Category of patients - Patients who have a history of several operations on the abdominal and pelvic cavity organs, expressed pelvic peritoneal spikes with the involvement of the intestine, the gland and the organs of the small pelvis.
Users Protocol - Doctors obstetrician - gynecologists of hospitals.
I: The evidence obtained from at least one properly randomized controlled study.
II-1: Evidence of well-developed controlled studies without randomization.
II-2: evidence of well-developed cohorts (alleged or
Retrospective) or study by case-control method, preferably more than one center or research group.
II-3: Evidence derived from comparisons between times or places with or without interference.
III: Opinions of experts based on clinical experience. Descriptive studies or expert reports.
A. There are reliable evidence to recommend a clinical prophylactic effect.
B. There are fair evidence to recommend a clinical prophylactic effect.
C. Existing evidence is in contradiction and do not allow
D. There are fair evidence to recommend against a clinical solution.
E. There are reliable evidence to recommend against a clinical solution.
I. There are insufficient evidence (in quantity or quality) to make a recommendation; However, other factors can affect decision making.
Classification
Clinical classification
Classification of the stage of the adhesive process in the laparoscopic picture:
I Stage - Single Slim Spikes;
Stage II - dense spikes, which occupy less than half the surface of the ovary;
III stage - numerous dense spikes, which occupy over half of the ovary surface;
IV Stage - Dense Plate Spikes, which occupy the entire surface of the ovary.
The severity of the adhesive process in a small pelvis correlates with the degree of adhesive process in the abdominal cavity.
Diagnostics
II. Methods, approaches and diagnostic and treatment procedures
List of basic and additional diagnostic events
Main diagnostic measures:
Blood group and rhesus - factor
General urine analysis
Common blood test (hemoglobin, hematocrit, platelets)
Biochemical blood test (total protein, albumin, creatinine, alote, asat, urea, bilirubin (general, straight)
Coagulogram
HIV Blood, Hepatitis, RW
Fluorography of the chest
Grinding
Smear on oncocytology
Consultation therapeuts
Ultrasound of a small pelvis and abdominal cavity
Additional diagnostic measures:
MRI small pelvis
Consultation Surgeon.
Diagnostic criteria:
1) complaints and history - Symptoms of small pelvis, most often manifested in the form of pelvic pain. Depending on the affected organ, the pelvic pain can be given to the area of \u200b\u200bthe rectum, the sacrum, the vagina. In the spikes of the intestine there are pain in the abdomen, most often near the place of operational incision. The character of painful or pulling.
Small pelvic spikes, symptoms can enhance with exercise, movements or change poses. Indicate the intestinal spikes, the treatment of which cannot be postponed, can frequent diarrhea or constipation, vomiting, bloating, postoperative spikes or after inflammation with time "grow" to neighboring organs. After previous laparotomic operations, spikes first can manifest themselves barely noticeable pelvic pains. Spikes whose treatment is not carried out, grow and cause painful feelings In all small pelvis.
When developing spikes in the pipes does not come pregnancy.
2) physical examination
Inspection on the mirrors - the shift of the cervix on the sides;
Palpation of the abdomen - there is pain with deep palpation of the front abdominal wall, the scars on the front wall of the belly, not shifted during palpation, swept with the subjectable tissues;
Bimanual gynecological research is a sharp pain, the uterus shift to the side, the intestinal involvement in the adhesion process, the formation of conglomerates in the cavity of the small pelvis.
3) Laboratory Studies
The smear on the flora of the vagina is the 4th degree of purity of the vagina: the reaction is alkaline, the deterlee sticks are not at all, a large number of coccoints, there may be other types of microorganisms - enterobacteria, bacteroids, leukocytes in a huge amount.
4) instrumental research
OMT and abdominal ultrasound, MRT OMT - anechogenic white trash is noted.
5) testimony for consultation of specialists- Surgeon - a pronounced adhesion process of the abdominal cavity and a small pelvis, the coarse scars of the anterior abdominal wall paved with the subjectable fabrics.
Differential diagnosis
Differential diagnosis
Treatment abroad
Treat treatment in Korea, Israel, Germany, USA
Get advice on medical examination
Treatment
Treats of treatment - Elimination of adhesions, restoration of fertility
Tactics of treatment - Operational treatment with laparoscopic access, separation of adhesions.
Main preparations:
Cephalosporins 3 generations
Ketoprofen.
Tramadol.
Acetylsalicylic acid
Snaropean calcium
Physiological sodium chloride solution 0.9%
H2 receptor antagonists or proton pump inhibitors
Lidocaine
Ropivacaina hydrochloride
Metoclopromide
Gelatin
Phenylephrin
Norepinephrin
Propofol.
Atrakuria Beales
Fentanyl
Atropine Sulfat.
Sevofluran
Diphenhydramine
Additional drugs:
Gentamicin
Cefasoline
Metronidazole.
Meropein 1G.
Other types of treatment: Physical examination, mud.
Surgical intervention:
The treatment of adhesive disease is entirely dependent on the severity of the disease. With acute and intermittent form of the disease, surgical treatment - laparoscopy, is the only method of treatment by virtue high efficiency and quick effect.
With the prolonged distribution of adhesions, therapeutic and diagnostic laparoscopy is shown. As a rule, a surgeon - a gynecologist diagnoses adhesive disease already on the operating table and at the same time conducts operation - dishes and removes spikes.
Perhaps 3 variants of laparoscopy:
Spikes dissect by laser - laser therapy;
Spikes dissect with water under pressure - aquadissection;
Spikes dissect with electrose-electrosurgery.
Alternative laparoscopy methods are used to enter the abdominal cavity in patients with waste and adhesive process:
Methodology using high pressure pneumoperitoneum. After introducing the needle of the versol and creating pneumoperitoneum at 20 - 30 mm Hg. In the deepest section of the navel through a vertical inoperative incision, a short trocar is administered. High pressure The pneumoperitoneum used at the initial introduction of the Troacar is reduced immediately after confirmation of the atraumaticness of penetration into the abdominal cavity. High intra-abdominal pressure significantly increases the distance between the front abdominal wall and large retroperitoneal vessels [UDI II-1 A].
Atypical Troacar Introduction and Double Laparoscopy:the first puncture of the anterior abdominal wall is made in atypical points, i.e. In distance from the navel, using the area of \u200b\u200bthe left hypochondrium - the needle of the versol is introduced in the left upper quadrant on the front axilar line laterally the straight abdominal muscle into two fingers below the rib arc. This choice also helps to avoid the injury of A.Epigastrica Superior, passing through the outer edge of the straight muscle of the abdomen and an anastamosing on the navel level with the lower contractual artery. Then under the control of the telescope introduced into this trocar, choose a space-free place in the aircraft region for a 10 millimeter trocar. It is possible to introduce the needle of the versa in the ninth intercostal in the anterior axillary line, the parietal peritonean in this place is separated from the skin only with a layer of intercostal muscles and fascia, and there is practically no subcutaneous fiber. There is a risk of injury of the diaphragm and the formation of pneumothorax. The contraindications are splenomegaly, inflating the stomach, the tumor of the abdominal cavity. The technique requires an additional puncture and the presence of a 5 mm laparoscope.
Conducting similar manipulations in the right intercoreria is excluded due to the high risk of liver injury [UD A].
Open laparoscopy. Allows avoiding damage associated with the "blind" entry into the abdominal cavity. The procedure lies in the dissection of a small section at the level of the navel of the abdominal wall, overlapping on the aponeurosis and (or) brush the brush and one suture from the edges. After that, trochar is introduced into the abdominal cavity with a blunt way without a style. This method is minilapotomy. This method is relatively safe, but requires a large cut length, which causes the potential risk of the formation of hernia and thorough sealing of the wound. This technique increases the duration of the operation [UD II-2 C]. Fencing trocacares Can be used to decrease input wounds. There is no evidence that they lead to minimal internal damage to vessels during laparoscopic access [UD II-B].
Direct introduction of trocara
The technique is based on the assumption that the complications of the laparoscopic entry into the abdominal cavity are caused to a greater degree in the introduction of the needle of the versol and insufflation of carbon dioxide. A hand surgeon lifts the front abdominal wall, while creating a negative pressure in the abdominal cavity. The first trocacar is carried out through all layers of the anterior abdominal wall in the middle line submbled, then laparoscope is introduced and the surrounding tissues inspect. Advantages: direct access short on 4, 3 min [UD II-2 V].
The traditional entry into the abdominal cavity using the palmer dough is used. This test is designed to determine whether the location of the needle from the battles or intestinal loops as a result of previously transferred operations is free. After the introduction of the needle, the versol abdominal cavity is filled with carbon dioxide. A half-filled with a needle with a needle, an abdominal puncture is carried out next to the needle in the estimated direction of the first Troacar movement, due to increased pressure There is an aspiration of the contents of the abdominal cavity in the syringe. Pure gas shows that the place is free, the absence of aspirate or blood points to the spikes, the turbid liquid indicates the puncture of the intestinal loop. Repeat repeatedly in various places of the front abdominal wall until pure gas is obtained [UD I-A].
Preventive actions:
Regular observation in the gynecologist, timely treatment of urogenital infections, natural family planning: protection against unwanted pregnancy, abortion failure, childbirth through natural labor pathways, regular sex life, careful intervention, use of the anti-barrier (gel), early activation after surgery, physilation .
Further maintenance - On the outpatient stage, physical peace, mud, physical peace for 3-6 months, dynamic observation of a gynecologist's doctor.
Hospitalization
Indications for hospitalization indicating the type of hospitalization
Indications for hospitalization - chronic pain symptom, infertility, chronic pelvic pain, intestinal disorders due to adhesions, hospitalization type - planned .
Information
Sources and literature
- Protocols of the Expert Commission on Health Development Mort RK, 2014
- 1) Philippe Laberge, George Vilos, Jeffrey Demptster, Artin Ternamian. Full Guideline. LaparoScopic Entry: A Review of Techniques, Technologies, And Complications No. 193, May 2007. 2) Adamyan L.V., Mynbaev O.A., Arslanyan K.N., Strugatsky V.M., Kocharyan L.T., Danilov A.Yu. Characteristics of peritoneal adhesions with repeated operations in gynecology // Endoscopy and alternative approaches in surgical treatment of female diseases (gynecology, obstetrics, urology, oncogynecology). Ed. V.I. Kulakova, L.V. Adamyan. M., 2001. - S.533-537. 3) Kumakiri J, Kikuchi I, Kitade M, Kuroda K, Matsuoka S, Tokita S, Takeda S. Incidence of Complications During Gynecologic Laparoscopic Surgery in Patients After Previous Laparotomy.//j Minim Invasive Gynecol. 2010 jul-aug; 17 (4): 480-6. 4) Krasnova I.A., Mishukova L.B., Golovkin N.V., Shtyos S.V., Bresenko N.V. The significance of the ultrasound method of research to diagnose the adhesive process to laparoscopic operations // Laparoscopy and hysteroscopy in gynecology and obstetrics. Ed. V.I Kulakova, L.V. Adamyan. M.: Panter, 2002. - S.509-510. 5) Kondo W, Bourdel N, Tamburro S, Cavoli D, Jardon K, Rabischong B, Botchorishvili R, Pouly J, Mage G, Canis M. Complications After Surgery for Deeply Infiltrating Pelvic Endometriosis. // BJOG. 2011 Feb; 118 (3): 292-8. DOI: 10.1111 / J.1471-0528.2010.02774.x. 6) Merviel P, Lourdel E, Brzakowski M, Garriot B, Mamy L, Gagneur O, Nasreddine A. Should A Laparoscopy BE Necessary in Case of Infertility with Normal Tubes at Hysterosalpingography?.. // Gynecol Obstet Fertil. 2011 SEP; 39 (9): 504-8. By self-medication, you can apply irreparable harm to your health.
- The information posted on the MedElement website and in MEDElement mobile applications, "Lekar Pro", "Dariger Pro", "Diseases: Therapist's Directory", cannot and should not replace a full-time doctor consultation. Be sure to contact B. medical institutions If there are any diseases or disturbing symptoms.
- The choice of medicines and their dosages should be stated with a specialist. Only a doctor can prescribe the necessary medicine and its dosage, taking into account the disease and the state of the patient's body.
- Website MedElement and Mobile Applications "MedElement (Medleylement)", "Lekar Pro", "Dariger Pro", "Diseases: Directory of Therapist" are exclusively information and reference resources. The information posted on this site should not be used for unauthorized changes to the doctor's prescriptions.
- The editorial office of MedElement is not responsible for any damage to health or material damage resulting from the use of this site.
Flashing disease - Permanent companion of any operational interventions in the abdominal cavity. The severity of symptoms depends on the severity and prevalence of the process. It may proceed as asymptomatic and bring significant discomfort to the patient. Some scientists believe that the abdominal surgery in 100% of cases is accompanied by the formation of adhesions, but in the future part of the adhesion is solved independently.
Occasionally there are symptoms of a congenital adhesive process, which is found in newborns, previously not exposed to surgical interventions.
Laparoscopy is considered a new factor that has frequent cases of adhesive disease.
Mechanism for the development of adhesive disease
The peritonese, covering organs of the abdominal cavity, has a property to accommodate damage zones. For example, it happens with an untreated appendicitis, the peritoneum sticks to the zone of inflammation and forms a limited cavity - appendicular infiltrate. Also occurs during operational interventions - the peritoneum sticks:
- to pieces of cut;
- to the operated organ;
- to the zone of inflammation.
In the resolution stage of common inflammatory processes or in chronic inflammation in the abdominal cavity, it usually concerns infectious diseases The uterine pipes and ovaries, the peritonean is diffuse to all organs, disturbing their location and normal functioning. In the future, the formed spikes are compacted and shortened, even more shifting and pursuing the organs and tissues that have fallen into them. In this case, squeezing, feeding organs and tissues, vessels. Normal bloodstream is disturbed and oxygen starvation develops, which causes abdominal pain during adhesive disease. Also, as a result of the displacement and narrowing of the intestinal lumen, the movement of the roaming masses is disturbed, which, in turn, leads to permanent constipation. And in the extreme case, it can lead to the development of such a formidable state, as intestinal obstruction.
The international classifier of diseases of the ICD-10 allocates separate adhesive disease of the abdominal cavity and. In essence, it is one disease, since the small pelvis is also part of the abdominal cavity. This disease is distinguished into a separate category, because the cause of adhesions, most often, are inflammatory diseases of the female genital organs.
The reasons
The reasons for the development of the adhesive process are many, but they are united by one - they all lead to damage to organs or tissues in the abdominal cavity, regardless of which kind of damage.
Let us dwell on the most frequent reasons adhesive process:
- Mechanical injuries of the abdominal cavity:
- strikes, drops from height, falling on a solid object;
- wounded wounds;
- bullet injuries;
- surgical operations;
- Chemical damage:
- burns with acids or alkalis when random or deliberately use;
- sprinkling the stomach with an exit to the abdominal cavity of acidic gastric content;
- severe pancreatitis with the vulnerament of pancreatic enzymes on the abdominal cavity;
- tarve the gallbladder with an influence of bile.
- Inflammatory diseases:
- appendix (appendicitis);
- gallbladder (cholecystitis);
- fine intestine (enteritis);
- tolstoy intestine (colitis);
- pipes and appendages (salpinting, ooforite).
Frequently caused by the development of adhesive disease around the intestine and small pelvic organs is chronic inflammatory process In the female genital organs. Since with low-level symptoms and, accordingly, long flow, it leads to a pronounced and often irreversible process up to infertility.
Related factors - a patient nutrition, diabetes, foreign materials in the wound.
Classification
According to the ICD-10, the spikes of the abdominal cavity are divided:
- Pervian spikes (K66.0), which include:
- abdominal (walls) spikes;
- spikes diaphragm;
- spikes intestines;
- pelvic spikes in men;
- spikes mesenter of thin and / or a large intestine
- spikes of the gland;
- spikes stomach.
- Peritoneal inflammatory spikes in women in small pelvis (N73.6).
- Postoperative spikes in a small pelvis (N99.4).
The whole picture of the disease can be described by triad complaints, which includes the following symptoms:
- abdominal pain;
- constipation and;
- vomiting.
Symptoms of Disease
Of course, not everyone will feel like a person. Depending on the location of the pathological process, the age and duration of the adhesive disease, these symptoms may appear in various combinations. Symptoms are not always found and sometimes discovered only with some random studies, for example, in women in research on infertility.
 Painful feelings in the stomach arise due to the fact that squeezing or explosion of the sector. The intestines peristals and struggles with a non-German. The pain is always long. After all, the spikes are formed gradually. When the spikes compress the intestine, then the intestinal obstruction begins. The pain is first deaf, distant, but then becomes an acute cutting belly. It can be localized in a certain area of \u200b\u200bthe abdomen either over the entire surface. If you do not apply for medical helpThis will exhibit the pathological process and pain will become unbearable. The fear of death appears. Then everything subsides. This means that all nervous endings are destroyed, and irreversible processes began.
Painful feelings in the stomach arise due to the fact that squeezing or explosion of the sector. The intestines peristals and struggles with a non-German. The pain is always long. After all, the spikes are formed gradually. When the spikes compress the intestine, then the intestinal obstruction begins. The pain is first deaf, distant, but then becomes an acute cutting belly. It can be localized in a certain area of \u200b\u200bthe abdomen either over the entire surface. If you do not apply for medical helpThis will exhibit the pathological process and pain will become unbearable. The fear of death appears. Then everything subsides. This means that all nervous endings are destroyed, and irreversible processes began.
Since the intestine continues to work, and the promotion of internal content does not occur due to the obstacle, then this is manifested by vomiting, constipation and. If the adhesive disease affects thin gut, the first symptom with pain will be vomiting. When the pathological process is limited to the colon, it starts with constipation.
Vomiting may be abundant, multiple. The composition of the vomit first includes products eaten on the eve, then gastric and intestinal juices, bile. Vomiting does not bring relief. There is a feeling of gravity in the stomach. Nausea does not leave for a minute. The act of vomiting is painful, since antiperistal waves affect the areas of the non-working intestine, which hurts with greater intensity.
People face constipation in everyday life. Therefore, at the beginning, a person does not pay due attention. Everyone thinks that everything will pass. But constipation in adhesive disease, it's not just constipation! Spikes are increasingly binding the intestines like a web. It violates his work. The dietary masses are in the intestine immobilized and begin to wander. This leads to the formation of a large amount of gases, which can also not go out. There is a bowl of the intestines and the abdomen accordingly. The intestine is stretched, which also causes painful sensations. The patient is trying to go to the toilet as productively as possible, I use several approaches. But everything is in vain. Treatment with laxative and enema does not help either. On the contrary, may aggravate the situation.
Favoring disease can affect the small pelvis organs. In this case, the symptoms may be slightly modified. It is typical for women who have transferred operations in this area and often ill-suffering in inflammatory diseases of the genitals. In the small pelvis in women there is a uterus, a fallopian tube and ovaries. They can be involved in the process. After all, the spikes do not choose who to tighten into their pathological web. As a result, women begin problems with menstruation. They become painful, irregular, up to complete cessation. This is explained by the fact that the uterus is shifted, the pipes are beyond or squeezed, the ovaries twisted. All this requires an immediate appeal for medical care, as it leads to infertility in a launched form.
Surgeons resort to some special methods of preventive treatment during operation, which reduce the spread of the adhesive process around the intestine. These are special gels with enzymes, soluble membranes, special solutions, washing intestines. Also, the prevention of the development of adhesive disease around the intestines contributes: moistened gas with less pressure with laparoscopic manipulations, the use of special surgical gloves without powder, the use of wet tampons when working with intestines, shortening the time of surgical intervention, antibiotic treatment before and after surgery and other measures.
Treatment
Preventive treatment of adhesive disease is preventive measures, undertaken during surgery, such as:
- Use during operational treatment 4% ICodextrin polymer;
- Treatment with carboxymethylcellulose and polyethylene oxide, which create a jelly-like barrier around the intestines;
- Application for the treatment of barrier membranes with hyaluronic acid, cellulose and other materials.
The feature of the adhesive disease is also in the fact that it can develop in a fairly remote period after the operation. If despite all the preventive spike treatment methods formed, they cannot be cured at home. Folk remedies here are powerless. It is not worth going to the signals and psychics. Since you can lose precious time.
When the process began to spread to internal organs, intestines, in a small pelvis and appeared the above complaints to seek medical attention. In this case, there is only surgical methods for the treatment of adhesive disease. Tactics determines the attending physician.
Prevention
After analyzing the causes of adhesive disease, it can be concluded that it is almost impossible to prevent this disease. Partly this statement is true. Nevertheless, some non-surgical causes of the development of adhesive disease can be prevented.
Compliance with a number of simple rules will significantly reduce the risk of the development of adhesive disease in a small pelvis:
- Diseases such as appendicitis, cholecystitis, acute pancreatitis, the peritonitis of the houses are not treated at home. And do not even try to google in search of the best herbal collection. These diseases are treated in the hospital surgeon.
- Chronic inflammatory diseases of the abdominal cavity should also be treated under the control of the doctor.
- Follow your sex health, and this:
- compliance with the rules of intimate hygiene;
- use of barrier methods of contraception;
- maintaining a morally right sex life with one sexual partner;
- regular medical inspection of small pelvis;
- examination on infections transmitted by the sexual way;
- timely treatment of inflammatory diseases of female genital organs.
Dear friends! Medical information on our site is intended only for familiarization! Note that self-medication is dangerous for your health! Sincerely, website editorial
Fast disease - syndrome due to the formation of adhesions in the cavity of the peritoneum due to suffered diseases, injuries or surgical operations, is characterized by frequent attacks relative obstruction of the intestine.
Postoperative adhesive disease traditionally remains the most complex partition of abdominal surgery. The total number of these complications reaches, by literary data. 40% or more. Most of them require re-operational intervention, often much more traumatic and dangerous than the initial operation.
Despite the abundance of special literature devoted to this problem, practical health care has not yet been quite objective, simple and safe methods Diagnosis of such a condition as a bezed disease, as well as effective methods of rational treatment and prevention.
Diagnosis difficulties make it difficult to choose treatment tactics, especially when solving the issue of the need for re-operational intervention. In this issue, the opinions of the authors are fundamentally divided - from the necessary early planned (or software) relaparotomy and open maintenance of the abdominal cavity (lapostomy) before the use of late relaparotomy. At the same time, all clinicians converge in a single opinion that relaparotomy refers to the category of surgical interventions with high degree The operational risk of patients performed in the most complex and weakened contingent. This in turn determines the mortality rates after such operations, according to various data from 8 to 36%.
It should be noted that the absolute majority of practical surgeons remain on the position that the adhesive disease should be treated by wide relaparotomy. At the same time, the intersection of squeezing, and the separation of interchekt battles in intestinal obstruction, of course, saves the life of the patient, but inevitably provokes the formation of adhesions even more. Thus, the patient is at risk a re-operation, increasing with each intervention.
An attempt to break this vicious circle has become the proposed NOBLE intestine sling with the help of serous muscular seams, designed to prevent the random location of intestinal dishes and obstruction. Due to the large number of complications and bad remote results, this operation is now practically not used.
The methods of conservative impact on the pathogenesis of postoperative insufficient disease are also not developed for prevention and treatment.
Flash disease is a pathological condition due to the formation of adhesions in the abdominal cavity after operations, injuries and in certain diseases.
Fast disease can be two forms:
- congenital (rarely) as an anomaly of development in the form of plane interchesships (linen) or battles between the parts of the colon (Jackson membrane);
- acquired after operations, injuries with hemorrhages in a visceral leaflet of peritoneum, peritonean inflammation (viscerite, peritonitis, transient processes with inflammatory peripoches of internal organs).
Code of the ICD-10
- K56.5. Intestinal combustion [spikes] with obstruction.
- K91.3. Postoperative intestinal obstruction.
What causes adhesive disease?
After the operations of the formation of the pathological process in the abdominal cavity contributes to a long part of the intestines, the presence of tampons and drainage, entering the abdominal cavity of irritating substances (antibiotics, sulfonamides, talc, iodine, alcohol, etc.), blood remnants, especially infected, irritation of peritoneum during manipulations (for example, not to miss the exudate, but wiping it with a bottle).
The prevalence and nature of the pathological process can be different: a limited zone of operation or inflammation, sometimes a lifting the whole floor of the abdominal cavity, more often the cavity of the small pelvis; In the form of a soldering of an inflamed organ (gallbladder, intestine loops, stomach, gland) to the front abdominal wall; in the form of separate heavy (extrud) attached in two, points and squeezing the intestinal loop; In the form of an extensive process, exciting the entire abdominal cavity.
How does adhesive disease develop?
Fast disease is a very complex pathology, it is impossible to solve it without a clear understanding of the processes occurring in the abdominal cavity.
According to modern researchers, protective cell processes, initiating various intraperitone damaging moments - surgery, injury, inflammatory processes of various genes are developing with the direct participation of the main "generators" of inflammation cells - peritoneum and large glands. It is they who provide the greatest value from the point of view of phylogenesis of cellular protection mechanisms.
In this issue, monocyte derivatives - peritoneal macrophages should be stopped. We are talking about the so-called stimulated peritoneal macrophages, i.e. Phagocytes belonging to the inflammatory exudate of the abdominal cavity. In the literature, it was shown that in the first hours of the inflammatory response to the abdominal cavity, they are mainly neutrophilic leukocytes, and by the end of the first or the beginning of the second day in the exudate migrate monocuclears, activating and differentiating into peritoneal macrophages. Their functions are determined by the ability to intensively absorb various biological substrates and actively participate in the catabolism of the intraperitoneal process. That is why the state of macrophage reactions in the pathogenesis of adhesive disease can be considered indisputable.
When studying the state of protective cellular reactions in humans, the method of studying aseptic inflammatory response (AVR) in the "skin window" is most inflammatory.
To implement this study, the scarified surface of the study is superimposed and secured the sterile slide glass to remove the prints after 6 and 24 hours, thus obtaining the cell material of the first and second phases of the AVR. Subsequently, they are painted and studied under a microscope, evaluating the timeliness of the phase change (chemotaxis), the percentage cell composition, the quantitative relationship of various elements and cytomorphology.
Studies conducted on this technique showed that healthy people In the first phase of AVR, neutrophils are an average of 84.5%, and the macrophages - 14% in the second phase of the AVR observe the opposite ratio of cells: neutrophils - 16.0%, and macrophages - 84%, eosinophils do not exceed 1.5%.
Lymphocytes do not detect at all. There are no deviations in the indicated sequence of the output and the percentage ratio of cells indicative of the violation of the cellular mechanisms of protection.
Recently, clinical and experimental studies have appeared, which state that the adhesive disease - the result of the exchange of exchange connective tissue, in particular collagen. The stabilization of collagen chains is carried out with the participation of copper-containing enzyme lisocidase, catalyzing the conversion of lysilodeneoxylizin in aldehyde. These aldehydes, in turn, form transverse covalent bonds, forming a three-speech molecule of insoluble mature collagen. The activity of lisocidase is directly related to the activity of N-acetyltransferase - a constitutional enzyme that catalyzing the process of inactivating toxic products of metabolism and brought from the outside of ligands.
It is well known that the human population of N-acetyltransferase activity is divided into so-called "fast" and "slow" acetylants. At the same time, slow acetyologists include persons with acetylation percentage of less than 75, to rapid acetyologists with a percentage of acetylation exceeding 75.
The process of the regeneration of peritoneum The formation of collagen fibers in individuals with different speed of acetylation occurs differently.
- Slow acetylants accumulates acetylation substrates (endogenous and exogenous chelate complexes), which bind copper ions that are part of the linesidase. The synthesis rate of cross-links is reduced, the number of generating fibers is small. The accumulating laterant collagen on the principle of feedback activates the endogenous collagenase.
- Fast acetyluoris accumulation of acetylation substrates does not occur. Meli ions are not associated, Lysiloxidase activity is high. The active synthesis and the deposition of collagen fibers on the existing fibrin embedding occurs. In these fibers, in turn, fibroblasts are deposited, which perverts the normal course of peritoneum regeneration and leads to the formation of adhesive disease.
The adhesive disease develops due to the presence of a causal relationship between cytodynamic, cytomomorphological shifts of the normal course of local and general cellular reactions of protection under the disorders of the reparative synthesis of collagen.
These complications in clinical practice are represented by such states as: early intestinal obstruction (RSNA), late intestinal obstruction (PsNK) and adhesive disease (Sat).
Based on the above, in patients who have adhesive disease, a comprehensive study must be carried out, including phenotyping by acetylation rate, the study of cytodynamic processes and cytomomorphology of phagocytic cells in the peritoneal exudate (local cellular reaction), in the "skin window" on the reboot (total cellular cellular reaction). The verification of the data obtained must be carried out by the methods of ultrasound echography (ultrasonography) of the abdominal cavity and video transcomps.
The adhesive disease is characterized by the presence of changes in the parameters studied characteristic only for the specified pathology.
Citodamic reactions in the postoperative period in these patients had its own characteristics both in the peritoneal exudate and in the prints of the "skin window". Thus, in the peritoneal exudate, a reduced amount of macrophage elements was observed, during the ABR - a disorder of macrophage chemotaxis and increased content of fibrin fibers in the "skin window" wound. The average speed of acetylation in children with RSNK was significantly higher than patients with a favorable flow postoperative period, and amounted to; 88,89 ± 2.8% (p
The results of studies have allowed to come to the following conclusion.
If the operational intervention on the abdominal organs is performed in a child with a phenotype of fast acetylation and, at the same time, it has a lack of a macrophagum reaction, due to a violation of the chemotactic activity of mononuclear phagocytes, then, on the one hand, reinforced fibrinetsis and accelerated collagen synthesis will occur due to intensive proliferation of fibroblasts. , ahead of the speed of normal catabolism of fibrin, and on the other hand - an inadequate macrophagum reaction, perverting inflammation kinetics, which will lead to a long permissance of peritoneous degradation products, caused by the body sensitization of tissue decay and the formation of hypersensitivity slowly type, chronic immune-based inflammation with the attraction of an even more : Quantities of fibroblasts in the hearth focus. Thus, all marked processes in aggregate will lead to an excessive synthesis of connective tissue - the formation of such a state as a adhesive disease. It should be noted that the concomitant pathology gastrointestinal tract Multiplely increase the risk of pathological fibrinetsis.
How is the adhesive disease manifest?
The clinical flow differs acute intermittent and chronic adhesions.
Acute form is accompanied by a sudden or gradual development of pain syndrome, enhancement of peristaltics, clinic of dynamic intestinal obstruction, which is mostly possible to be allowed. Growing pain and change in their character on constant testify to the development of mechanical obstruction.
The intermittent form is accompanied by periodic attacks, which are accompanied by different pains, dyspeptic disorders, constipation, replacing diarrhea, discomfort. As a rule, it is found with limited pathological processes. The intestinal obstruction is rare.
The chronic form manifests itself with a stomaching pain, a sense of discomfort, constipation, weight loss, attacks of dynamic intestinal obstruction, but a mechanical form of obstruction can develop.
How is the adhesive disease recognize?
The diagnosis is based on a dynamic x-ray study of the passage of the barium suspension in the intestines, sometimes resort to irrigoscopy if a thick intestine is involved in the process. Simultaneously with the determination of the nature of the intestinal deformation and the presence of an obstacle to the passage of intestinal content, the relief of the mucousa is determined:
This is necessary for differential diagnosis with intestinal cancer and carcanomatosis.
The adhesive disease is characterized by deformation of the relief of the mucous membrane, but it is not interrupted as during cancer. In doubtful cases, laparoscopy perform, but during the period of exacerbation, it can represent certain difficulties, and even the danger of damage to bloated intestinal loops.
The success of the treatment of patients with postoperative adhesive disease depends largely on timely diagnosis. Well-known and widely used diagnostic methods do not always lead to the desired results, prompted clinicians to develop a comprehensive diagnostic program for predicting this pathology. This program includes the use of a chemical method for determining the type of acetylation of a particular patient, pathological techniques for the study of local and general cell reactions, an ultrasound of the abdominal cavity, traditional x-ray examination, laparoscopy.
Ultrasound diagnostics in suspected adhesive disease apply the terms of use of modern equipment. It allows you to get a characteristic echographic picture practically non-invasive.
However, it should be remembered that with ultrasound diagnosis of intestinal obstruction due to adhesive disease, it is impossible to navigate only on a static picture. More reliable data is obtained when carrying out echoscopy in real time, which makes it possible to identify the translational movement of particles in the intestinal tube in the norm and the phenomenon of reciprocating - with signs of mechanical intestinal obstruction. This phenomenon was revealed almost in all patients and called the "Symptom of Pendulum". However, with all the informativeness and the possibility of ultrasound diagnostics, they are largely limited to the accompanying phenomena of the intestinal car. To solve this problem, a method for differential diagnosis of mechanical and dynamic intestinal obstruction was developed. For this purpose, an ultrasound of the abdominal bodily organs perform, in which extended loops of the small intestine are visualized, filled with liquid content, which indicates a violation of the passage through the intestinal tube. Neostigmine methyl sulfate in the age dosage, followed by percutaneous intestinal electrostimulation and re-conduct echographic examination. If a reduction in the intestinal lumen and the translational movement of particles occur as a result of the stimulation carried out, it is safe to reject the diagnosis of mechanical intestinal obstruction and treat the patient conservatively. With mechanical obstruction
After stimulation is enhanced painfulnessIt often occurs vomiting, with a echographic study of the loop of the intestines, they are not reduced in size, mark the progressive movement of Himus - the "pendulum symptom", which allows diagnosing mechanical intestinal obstruction and formulate readings to its surgical resolution.
A rather characteristic picture of the x-ray diagnosis of intestinal obstruction (in the form of both overview radiographies of the abdominal cavity and x-ray radiographic studies with bariratory slust) is well known. In this regard, with all due respect to the old test method, it should be mentioned negative parties: a radiation load, the duration of the diagnostic process, difficulty in the differential diagnosis of dynamic intestinal passability from mechanical.
How is the adhesive disease treat?
Speaking about the methods of treatment of both early and late postoperative adhesions, should be indicated by the failure of unification in the problem
the choice of therapeutic tactics in this pathology. In this part of the solution to the problem, the principle of a differentiated approach, depending on the presence of a specific clinical form Postoperative complication.
At the same time, the first priority should be considered the desire to avoid broad laparotomy, and in the case of absolute testimony to surgical treatment, to achieve cure with the help of endosurgical intervention or minilapotomy.
Speaking about the treatment of children who have adhesive disease, the following should be noted. It is well known that so far all clinicians, with rare exception, were trying to get away from the operational treatment of children with adhesive disease, especially without obstomability phenomena, preferring conservative treatment methods, usually ineffective.
At the present stage, therapeutic tactics should be made up of active identification of children with adhesive disease, preoperative treatment, and then complete elimination of the adhesive process in the abdominal cavity with laparoscopic technology.
Indications K. surgical treatment Faving diseases include the following symptom complex:
- Frequent pain attacks accompanied by intestinal obstruction phenomena (vomiting, stool delay and gases).
- Recurient abdominal pains, especially when jumping and running (symptom of nod, or "stretched salinity").
- Intensive abdominal pain, often accompanied by vomiting arising after a diet violation in the form of overeating.
- The phenomena of complete intestinal obstruction allowed in the process of holding conservative events.
Naturally, the basis and pledge of the subsequent success here is the methods of diagnosis, which was discussed above. Moreover, the components of this diagnostic program make it possible not only to establish the presence of such a state as the adhesive disease, but also to determine the differentiated subsequent treatment tactics. Based on the foregoing, all rapid acetyologists should be prescribed preoperative preparations aimed at transformation of adhesions in order to reduce the trauma of subsequent laparoscopic intervention and prophylaxis of restoration of adhesive disease.
Fast sickness is treated as follows. In parallel with the examination of the patient in terms of preparation for surgery on the abdominal cavity, Penicillamin is prescribed in the age dosage 1 time per day during reception (preferably during lunch). Mandatory components of treatment - drugs. Normalizing intestines (bifidism bifidobacteria, bifidobicteria bifidum + intestinal sticks), and vitamin E as antihypoxant. Other drug therapy is used only to correct any pathological shifts discovered in the survey process. At the same time, physiotherapeutic procedures are carried out, consisting in phonophores with the ointment of Iruksol on the front abdominal wall. Depending on the intended degree of prevalence and the timing of the existence of adolescent disease, the course of preoperative treatment usually takes from 10 to 12 days. If there is a full-fledged polyclinic service at the place of residence of the patient, the specified treatment can be carried out outpatient.
Upon completion of the preoperative examination and treatment, therapeutic laparoscopy is performed, in which the prevalence of adhesive disease is finally estimated, the positive effect of the preoperative drug preparation has been noted and the separation of adhesions is carried out.
First of all, it is necessary to eliminate the spikes between the parietal visceral peritoneum. In this case, most of them are usually separated by a blunt way and almost bloodlessly.
Only separate long-term existing and well-vascular spikes should cross the sharp after electrocoagulation, using exclusively bipolar tools. In the future, they spend a thorough audit aimed at detecting intercircuit strips, which also need to be eliminated. Separate intercircuit flatness, not causing intestinal obstruction phenomena, is permissible to separate because they do not determine any pathological phenomena in the future.
The procedure is completed by the final audit of the abdominal cavity to evaluate the resulting result and verification of the usefulness of hemostasis, after which the gas of the pneumoperitoneum is evacuated, laparoscopic ports are removed and sewn.
As a rule, on the 2nd day of the postoperative period, children in the stomach pain practically do not experience, begin to walk in a short time (5-7 gut) are issued home.
In the katamase of patients inspect 1 week. 1, 3, 6 months and 1 year. The peculiarities of this katamnestic group should include a tendency to the development of intestinal dysbacteriosis and various gastroduodenal pathology in the form of gastritis and gastroduodenitis, which requires additional participation of the gastroenterologist in the observation of these children.
It should also be noted that a small clinical group of patients (slow acetylasts) does not require preoperative treatment, since they have adolescence due to the fixation of the free edge of the large gland to the front abdominal wall in the projection of laparotomous access or to the intestinal hinges during operational intervention due to previous intraoperative technical technical Error. Such patients should be carried out by a laparoscopic operation 2-3 days after entering the hospital. Performing a larposcopy on the already described methodology, it is necessary to determine the location of the large gland, coagulate it along the alleged intersection line, and then cut off endosurgical scissors. Children from this group are usually prone to relapses, and therefore special treatment Do not require.
How is adhesive disease prevented?
Speaking about how adhesive disease is prevented, it should be given due to the opinions of many authors who believe that these events should begin during the fulfillment of the first operational intervention. Adequate operating accessories, gentle, delicate manipulations with tissues and abdominal organs, strict adherence to the rules of aseptics and antiseptics significantly reduce the risk of pathological spike formation, but do not eliminate it completely.
The prevention of the RSNK is very promising when using information obtained in the process of comprehensive study of this problem. As mentioned, two conditions are necessary for the development of this complication: a rapid acetylated phenotype and an inadequate macrophage reaction. Thus, exploring the parameters in patients in the first day of the postoperative period, it is clearly distinguished by a group of patients threatened by the development of RSNK.
If the likelihood of the development of the RSNK in a particular patient is predicted, it should be prescribed prophylactic treatment, including preparations of penicillamine in the age dosage 1 time per day for 7 days, Prodigiosis 0.005% solution in the age dosage - 3 intramuscular injections every other day, vitamin E inward 3 times Day and ultrafonophoresis on the front abdominal wall with the Mazus "Iruksol" (bacterial collagenase-clostridopeptidaea A).
PSNC prevention should be considered mandatory dispensary observation Behind the children who moved surgery on the abdominal organs. Moreover, than with large technical difficulties or with large pathological changes in the abdominal cavity, there was an operational intervention, the more thoroughly it is necessary to carry out postoperative control in order to identify such a pathological process, like adhesive disease and eliminate it before the occurrence of intestinal obstruction.
The most full-fledged results gives the inspection of patients using ultrasonography in terms of 1 week, 1.3, b m and 1 year after the operation on the abdominal cavity. Clinical experience shows that the risk of early postoperative intraperous complications are most large among children with rapid acetylation phenotype in the presence of inadequate cellular reactions of inflammation and peristine's vanishing reparation. In this regard, in patients, underwent operations on the abdominal cavity, especially accompanied by significant trauma and peritonitis, in the postoperative period, it is necessary to carefully investigate the aforementioned indicators.
In the presence of data indicating the disorders of cytodynamics and cytomomorphology, especially in "fast acetylants", it is necessary to carry out the above prophylactic treatment.
The entire complex of described preventive measures reliably protects patients with an abdominal surgeon from such a state as a adhesive disease.
Content
People who have undergone operations on the internal organs often appear painful symptoms. They arise in the abdominal cavity, the organs of the small pelvis. The causes of the intestinal disease may be injuries, violation of the integrity of the organs. In gynecology, symptoms are associated with inflammatory processes, hormonal diseases. It causes all this adhesive disease of the abdominal cavity. Its appearance can lead to serious consequences - intestinal obstruction, and in women - also to infertility.
What is spikes
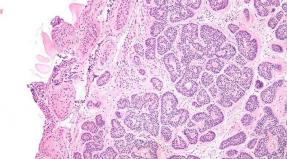
After inflammation or operational interventions, seals appear, which connect internal organs among themselves. They are called spikes. It seems to resemble a thin film, or a strip fiber. Education is hampered by the normal operation of the organs. A dangerous health situation is created. Because of pathological processes in the digestion system, the intestinal obstruction arises. As a result, in serious cases there are disability and fatal outcome. Fast processes of small pelvis organs lead to infertility. So the spikes look in the photo.
Symptoms of adhesive disease
By international Classification The ICD-10 is isolated for adhesive disease of a small pelvic and abdominal cavity. Sometimes there are no symptoms and are determined by accident on ultrasound. This is especially characteristic of gynecology, where often the cause of adhesions are inflammation and infections. With the diseases of the lungs, another situation occurs. Appeated pleurodiaphragmal spikes to determine difficult. They do not have symptoms, but do not affect well-being - therefore they are not treated. Such formations are connected to a diaphragm with the lower part of the lung. Common symptoms of adhesive disease include:
- pain;
- constipation;
- vomiting;
- temperature increase.
Intestine
Spikes in the intestines appear after surgical operations. May pass asymptomatic, but sometimes manifests themselves very bright. Most dangerous sign - intestinal obstruction. Due to strong prolonged pain, the absence of a chair, the sweat of the belly appears fear of death. The symptoms of the adhesive process are:
- painful vomiting;
- gravity in the stomach;
- flatulence;
- constipation.

Adhesion process in small pelvis
The symptoms of the appearance of adhesions in a small pelvis differ little from the manifestations of gynecological diseases. Especially difficult to determine that the reason is more often linked in inflammatory processes, hormonal diseases. Spikes cover the appendage organs - ovaries, uterine pipes and the uterus itself. Such a state leads to ectopic pregnancy, infertility. Symptoms of the adhesive process:
- bleeding;
- many pain in the lower abdomen;
- reduced pressure.
On ovaries
Spikes on the ovaries arise as a consequence of inflammatory processes, injuries conducted by operations. They appear after taking antibiotics, ignitions of erosion. Symptoms of adhesive disease on the ovaries:
- impairment of the menstrual cycle;
- painful monthly;
- pain in the lower back, at the bottom of the abdomen;
- ectopic pregnancy;
- sex pain;
- infertility.
In the uterus

The appearance of adhesions in the uterus is connected with abortion and scraping epithelium. After conducting operations on the mucous, the connecting tissue begins. Healthy endometrium is dying, formation is connected among themselves the walls of the uterus. This leads to a violation of the menstrual cycle. Monthly becomes scarce or missing at all. Everything is accompanied by strong, painful pains. Leads to frozen pregnancy, infertility.
In trumpet
Peritabar spikes are formed from the outer side of the uterine pipes, capable of bringing them obstruction, as a result - infertility. Appeal after inflammatory, infectious diseases. The peculiarity is that there are no special symptoms. Women write off their uncomfortable condition for stress, fatigue and do not turn to the doctor. Begin to beat the alarm when they can not get pregnant. Spikes are discovered during a survey associated with infertility.
Causes of adhesions in the abdominal area
More often, adhesions are associated with operational intervention. In gynecology, it may be abortions, cesarean section, rapid birth. In addition, among the causes of adhesive disease:
- abdominal injuries;
- injuries;
- appendicitis;
- acute pancreatitis;
- damage to the gallbladder;
- internal bleeding;
- inflammatory processes in organs;
- hormonal diseases;
- sex infections.

Diagnostics
In case of adhesion of the abdominal cavity, the diagnosis begins with an external examination of the patient. The doctor produces a survey of symptoms, the character of pain. General analyzes are assigned. In the spikes of the intestine produce a finger survey of the rectum. More accurate diagnosis is carried out using ultrasound examination, radiography. What are prescribed:
- In gynecology, diagnosis is carried out using an ultrasound, magnetorezonance tomography (MRI).
- Laparoscopic examination gives accurate diagnostics. He is prescribed in difficult cases.
- With spikes in the uterine pipes, a special contrast is introduced, a X-ray is made. Check how much obstruction is common.
- Another diagnostic method involves the input of a physiological solution along the cervical channel and inspection using an ultrasound.
Treatment of guns

In case of adhesive disease of the abdominal cavity, treatment begins with prevention during operations. Special substances are used that fill the space around the intestines, the connective tissue is not allowed. If postoperative spikes occurred, then for treatment use:
- medical preparations in the form of tablets, injections, candles;
- physiotherapy;
- medical physical education;
- folk methods;
- diet;
- operational intervention.
In gynecology
Treat spikes in a small pelvis begin with the use of drugs. It is not always the reason for the appearance of surgical intervention. If the formation of adhesions is caused by infectious diseases - treat antibiotics. With inflammatory prescribed non-steroidal anti-inflammatory drugs. To remove spikes on the ovaries and the uterine pipes, enzymes use that help their resorption: "Lidase", "Longidase". Effectively physilation electrophoresis with medicines.
A vibrating massager is used for squeezing of adhesions. Prescribed therapeutic physical culture, a special diet. Folk remedies helps to get rid of - dyeing with a decoction of Badan. Surgery comes to help with acute form Diseases or when the remaining methods are powerless. Laparoscopy helps to cure disease. Dissection of adhesions with a laser, aquadissection. Fully removal is performed using electrosurgery. This gives women hope for pregnancy.
Intestinal
The treatment of intestinal adhesions starts with physioprocessed. Laparoscopy is very effective when it is possible to see and neutralize education. To hold it on the body there are three small holes for the probe. Spikes are caught with a laser, either or removed completely. When there are many of them and they have large sizes, dissect the front wall of the peritoneum and make the operation.
Diet with intestinal adhesion

One of the methods of treatment of the intestinal adhesive is to comply with the diet. It is necessary to exclude irritating stomach and intestines. Products: sharp, sour, with coarse tissue. Food should not cause gaspace. It is not allowed to use:
- drift;
- carbonated drinks;
- spices;
- confectionery;
- hot and cold food;
- smokers;
- sweets;
- sausage products;
- alcohol;
- fried.
It is advisable to eat small portions, thoroughly chewing food. Power must be fractional - at least 5 times. More useful meal prepared for a couple. It should be eaten:
- vegetarian, dairy soups;
- non-fat meat;
- fish;
- lactic acid products;
- porridge on water;
- black, white bread;
- ripe fruits, berries;
- greens, vegetables;
- tea with milk, juices.
Video: Spike exercises
Attention! The information presented in the article is familiarized. Article materials do not call for independent treatment. Only a qualified doctor may diagnose and give recommendations on treatment, based on the individual characteristics of a particular patient.
Found in the text error? Highlight it, press Ctrl + Enter and we will fix everything!Discuss
Bashes of the abdominal cavity - prevention and treatment. Symptoms of adhesive disease of the abdominal cavity, diet
Differential diagnosis is carried out with a mecosis, stenosis of the terminal deposition of the ileum, dynamic intestinal obstruction, megacolon, familiar constipation, endocrinopathy, hypovitaminosis in 1.
With the imparency of the intestines associated with enterocolitis, apply antibacterial therapy And daily enemas with isotonic solution. The relief of enterocolithic phenomena leads to the disappearance of obstruction. Radical and mandatory operation (Fig. 8-5, d) precede conservative treatment: Lightweight diet, cleansing and siphon units, symptomatic therapy.
The forecast is favorable with rectal form and timely operational intervention.
K66.0. Abdominal peritoneal spikes (walls), intestines, mesenter, adhesions.
Bashes of peritonean - syndrome due to the presence of adhesions in the abdominal cavity and characterized by frequent attacks of intestinal obstruction arising, as a rule, due to surgical interventions on the abdominal organs and the differing variety clinical manifestations.
Recently, there is an increase in the prevalence of adhesive sickness (SBB) and adhesive intestinal obstruction (SCN) among other types of Ileus in children.
Surgical interventions on the abdominal cavity are the immediate cause of adhesions. Any inflammatory process in the abdominal cavity as a result of injury to peritoneum and exposure infectious agent leads to an activation of an immune response with the participation of inflammatory mediators, cytokines, immune cells, resulting in pathological immune complexes. These complexes are attached to healthy tissue cells and cause activation of the complement system. Cytotoxic reactions caused by their activation lead to damage to the tissue and the stubborn flow of the inflammatory process, accompanied by the proliferation of the connective tissue, thereby contributing to the enhancement of the adhesive process in the abdominal cavity.
SBB classification (Gataullin N.G., 1978) is based on the clinical course of the disease, taking into account its gravity and allows you to determine the most convenient tactics of patients.
It highlighted 4 forms of the disease:
Latent asymptomatic SBB form;
Adhesive disease with a predominance of pain syndrome;
Adhesive disease with a predominance of discomfort in the gastrointestinal tract;
Table 8-2. Main forms and clinical manifestations of SBB
Fig. 8-6. Forms of SKN in children (according to Bairova G.A., 1983)
The clinical picture of adhesive disease and adhesions of the abdominal cavity variabella. It consists of symptoms caused by the severity of the overall condition of the patient, and local manifestations (Table 8-2). Properly assembled anamnesis, In which a particular importance is given to the identification of previously inflammatory processes and operational interventions on the abdominal organs, as well as the prescription of the disease, are leading in diagnosis.
It is important to properly carry out the palpation of the abdomen in order to identify some characteristic symptoms, the mechanism of which is based on the principle of viscesencensor reflexes and is associated with the appearance of painful sensations when stretching adhesions:
- symptom Publine - pain in the rubar when tilting the body forward;
- symptom Androsov - pain in epigastrics with deep palpation of the hypogastral region;
- symptom of Huanafina - The appearance of pain in artificial inflating belly (with spikes of any localization).
When developing acute SCNs, in addition to sharp, grapple pains, vomiting stagnant content, the blown of the abdomen, the latency of the chair and gases, the abdominal asymmetry, visible peristaltics of intestinal loops on the front abdominal wall, the noise of the splash, the noise of the falling drop.
In the later dates, peritoneal phenomena, fever, neutrophilic leukocytosis, sharp rise in ESP are joined.
The leading role in diagnostics belongs to X-ray research. The main symptoms of the SBB, detected in the overview radiograph of the abdominal organs (Fig. 8-7, a):
Uneven distribution of gases in intestinal loops;
Clamps of Cloible and Arches, allowing to determine the level of intestinal obstruction.
However, direct signs allowing to determine the size, view, localization of adhesions, this method There are no studies.
A more informative recognized method of x-ray study of the GTS with contrasting with a sulfuric acid barium. The time of the appearance of a contrast agent in the blind intestine in terms of the reception of the barium suspension per OS. Reveal indirect signs The adhesive process (Fig. 8-7, b):
Fixation of intestinal loops to the front abdominal wall, postoperative logging or other organs;
Conglomerates loops of the small intestine with an uneven speed of evacuation of a contrast agent;
The narrowing of the segments of the small intestine, the expansion and thickening of the intestine of the intestine above the adhesions, the formation of false diverticulus in the small intestine due to its spikes.
Promising and most informative method for diagnosing SBB is diagnostic laparoscopy (Fig. 8-7, B).
The fight against the adopted spikes of the abdominal cavity to date remains difficult and to the end of a not solved problem of abdominal surgery. In practice, most of the operations are performed in an emergency in the event of a situation threatening the patient's life.
Fig. 8-7. SBB: a - overview radiograph of the abdominal organs; B - X-ray-contrast study of the gastrointestinal tract in direct projections; B - laparoscopic picture; M - dissection of coagulated spike
Depending on the clinical manifestations of the disease (from an isolated painful syndrome to a pronounced picture of SCN), the decompression of the tract is used by introducing a nasogastric probe and washing of the stomach, blockades, hypertensive compresses on the front abdominal wall, drug stimulation by administering anticholinesterase products, cleansing and hypertensive enema, decrease pain syndrome by introducing spasmolitics.
These events allow you to stop intestinal obstruction without surgery. The timing of conservative treatment is determined within the reach of the overall state, daughter can be extended.
With the ineffectiveness of conservative treatment and a pronounced picture of the SKN question about surgical intervention It is definitely solved. In diagnostic laparoscopy, it can go to therapeutic when confirming the presence of adhesions in the abdominal cavity. This operation is called laparoscopic adhesiolysis. It is not enough invasive, allows you to maximize the trauma of operational intervention and improve the remote results of SBB treatment. The essence of the operation consists in visualization of adhesions of the abdominal cavity and their coagulation, followed by dissection (Fig. 8-7, d).
In daily surgical practice, compliance needed principles of nonspecific intraoperative prophylaxis Spike formation, i.e. Reducing the invasiveness of interference, injury, tissue ischemia.
Special (private) Prevention methods Provide the appointment of drugs operating in different directions:
Fibrinolytic enzymes (streptinate, urchinase, collagenase, etc.);
Proteolytic enzymes (tripsin, chymotrypsin, etc.);
Anticoagulants (low molecular weight heparin);
Anti-inflammatory drugs (antibiotics);
Nonspecific desensitizing agents (antihistamine drugs);
Hyaluronidase preparations (lidases).
In addition, in the postoperative period, the Patients of the Risk Group of SBB development need to prescribe preparations that slow down the synthesis of collagen and reinforcing its disposal. In a complex with conventional anti-inflammatory therapy, it is necessary for the prescription of penicillamine (Coopened *) inside from 3 days after surgery in the next dosages: up to 5 years - 0.15 g; 5-12 years old - 0.3 g; Over 12 years old - 0.45. In order to destroy and dispose of collagen fibers, phonophoresis of collalizin is carried out at the same time from 2-3rd days after the operation of Posässa.
To prevent the development of the postoperative passer in the intestine, electrostimulation, igloreflexotherapy, prolonged blockade of the reflexogenic zones of the abdominal cavity, hyperbaric oxygenation are used.
An important point is the awareness of the patients and their parents regarding the clinical course of the SBB and the need for medical advice in order to early diagnosis Diseases and warnings of SCN and other complications.
After transferred surgical treatment and discharge from the hospital, all patients must be taken to dispensary account With regular inspections at least 2 times a year. Recommend the implementation of rehabilitation measures aimed at increasing the general resistance of the body to prevent inflammatory diseases.
The forecast is unfavorable in the case of late operational intervention with SCN, mortality at which can be 5-7%. In the course of a long flow of the adhesive process with frequent recurrences of intestinal obstruction, persistent disability of patients may develop.
Bashes of the abdominal cavity: code on the ICD-10, symptoms, treatment, diet, folk remedies
Forms
- Purchased. Developing as a result of surgical operations, inflammatory diseases of the perigests (peritonitis, viscerite, periprocesses of internal organs) or its traumatic damage, accompanied by hemorrhages in the visceral leaf area.
Code of the ICD-10
Peritoneal spikes in women localized in the field of small pelvis are attributed to the XIV class, including diseases of the urogenital system, under the code N73.6. For postoperative peritoneal pelvic spikes in women, the code N99.4 is fixed.
Causes of the disease
- surgical interventions;
- strong blows;
- bullet wounds;
- koloto-cut wounds.
Acute form always starts suddenly. The patient has severe abdominal pain. Against the background of gradually reinforcing intestinal peristals, vomiting develops and an increase in body temperature occurs. A common blood test taken at this point will indicate the presence of leukocytosis and an increased erythrocyte sedimentation rate.
- Constant thirst.
- Tachycardia.
- Arterial hypertension.
Diagnostic methods
- infectious pathologies.
Electrogastrography - electrophysiological studies of gastric peristaltic by registering the stomach biopotentials. To implement this procedure, the electrodes are either implanted into the wall of the stomach, or attach to the skin cover of the front wall of the abdomen.
Bashes of the abdominal cavity
The beginning of the formation of adhesions between the loop of the small intestine
- timely execution of operational intervention acute diseases abdominal organs without the use of coarse drainage and tampons;
- washing the abdominal cavity, sometimes - carrying out peritoneal dialysis;
- intensive antibiotic therapy on the background and after surgery - the drugs of the choice are antibiotics of groups of tetracycline, cephalosporins, sulfanimides;
- the use of anticoagulants (heparin, fraxipart), prednisone with novocaina;
- stimulation of intestinal motorcycles (prozerne);
- the use of fibrinolytic drugs (preparations dissolving fibrin, around which spikes are formed) - chymotrypsin, trypsin, fibrinolysin, streptocinase, urocinase.
Indicators of the electric strooperogram in a patient with adhesive disease
Flashing: Forms, Signs and Treatment Methods
Fast disease is called a pathological condition due to the occurrence of dense connective tissue structures (heavy) between the peritoneum and internal organs.
All sorts of inflammation and traumatic damage to the peritoneum can be an impetus for the development of adhesive disease, as well as surgical operations on the abdominal organs.
The formation of adhesions is protective reaction The body trying to protect the healthy organs from damaged structures by forming a white adhesive tank with a high fibrin content.
The main purpose of this sticky of the connective tissue film is to glue the adjacent surfaces, which helps limit the lesion zone. As the inflammatory process is raised, more dense structures that connect the peritone with the internal organs can form in the places of formed.
Thinking and significantly limiting the mobility of internal organs and blood vessels of peritoneum, spikes over time are increasingly compacted and shortening, creating conditions for the occurrence of dangerous diseases ending, for example, female infertility or complete intestinal obstruction.
The inflammatory process in the abdominal cavity does not always lead to adhesions. If a whole range of preventive measures aimed at preventing adhesive disease can be in a timely manner, it is possible to avoid this severe pathology.
Forms
Depending on the etiology of the occurrence, adhesive disease can be:
- Congenital. Rare cases of such pathologies are usually represented by the sacrifices between the loop of the colon (Jackson membranes) or flat interchequctal battles (the so-called damasters of Lane).
- Acquired, developing as a result of surgical operations, inflammatory diseases of the perigesons (peritonitis, viscerite, periprocesses of internal organs) or its traumatic damage, accompanied by hemorrhages in the visceral leaf area.
Features of the clinical current make it possible to distinguish three main forms of adhesive disease:
- acute, accompanied by pronounced symptomatic intestinal obstruction;
- an intermittent, distinguished calm clinical flow;
- chronic, characterized by alternating periods of the complete absence of clinical manifestations and exacerbations of the ailment.
Code of the ICD-10
In the latest version of the international classification of diseases (ICD-10), the abdominal spikes are assigned to the XI class covering the diseases of the digestive system.
In the "Other defeat of the peritoneum" (under the code K66. 0) Spikes are combined:
According to this classification, adhesive disease is referred to immediately to two classes. The basis for the extraction of adhesive diseases of a small pelvis into a separate category is inflammatory lesions of female genital organs.
Causes of the disease
There is a huge number of reasons that can provoke the development of the adhesive process.
The only moment uniting all these reasons is the final result - damage to the tissues and organs of the abdominal cavity (the type of damage in this case does not have the value).
Damaging factors for convenience are made to divide into three groups.
Mechanical damage to the abdominal cavity accompanied by the emergence internal bleeding, the formation of a hematoma, metabolic disorders and outflow of lymph in structures of affected tissues, may occur as a result:
- surgical interventions;
- strong blows;
- all sorts of drops (on solid objects or from height);
- bullet wounds;
- koloto-cut wounds.
A group of inflammatory diseases capable of leading to the emergence of adhesive disease is presented:
- appendicitis (inflammation of the appendix);
- colitis (inflammation of the colon);
- enteritis (inflammation of the small intestine);
- ooforitis and salpingitis (ointment of uterine pipes and appendages);
- cholecystitis (inflammation of the gallbladder).
Chemical injuries of the abdominal organs can be obtained as a result:
- publishing the stomach - the most dangerous complication peptic diseaseending in the abdominal cavity of the contents of the stomach and concentrated gastric juice;
- severe pancreatitis, leading to spreading specific enzymes throughout the abdominal cavity;
- alkaline or acid burns obtained due to the intentional or random use of acids and alkalis;
- gap bubble with inevitable oral influence.
A fairly common cause of adhesion disease in the field of small pelvis and intestines and intestines is the presence of a chronic inflammatory process in genital female organs.
The cunning of this illness is that due to the gloveness of clinical manifestations, it may proceed for many years, leading to irreversible changes, the most difficult of which is infertility.
In rare cases, the adhesion process can be a consequence of intrauterine defects of development and congenital anomalies.
Symptoms of adhesive diseases of the abdominal cavity
Features of the clinical course of adhesive disease are directly related to the form of the pathological process.
As increasing the obstruction of the intestine of the patient suffers from:
- Constant thirst.
- Frequent seizures of vomiting (the composition of the vomit is first submitted by the contents of the small intestine, then the gastric juice and bile). Vomiting, not bringing relief, leaves a feeling of gravity in the stomach.
- Tachycardia.
- Discomfort caused by a bowl of the intestines.
- Arterial hypertension.
In addition to the above manifestations, it should be noted:
- skin sinusiness, tight lips, ears, fingers on hands and legs, nose tip;
- braking of conditional reflexes;
- a significant reduction in the volume of urine produced by the kidneys during the day (daily diurea).
When the belly palpation, the patient experiences acute pain, to establish the localization of which it is difficult.
The intermittent form of adhesive disease is characterized by the frequency of emerging pain. For this form of illness, a whole complex of dyspeptic disorders is characterized (the occurrence of heartburn, obscure acid, increased gas formation, sensations of the overflow of the stomach) and a significant change in intestinal peristaltics. In some patients, it, intensifying, leads to the emergence of diarrhea, the others weakens so much that it provokes the appearance of constipation.
For chronic shape of adhesive disease, the presence of weakly pronounced clinical manifestations is characterized: occasionally emerging other pains and rather minor intestinal disorders.
As a rule, such a form acquires a safe process that struck the female genitals. His main danger is a negative impact on the formation of the menstrual cycle and the ability to the birth of children.
Diagnostic methods
To suspect the existence of the adhesive process, an experienced surgeon may still at the initial examination of the patient.
The basis for suspicion may be:
- whole complex of characteristic complaints;
- previously transferred inflammatory diseases of the abdominal organs;
- implemented surgical interventions;
- infectious pathologies.
To form an accurate diagnosis, a number of instrumental research is needed:
- Ultrasound of the abdominal organs. The main value of this diagnostic procedure consists in the possibility of identifying the adhesive process on its preclinical stage, which greatly facilitates the treatment of ailment and improves its forecast. In the case of detection of the adhesive process at a later stage of its development, ultrasound allows to determine the exact localization of connective tissues and their prevalence.
- Laparoscopy - procedures for the diagnostic examination of the condition of the abdominal cavity using the optical system of the laparoscope - the device introduced into the patient's body through small punctures in the front wall of the abdomen. An endovide camera mounted in a laparoscope transmits an image to a special monitor equipped with a multiple increase function, so the execution of laparoscopy is carried out under the control of vision. The main advantage of this diagnostic procedure is its low traumaticity and the possibility of diagnosing without waste. If necessary, diagnostic laparoscopy can easily transform into a medical procedure: finding spikes, the surgeon can perform an operation to eliminate them.
- MSCT (multispiral computed tomography) of the abdominal organs allowing to obtain two- and three-dimensional images of internal organs with which you can identify any neoplasms.
- The overview radiography of the abdominal cavity is a diagnostic technique that is of great importance in the formulation of an accurate diagnosis in adhesive disease. X-ray pictures obtained during the procedure can identify the presence of increased gas formation in the intestines, its bloating, as well as the presence of inflammatory exudate in the abdominal cavity. To determine the degree of intestinal obstruction, radiography is often performed using an X-ray-contrast substance - barium sulfate suspension.
How to treat adhesive disease?
The treatment of adhesive disease can be:
- Conservative. The main goal conservative therapy It is preventing the emergence of adhesions and their complications, as well as the elimination of their clinical manifestations.
- Surgical. Indications for surgery are: urgent acute states, frequent exacerbations and regular recurrence of adhesive disease.
The first priority of the conservative treatment of the adhesive process is to relieve pain syndrome. If the pains are caused by the accumulation of gases in the intestine and the presence of constipation, to alleviate the patient's condition will help:
- cleansing enema;
- taking antispasmodics - drugs that contribute to the relaxation of smooth muscles;
- applying heat to the stomach.
To get rid of constipation, the patient is prescribed:
- A special diet consisting of products that contribute to the strengthening of intestinal peristaltics (there must be a large amount of plant fiber).
- Preparations that have a light laxative effect.
- A number of physiotherapy procedures. The ionophoresis (method of delivery of charged ions with electroplating currents of low voltage and low force), diathermy (heating the deep-resolidating organs and tissues, helps electric shock High frequency), mud and the cycle of paraffin applications.
- Full failure physical Loadscontributing to the spizming of smooth muscles and provoking the amplification of pain syndrome.
For termination of vomiting, antiemetic drugs prescribe patients, and intravenous introduction of special drugs helps to cope with the effects of dehydration.
Operation
Operational interventions related to the treatment of adhesive process require a mandatory and very serious preoperative preparation of the patient.
To eliminate the symptoms of dehydration and normalize the acid-base condition of the blood, the patient intravenously - in addition to the blood plasma - solutions are poured:
The choice of operational intervention methods in each specific case is carried out individually: during operation, detected spikes can be removed, divided or spread.
Dissection of adhesions can be carried out with:
- electron-like (this area of \u200b\u200bmedicine is called electrosurgery);
- laser (during laser and therapy operation);
- water (this type of operation is called aquadissection).
The excision of the old scars remaining on the skin from the previous operation is not produced, since it is fraught with the development of complications associated with a durable soldering of intestinal loops.
In the presence of heavy, essentially deforming the intestines, impose bypass intercircuit anastomosis. If the Conglomerate of intestinal loops was too tight, perform resection of the problem area.
To prevent recurrence of adhesive disease, during surgery:
- cuts are made wide;
- take measures to prevent the dryness of the peritoness leaves;
- prevent hitting foreign languages in an operating wound;
- bleeding timely and remove blood;
- dry antiseptic and antibiotic drugs for processing operating wounds;
- conduct conservative treatment by introducing barrier liquids - diplot, dextrana (with the same purpose, films are applied to the surface of the ovaries and uterine pipes);
- polymer suture is used.
During the postoperative period, proteolytic enzymes are introduced into the patient's abdominal cavity, intestinal peristaltics are stimulated, antihistamine and anti-inflammatory drugs are prescribed.
Diet
Patient food presumably suffering from adhesive disease must obey a number of rules:
- Acceptable food should be warm and rubbed, and the volume of portions - reduced to a minimum.
- It should be eaten at least five to six times a day.
- It is necessary to make a power schedule, which provides for the same clock of food intake: it will facilitate the body of the problem for its processing.
The main goal of such a diet is to prevent the intelligence sensations associated with the occurrence of constipation and driving the abdomen.
During the preoperative period, the patient must completely refuse to use:
- Products containing a large amount of coarse vegetable fibers, overloading the intestines and the cause of increased gas formation. This category includes: corn, legume crops, any kind of cabbage.
- Smoked, pickled, salted and fried dishes.
- Mushrooms who are poorly digested by the human body.
- Baking baking I. white breadprovoking the "swelling" of the abdomen.
- Mayonnaise, fat broths and sauces activating fermentation processes and capable of reinforcing pain syndrome.
- Any sharp seasonings (adjusts, peppers, mustard) capable of irritating the mucous membranes of the gastrointestinal tract organs.
- Carbonated drinks, tea, coffee and milk. The best drinks during diet are green tea and drinking water.
At the table of a patient suffering from adhesive disease, should be:
- Puree from boiled vegetables.
- Lean broths.
- Low-fat fish, chicken and rabbit meat (exclusively in boiled form).
- Dishes from cottage cheese and cheese.
- Non-fat yogurt and kefir.
- Strongly strained liquid cereals (oatmeal or buckwheat), prepared on water with the addition of a small piece of butter.
Postoperative nutrition
Compliance with the diet after the elimination of adhesions is necessary so that the mucous membranes of the operated organs can fully recover.
- For twenty-four hours after the operation, the patient must refrain from eating any food. It is possible to drink water, but in small quantities.
- After a day, the diet of the operated patient includes lean broths and liquid rubbing cripples.
- In the following days, vegetable soups, purees, juices and ragners are introduced into the menu medicinal herbalSugar not containing.
During this period, the operated patient is allowed to use:
- Scrambled eggs.
- Boiled chicken and fish.
- Puree soups cooked from carrots, beets and zucchini.
- Efficiency products (especially kefir), contributing to the rapid restoration of the body.
- Apples (rubbed or baked).
- Compats, kisins and fruits.
- Fruit juices, which should be exclusively fresh and half diluted with clean drinking water.
The selection of a postoperative diet is individually carried out by the attending physician. The harder and launched was a transferred ailment - the more strict is the appointed diet.
The patient must in every way avoid the use of products capable of provoking the occurrence of constipation, bloating and irritation of the mucous membranes of digestive organs.
Folk remedies
Folk medicine drugs for adhesive diseases can have an effective impact or as prophylaxis of relapse (during the rehabilitation period), or on the most early stages illness as an additional fundamental treatment.
- Most often applies the decoction of the Hypericum. Taking a dining spoon of dry raw materials, poured it with a glass of steep boiling water and boiled in a water bath for a quarter of an hour. After the filping, they drink 100 ml three times a day.
- A similar action has a decoction made from a tablespoon of plantain seeds and 400 ml of water (the cooking technology is the same as in the prescription described above). The duration of the course of treatment - under the condition of three-time reception on one tablespoon - is at least four weeks.
- No less demanded infusion made from a hipsnik berry (30 g), lingonberries (15 g) and nettle leaves (30 g). Bay of phytosyrin liter boiling water, insist in a thermos overnight. Take 100 ml: before bedtime and only on an empty stomach.
- Mixing the dry phytosyrier (the donon, mother-and-stepmother and the gold masculine, taken in equal shares), take a tablespoon of herbal collection and, falling asleep into a thermos, pour the glass of steep boiling water. After two-hour instead, the infusion is taken by 100 ml at least five times a day. The minimum course of treatment is four weeks.
Prevention and forecast
In the presence of single adhesions, the forecast is favorable, which cannot be said about the disease leading to the emergence of multiple lesions.
It is possible to prevent the development of adhesive disease by complying with a number of uncomplicated rules prescribing:
- compliance healthy image life;
- the need for rational and full nutrition;
- the obligation of optimal sports loads;
- invalidation of alternation of periods of long starvation with episodes of overeating;
- mandatory monitoring of the regularity of the chair;
- the need for measures aimed at ensuring full digestion;
- the obligation of regular inspections from the gastroenterologist.
To prevent the need for repeated surgical interventions, the specialists of the leading clinics resort to the method of preoperative identification of a constitutional hereditary predisposition to the formation of adhesions.
After performing the operation in the abdominal cavity of the patient, special antley preparations are introduced.
There is a suggestion that the economic benefit from the use of antisposhic drugs to the introduction of the method of preoperative detection of genetic predisposition to adopted diseases Russian Federation It may make more twenty million dollars only by reducing the cases of re-acute adhesive intestinal obstruction.
Bashes of the abdominal cavity: symptoms and treatment
Flash disease is a permanent companion of any surgical interventions in the abdominal cavity. The severity of symptoms depends on the severity and prevalence of the process. It may proceed as asymptomatic and bring significant discomfort to the patient. Some scientists believe that the abdominal surgery in 100% of cases is accompanied by the formation of adhesions, but in the future part of the adhesion is solved independently.
Occasionally there are symptoms of a congenital adhesive process, which is found in newborns, previously not exposed to surgical interventions.
Laparoscopy is considered a new factor that has frequent cases of adhesive disease.
Mechanism for the development of adhesive disease
The peritonese, covering organs of the abdominal cavity, has a property to accommodate damage zones. For example, it happens with an untreated appendicitis, the peritoneum sticks to the zone of inflammation and forms a limited cavity - appendicular infiltrate. Also occurs during operational interventions - the peritoneum sticks:
- to pieces of cut;
- to the operated organ;
- to the zone of inflammation.
In the resolution of common inflammatory processes or in chronic inflammation in the abdominal cavity, it is especially true of infectious diseases of the fallopian tubes and ovaries, the peritonean is affusually glued to all organs, violating their location and normal functioning. In the future, the formed spikes are compacted and shortened, even more shifting and pursuing the organs and tissues that have fallen into them. In this case, squeezing, feeding organs and tissues, vessels. Normal bloodstream is disturbed and oxygen starvation develops, which causes abdominal pain during adhesive disease. Also, as a result of the displacement and narrowing of the intestinal lumen, the movement of the roaming masses is disturbed, which, in turn, leads to permanent constipation. And in the extreme case, it can lead to the development of such a formidable state, as intestinal obstruction.
The international classifier of diseases of the ICD-10 allocates separate adhesive disease of the abdominal cavity and adhesive disease of the small pelvis. In essence, it is one disease, since the small pelvis is also part of the abdominal cavity. This disease is distinguished into a separate category, because the cause of adhesions, most often, are inflammatory diseases of the female genital organs.
The reasons
The reasons for the development of the adhesive process are many, but they are united by one - they all lead to damage to organs or tissues in the abdominal cavity, regardless of which kind of damage.
Let us dwell at the most frequent reasons for the adhesive process:
- Mechanical injuries of the abdominal cavity:
- strikes, drops from height, falling on a solid object;
- wounded wounds;
- bullet injuries;
- surgical operations;
- Chemical damage:
- burns with acids or alkalis when random or deliberately use;
- sprinkling the stomach with an exit to the abdominal cavity of acidic gastric content;
- severe pancreatitis with the vulnerament of pancreatic enzymes on the abdominal cavity;
- tarve the gallbladder with an influence of bile.
- Inflammatory diseases:
- appendix (appendicitis);
- gallbladder (cholecystitis);
- subtle intestine (enteritis);
- tolstoy intestine (colitis);
- pipes and appendages (salpinting, ooforite).
The resultant cause of the development of adhesive disease around the intestines and the small pelvis organs is a chronic inflammatory process in female genital organs. Since with low-level symptoms and, accordingly, long flow, it leads to a pronounced and often irreversible process up to infertility.
Related factors - a patient nutrition, diabetes, foreign materials in the wound.
Classification
According to the ICD-10, the spikes of the abdominal cavity are divided:
- Pervian spikes (K66.0), which include:
- abdominal (walls) spikes;
- spikes diaphragm;
- spikes intestines;
- pelvic spikes in men;
- spikes mesenter of thin and / or a large intestine
- spikes of the gland;
- spikes stomach.
- Peritoneal inflammatory spikes in women in small pelvis (N73.6).
- Postoperative spikes in a small pelvis (N99.4).
The whole picture of the disease can be described by triad complaints, which includes the following symptoms:
Of course, not everyone will feel like a person. Depending on the location of the pathological process, the age and duration of the adhesive disease, these symptoms may appear in various combinations. Symptoms are not always found and sometimes discovered only with some random studies, for example, in women in research on infertility.
Painful feelings in the stomach arise due to the fact that squeezing or explosion of the sector. The intestines peristals and struggles with a non-German. The pain is always long. After all, the spikes are formed gradually. When the spikes compress the intestine, then the intestinal obstruction begins. The pain is first deaf, distant, but then becomes an acute cutting belly. It can be localized in a certain area of \u200b\u200bthe abdomen either over the entire surface. If you do not seek medical attention in time, then the pathological process will be aggravated and the pain will become unbearable. The fear of death appears. Then everything subsides. This means that all nervous endings are destroyed, and irreversible processes began.
Since the intestine continues to work, and the promotion of internal content does not occur due to obstacles, it is manifested by vomiting, constipation and flatulence. If the adhesive disease affects the small intestine, then the first symptom together with the pain will be vomiting. When the pathological process is limited to the colon, it starts with constipation.
Vomiting may be abundant, multiple. The composition of the vomit first includes products eaten on the eve, then gastric and intestinal juices, bile. Vomiting does not bring relief. There is a feeling of gravity in the stomach. Nausea does not leave for a minute. The act of vomiting is painful, since antiperistal waves affect the areas of the non-working intestine, which hurts with greater intensity.
People face constipation in everyday life. Therefore, at the beginning, a person does not pay due attention. Everyone thinks that everything will pass. But constipation in adhesive disease, it's not just constipation! Spikes are increasingly binding the intestines like a web. It violates his work. The dietary masses are in the intestine immobilized and begin to wander. This leads to the formation of a large amount of gases, which can also not go out. There is a bowl of the intestines and the abdomen accordingly. The intestine is stretched, which also causes painful sensations. The patient is trying to go to the toilet as productively as possible, I use several approaches. But everything is in vain. Treatment with laxative and enema does not help either. On the contrary, may aggravate the situation.
Favoring disease can affect the small pelvis organs. In this case, the symptoms may be slightly modified. It is typical for women who have transferred operations in this area and often ill-suffering in inflammatory diseases of the genitals. In the small pelvis in women there is a uterus, a fallopian tube and ovaries. They can be involved in the process. After all, the spikes do not choose who to tighten into their pathological web. As a result, women begin problems with menstruation. They become painful, irregular, up to complete cessation. This is explained by the fact that the uterus is shifted, the pipes are beyond or squeezed, the ovaries twisted. All this requires an immediate appeal for medical care, as it leads to infertility in a launched form.
Surgeons resort to some special methods of preventive treatment during operation, which reduce the spread of the adhesive process around the intestine. These are special gels with enzymes, soluble membranes, special solutions, washing intestines. Also, the prevention of the development of adhesive disease around the intestines contributes: moistened gas with less pressure with laparoscopic manipulations, the use of special surgical gloves without powder, the use of wet tampons when working with intestines, shortening the time of surgical intervention, antibiotic treatment before and after surgery and other measures.
Preventive treatment of adhesive disease is preventive measures taken during surgery, such as:
- Use during surgical treatment of 4% of the ICodextrin polymer;
- Treatment with carboxymethylcellulose and polyethylene oxide, which create a jelly-like barrier around the intestines;
- Application for the treatment of barrier membranes with hyaluronic acid, cellulose and other materials.
The feature of the adhesive disease is also in the fact that it can develop in a fairly remote period after the operation. If despite all the preventive spike treatment methods formed, they cannot be cured at home. Folk remedies here are powerless. It is not worth going to the signals and psychics. Since you can lose precious time.
When the process began to spread to internal organs, intestines, in a small pelvis and appeared the above complaints to seek medical attention. In this case, there is only surgical methods for the treatment of adhesive disease. Tactics determines the attending physician.
After analyzing the causes of adhesive disease, it can be concluded that it is almost impossible to prevent this disease. Partly this statement is true. Nevertheless, some non-surgical causes of the development of adhesive disease can be prevented.
Compliance with a number of simple rules will significantly reduce the risk of the development of adhesive disease in a small pelvis:
- Diseases such as appendicitis, cholecystitis, acute pancreatitis, the peritonitis of the houses are not treated at home. And do not even try to google in search of the best herbal collection. These diseases are treated in the hospital surgeon.
- Chronic inflammatory diseases of the abdominal cavity should also be treated under the control of the doctor.
- Follow your sex health, and this:
- compliance with the rules of intimate hygiene;
- use of barrier methods of contraception;
- maintaining a morally right sex life with one sexual partner;
- regular medical inspection of small pelvis;
- examination on infections transmitted by the sexual way;
- timely treatment of inflammatory diseases of female genital organs.