Lymphadenitis. Submandibular lymphadenitis: causes, symptoms and treatment Inflammation of the lymph nodes mkb 10
In 2007, the World Health Organization carried out 10 revisions of the classification of diseases in order to subordinate them to the international coding of diagnoses, and as a result, 22 subsections were obtained. According to the generally accepted standard for ICD 10, the lymphadenitis code is L04, with the exception of some diseases, which we will consider below.
What is lymphadenitis
Lymphadenitis is a disease lymph nodes associated with their inflammation, reaching an infectious-purulent form. Pathology is not only unpleasant painful sensations, discomfort, as well as those that affect appearance... Most often, you can find inflammatory processes in the neck, jaw, armpits.
The trigger signal is the ingress of an infection or a pyogenic microorganism into the lymph node. They enter the system from blood or lymph fluid. The first symptoms are most often pain accompanied by weakness, malaise, elevated temperature, headache, enlargement of lymph nodes in size.
Views
There are several classifications of this disease, which are also reflected in ICD 10. Depending on the duration of the course, there is an acute and chronic form... Depending on the location, they are distinguished:
- submandibular lymphadenitis;
- pathology in the neck;
- inflammation of the nodes of the armpits;
- inguinal lymphadenitis.
Patients with similar diagnoses are hospitalized. The doctor prescribes drug treatment, physiotherapy procedures, rest.
By the nature of the infection, a purulent stage can be distinguished, accompanied by constant, throbbing pain, compaction, redness of the skin in the area of inflammation. This type can lead to serious complications, sepsis, as it quickly spreads to neighboring lymph nodes, penetrates into nearby tissues and cells. Purulent pathology requires mandatory surgical intervention, drainage. In the absence of pus, the disease is much easier, does not require surgical intervention, and does not change the condition of the skin.
Classification according to ICD10
Lymphadenitis in ICD 10 can be found in three sections:
- Diseases of the circulatory system include a chronic type of disease under number I1, nonspecific mesenteric in acute or chronic form - I88.0, nonspecific unspecified - I88.9, as well as other forms of nonspecific pathology - I88.8.
- Diseases of the skin and subcutaneous tissue L04 include an acute form of pathology, numbered according to the location: 0 - face, head and neck, 1 - trunk, 2 - upper limbs (including armpits, shoulder), 3 - lower limbs, pelvic area, 8 - other sites, 9 - unspecified.
- Lymph node enlargement can be attributed more to symptomatology than diagnosis, however, it also has a separate classification: R59.0 - well-defined localization, R59.1 - generalized enlargement, lymphadenopathy NOS (except for HIV, which is included in B23.1), R59.9 - unspecified form.
Based on the above classification, it is possible to clearly determine where this or that diagnosis belongs. For example, cervical lymphadenitis in ICD 10 refers to L04.0. This approach allows you to standardize medical documents around the world.
In Russia, the International Classification of Diseases of the 10th revision (ICD-10) has been adopted as a single normative document to take into account the incidence, reasons for medical institutions all departments, causes of death.
ICD-10 was introduced into health care practice throughout the Russian Federation in 1999 by order of the Ministry of Health of Russia dated 05/27/97. No. 170
A new revision (ICD-11) is planned by WHO in 2017 2018.
As amended and supplemented by WHO
Processing and translation of changes © mkb-10.com
Inguinal lymphadenitis
Inguinal lymphadenitis is a type of inflammation of the lymph nodes. The main function of the lymphatic system is to protect the body from various kinds of external influences. This is done by the formation of special immune cells in it, which protect the body from all kinds of infections. Thus, human health directly depends on the state of the lymphatic system. If a person has inflammation of the lymph nodes, this indicates the presence in the body of an infection that is dangerous to health.
Inguinal lymphadenitis in men and women is a secondary disease that occurs due to the presence of inflammation in any part of the body. The most common cause of inguinal lymphadenitis is a sexually transmitted disease. Primary inflammation of the lymph nodes is very rare, and its pathogens are pathogenic microflora.
Inguinal lymphadenitis symptoms
The main symptoms of inguinal lymphadenitis in women and men are:
- induration and enlargement of the lymph nodes in the groin;
- increased body temperature;
- a state of general malaise, weakness;
- the appearance of painful sensations in the groin and lower abdomen with physical activity and walking;
- redness of the skin around the lymph nodes.
It happens that inguinal lymphadenitis spreads to all lymph nodes. If lymphadenitis is purulent, then its result may be an abscess, in which the walls decompose blood vessels accompanied by constant bleeding. In this case, immediate treatment of inguinal lymphadenitis is necessary.
Causes of inguinal lymphadenitis
If you suspect lymphadenitis, you should immediately contact a therapist, who, in turn, can refer the patient for consultation to other specialists and for an examination.
Sometimes the cause of inguinal lymphadenitis can be a serious illness such as syphilis. Inguinal lymphadenitis in men may result from metastases malignant formation testicles or penis. In women, inguinal lymphadenitis often occurs as a result of ovarian cysts and various fungal diseases.
In children, inflammation of the inguinal lymph nodes is extremely rare. If it occurs, then this indicates the presence of damage to the skin surfaces of the lower extremities as a result of abrasions, cuts and injuries. If, after the healing of all wounds, the lymph nodes continue to become inflamed, it is urgent to show the child to a specialist.
Inguinal lymphadenitis treatment
The exact diagnosis and the main cause of inguinal lymphadenitis can only be determined by a doctor. Therefore, the patient should not self-medicate, but seek the advice of a specialist.
Inguinal lymphadenitis treatment can be conservative or operative. Conservative treatment used at an early stage of the disease. The patient is prescribed adequate antibiotic therapy. During treatment, the patient is shown complete rest and warmth, but it is strictly forbidden to warm up the inflamed lymph node itself. Heat provokes the further course of the inflammatory process. It should also be borne in mind that lymphadenitis may be the result of a malignant tumor, and in this case, heating is strictly prohibited, since it promotes the spread of cancer cells. For the treatment of the disease, special aseptic dressings of local action are widely used.
If the inguinal lymphadenitis has developed into a purulent form, then it can cause necrosis of the surrounding tissues. In this case, the treatment of inguinal lymphadenitis is only surgical. The surgeon makes an incision inflamed lymph node, extracts pus from there and removes nearby dead tissue. With the help of antimicrobial and antiseptic drugs, the doctor drains the opened cavity.
For the treatment of the chronic form of inguinal lymphadenitis, it is first of all necessary to determine the cause of the disease. If the cause is any sexually transmitted disease, then the main treatment should be aimed at eliminating it. As a rule, after eliminating the cause, the inflammation of the lymph nodes goes away on its own. If the inflammation does not disappear, the doctor prescribes an additional X-ray examination and prescribes treatment aimed at strengthening the patient's immunity.
Today, doctors are trying to resort to surgical intervention only in extreme cases, since it has been proven that it can lead to an incorrect outflow of lymph, which, in turn, leads to lymphostasis or elephantiasis.
© g. ICD 10 - International classification of diseases 10th revision
Lymphadenitis encoding according to ICD
In 2007, the World Health Organization carried out 10 revisions of the classification of diseases in order to subordinate them to the international coding of diagnoses, and as a result, 22 subsections were obtained. According to the generally accepted standard for ICD 10, the lymphadenitis code is L04, with the exception of some diseases, which we will consider below.
What is lymphadenitis
Lymphadenitis is a disease of the lymph nodes associated with their inflammation, reaching an infectious-purulent form. Pathology is unpleasant not only with painful sensations, discomfort, but also with the fact that it affects the appearance. Most often, you can find inflammatory processes in the neck, jaw, armpits.
The trigger signal is the ingress of an infection or a pyogenic microorganism into the lymph node. They enter the system from blood or lymph fluid. The first symptoms are most often painful sensations, accompanied by weakness, malaise, fever, headache, enlargement of the lymph nodes in size.
There are several classifications of this disease, which are also reflected in the ICD 10. Depending on the duration of the course, there is an acute and chronic form. Depending on the location, they are distinguished:
- submandibular lymphadenitis;
- pathology in the neck;
- inflammation of the nodes of the armpits;
- inguinal lymphadenitis.
Patients with similar diagnoses are hospitalized. The doctor prescribes medication, physiotherapy, and rest.
By the nature of the infection, a purulent stage can be distinguished, accompanied by constant, throbbing pain, compaction, redness of the skin in the area of inflammation. This type can lead to serious complications, sepsis, as it quickly spreads to neighboring lymph nodes, penetrates into nearby tissues and cells. Purulent pathology requires mandatory surgical intervention, drainage. In the absence of pus, the disease is much easier, does not require surgical intervention, and does not change the condition of the skin.
Classification according to ICD10
Lymphadenitis in ICD 10 can be found in three sections:
- Diseases of the circulatory system include a chronic type of disease under number I1, nonspecific mesenteric in acute or chronic form - I88.0, nonspecific unspecified - I88.9, as well as other forms of nonspecific pathology - I88.8.
- Diseases of the skin and subcutaneous tissue L04 include an acute form of pathology, numbered according to the location: 0 - face, head and neck, 1 - trunk, 2 - upper limbs (including armpits, shoulder), 3 - lower limbs, pelvic area, 8 - other sites, 9 - unspecified.
- Lymph node enlargement can be attributed more to symptomatology than diagnosis, however, it also has a separate classification: R59.0 - well-defined localization, R59.1 - generalized enlargement, lymphadenopathy NOS (except for HIV, which is included in B23.1), R59.9 - unspecified form.
Based on the above classification, it is possible to clearly determine where this or that diagnosis belongs. For example, cervical lymphadenitis in ICD 10 refers to L04.0. This approach makes it possible to standardize medical records around the world.
Add a comment Cancel reply
- Scottped on Acute gastroenteritis
Self-medication can be hazardous to your health. At the first sign of disease, consult a doctor.
ICD 10. Class XII (L00-L99)
ICD 10. CLASS XII. DISEASES OF THE SKIN AND SUBCUTANEOUS CELLS (L00-L99)
Excludes: certain conditions originating in the perinatal period (P00-P96)
complications of pregnancy, childbirth and postpartum period(O00-O99)
congenital malformations, deformities and chromosomal abnormalities (Q00-Q99)
illness endocrine system, eating disorders and metabolic disorders (E00-E90)
injury, poisoning and some other consequences of exposure external causes(S00-T98)
lipomelanotic reticulosis (I89.8)
symptoms, signs and abnormalities identified
in clinical and laboratory research,
not elsewhere classified (R00-R99)
systemic violations connective tissue(M30-M36)
This class contains the following blocks:
L00-L04 Infections of the skin and subcutaneous tissue
L55-L59 Diseases of the skin and subcutaneous tissue associated with radiation
L80-L99 Other diseases of the skin and subcutaneous tissue
The following categories are marked with an asterisk:
L99 * Other disorders of skin and subcutaneous tissue in diseases classified elsewhere
Infections of the skin and subcutaneous tissue (L00-L08)
If necessary, identify infectious agent use the additional code (B95-B97).
local skin infections classified in class I,
Herpetic viral infection (B00 .-)
lip adhesion crack [jam] (due to):
L00 Staphylococcal scalded blister syndrome
Excludes1: toxic epidermal necrolysis [Lyell's] (L51.2)
L01 Impetigo
Excludes: impetigo herpetiformis (L40.1)
pemphigus of newborn (L00)
L01.0 Impetigo [caused by any organism] [any site]. Impetigo Bockhart
L01.1 Impetiginization of other dermatoses
L02 Skin abscess, boil and carbuncle
Excluded: areas anus and rectum (K61 .-)
genitals (external):
L02.0 Skin abscess, furuncle and facial carbuncle
Excludes: ear external (H60.0)
head [any part other than face] (L02.8)
L02.1 Skin abscess, boil and carbuncle of neck
L02.2 Abscess of skin, boil and carbuncle of trunk. Abdominal wall. Back [any part other than gluteal]. Chest wall. Groin area. Perineum. Navel
Excludes: breast (N61)
omphalitis of newborn (P38)
L02.3 Abscess of skin, boil and carbuncle of buttock. Gluteal region
Excludes1: pilonidal cyst with abscess (L05.0)
L02.4 Abscess of skin, furuncle and carbuncle of limb
L02.8 Abscess of skin, furuncle and carbuncle of other sites
L02.9 Skin abscess, boil and carbuncle, unspecified. Furunculosis NOS
L03 Phlegmon
Includes: acute lymphangitis
eosinophilic cellulitis [Welsa] (L98.3)
febrile (acute) neutrophilic dermatosis [Sweet] (L98.2)
lymphangitis (chronic) (subacute) (I89.1)
L03.0 Phlegmon of fingers and toes
Nail infection. Onychia. Paronychia. Perionychia
L03.1 Phlegmon of other extremities
Armpit. Pelvic girdle. Shoulder
L03.3 Phlegmon of the trunk. The walls of the abdomen. Backs [any part]. Chest wall. Groin. Perineum. Navel
Excludes1: omphalitis of newborn (P38)
L03.8 Cellulitis of other sites
Heads [any part other than the face]. Scalp
L03.9 Phlegmon, unspecified
L04 Acute lymphadenitis
Included: abscess (acute)> any lymph node,
acute lymphadenitis> except mesenteric
Excludes: enlarged lymph nodes (R59.-)
human immunodeficiency virus disease
[HIV], manifested as a generalized
Chronic or subacute, other than mesenteric (I88.1)
L04.0 Acute lymphadenitis of face, head and neck
L04.1 Acute lymphadenitis of trunk
L04.2 Acute lymphadenitis of the upper limb. Armpit. Shoulder
L04.3 Acute lymphadenitis lower limbs... Pelvic girdle
L04.8 Acute lymphadenitis of other sites
L04.9 Acute lymphadenitis, unspecified
L05 Pilonidal cyst
Includes: fistula> coccygeal or
L05.0 Pilonidal cyst with abscess
L05.9 Pilonidal cyst without abscesses. Pilonidal cyst NOS
L08 Other local infections of the skin and subcutaneous tissue
Excludes1: pyoderma gangrenous (L88)
L08.8 Other specified local infections of skin and subcutaneous tissue
L08.9 Local infection of skin and subcutaneous tissue, unspecified
Bullous Disorders (L10-L14)
Excludes: benign (chronic) familial pemphigus
staphylococcal scalded blister syndrome (L00)
toxic epidermal necrolysis [Lyell's syndrome] (L51.2)
L10 Pemphigus [pemphigus]
Excludes: pemphigus of newborn (L00)
L10.0 Pemphigus vulgaris
L10.1 Pemphigus vegetative
L10.2 Pemphigus foliaceus
L10.3 Pemphigus brazilian
L10.4 Pemphigus erythematous Senir-Asher syndrome
L10.5 Pemphigus due to drugs
L10.8 Other pemphigus
L10.9 Pemphigus, unspecified
L11 Other acantholytic disorders
L11.0 Acquired follicular keratosis
Excludes1: follicular keratosis (congenital) [Darrieus-White] (Q82.8)
L11.1 Transient acantholytic dermatosis [Grover]
L11.8 Other specified acantholytic changes
L11.9 Acantolytic changes, unspecified
L12 Pemphigoid
Excludes: herpes of pregnancy (O26.4)
herpetiform impetigo (L40.1)
L12.1 Cicatricial pemphigoid Benign Mucosal Pemphigoid [Levera]
L12.2 Chronic bullous disease in children Juvenile dermatitis herpetiformis
L12.3 Acquired epidermolysis bullosa
Excludes1: epidermolysis bullosa (congenital) (Q81.-)
L12.9 Pemphigoid, unspecified
L13 Other bullous changes
L13.0 Dermatitis herpetiformis Dühring's disease
L13.1 Subcorneal pustular dermatitis Sneddon-Wilkinson disease
L13.8 Other specified bullous changes
L13.9 Bullous changes, unspecified
L14 * Bullous skin disorders in diseases classified elsewhere
DERMATITIS AND ECZEMA (L20-L30)
Note In this block, the terms "dermatitis" and "eczema" are used interchangeably.
Excludes: chronic (childhood) granulomatous disease (D71)
diseases of the skin and subcutaneous tissue associated with exposure to radiation (L55-L59)
L20 Atopic dermatitis
Excludes1: limited neurodermatitis (L28.0)
L20.8 Other atopic dermatitis
L20.9 Atopic dermatitis unspecified
L21 Seborrheic dermatitis
Excludes1: infectious dermatitis (L30.3)
L21.1 Seborrheic dermatitis infantile
L21.8 Other seborrheic dermatitis
L21.9 Seborrheic dermatitis, unspecified
L22 Diaper dermatitis
Psoriasis-like rash caused by diapers
L23 Allergic contact dermatitis
Includes: allergic contact eczema
diseases of the skin and subcutaneous tissue associated with exposure to radiation (L55-L59)
L23.0 Allergic contact dermatitis due to metals. Chrome. Nickel
L23.1 Allergic contact dermatitis due to adhesives
L23.2 Allergic contact dermatitis due to cosmetics
L23.3 Allergic contact dermatitis due to drugs in contact with skin
If necessary, identify medicine use an additional external reason code (class XX).
L23.4 Allergic contact dermatitis due to dyes
L23.5 Allergic contact dermatitis due to other chemicals
Cement. Insecticides. Plastic. Rubber
L23.6 Allergic contact dermatitis due to food in contact with skin
L23.7 Allergic contact dermatitis due to plants, other than food
L23.8 Allergic contact dermatitis due to other substances
L23.9 Allergic contact dermatitis, cause unspecified Allergic contact eczema NOS
L24 Irritable contact dermatitis simple
Includes: simple irritant contact eczema
diseases of the skin and subcutaneous tissue associated
L24.0 Simple irritant contact dermatitis due to detergents
L24.1 Simple irritant contact dermatitis due to oils and lubricants
L24.2 Simple irritant contact dermatitis due to solvents
L24.3 Simple irritant contact dermatitis due to cosmetics
L24.4 Irritant contact dermatitis due to drugs in contact with skin
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
Excludes: allergy NOS due to drugs (T88.7)
drug-induced dermatitis (L27.0-L27.1)
L24.5 Simple irritant contact dermatitis due to other chemicals
L24.6 Simple irritant contact dermatitis due to food in contact with skin
Excludes1: dermatitis due to food eaten (L27.2)
L24.7 Simple irritant contact dermatitis due to plants, other than food
L24.8 Simple irritant contact dermatitis due to other substances Dyes
L24.9 Simple irritant contact dermatitis, cause unspecified Irritant contact eczema NOS
L25 Contact dermatitis, unspecified
Includes: contact eczema, unspecified
lesions of the skin and subcutaneous tissue associated
L25.0 Unspecified contact dermatitis due to cosmetics
L25.1 Unspecified contact dermatitis due to drugs in contact with skin
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
Excludes: allergy NOS due to drugs (T88.7)
drug-induced dermatitis (L27.0-L27.1)
L25.2 Unspecified contact dermatitis due to dyes
L25.3 Unspecified contact dermatitis due to other chemicals. Cement. Insecticides
L25.4 Unspecified contact dermatitis due to food in contact with skin
Excludes1: contact dermatitis due to ingested food (L27.2)
L25.5 Unspecified contact dermatitis due to plants, other than food
L25.8 Unspecified contact dermatitis due to other substances
L25.9 Unspecified contact dermatitis, cause unspecified
Dermatitis (professional) NOS
L26 Exfoliative dermatitis
Excludes: Ritter's disease (L00)
L27 Dermatitis due to ingested substances
allergic reaction NOS (T78.4)
L27.0 Generalized skin rash due to drugs and medication
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L27.1 Localized skin eruption due to drugs and medication
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L27.2 Dermatitis due to food eaten
Excludes1: dermatitis due to food in contact with skin (L23.6, L24.6, L25.4)
L27.8 Dermatitis due to other substances taken internally
L27.9 Dermatitis due to unspecified substances, taken by mouth
L28 Lichen simplex chronicus and pruritus
L28.0 Lichen simplex chronicus Limited neurodermatitis. Deprive NOS
L29 Pruritus
Excludes: neurotic skin scratching (L98.1)
L29.3 Anogenital pruritus, unspecified
L29.9 Pruritus, unspecified Itching NOS
L30 Other dermatitis
small plaque parapsoriasis (L41.3)
L30.2 Cutaneous autosensitization Candidal. Dermatophytosis. Eczematous
L30.3 Infectious dermatitis
L30.4 Erythematous intertrigo
L30.8 Other specified dermatitis
L30.9 Dermatitis, unspecified
PAPULOSQUAMOUS DISORDERS (L40-L45)
L40 Psoriasis
L40.0 Psoriasis vulgaris Coin psoriasis. Plaque
L40.1 Generalized pustular psoriasis Impetigo herpetiformis. Tsumbush's disease
L40.2 Acrodermatitis persistent [Allopo]
L40.3 Palmar and plantar pustulosis
L40.8 Other psoriasis Flexion inverse psoriasis
L40.9 Psoriasis, unspecified
L41 Parapsoriasis
Excludes1: atrophic vascular poikiloderma (L94.5)
L41.0 Pityriasis lichenoid and acute smallpox. Fly-Habermann disease
L41.1 Pityriasis lichenoid chronic
L41.2 Lympomatoid papulosis
L41.3 Small plaque parapsoriasis
L41.4 Large plaque parapsoriasis
L41.5 Network parapsoriasis
L41.9 Parapsoriasis, unspecified
L42 Pitiriasis pink [Gibert]
L43 Deprive red flat
Excludes1: versicolor flat hair (L66.1)
L43.0 Lichen hypertrophic red flat
L43.1 Lichen red flat bullous
L43.2 Lichen reaction to drug
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L43.3 Lichen red flat subacute (active). Deprive red flat tropical
L43.8 Other lichen planus
L43.9 Lichen red flat, unspecified
L44 Other papulosquamous changes
L44.0 Pityriasis red hair pityriasis
L44.3 Lichen red moniliform
L44.4 Childhood papular acrodermatitis [Gianotti-Crosty syndrome]
L44.8 Other specified papulosquamous changes
L44.9 Papulosquamous changes, unspecified
L45 * Papulosquamous disorders in diseases classified elsewhere
NETTLE AND ERYTHEMA (L50-L54)
Excludes: Lyme disease (A69.2)
L50 Urticaria
Excludes: allergic contact dermatitis (L23.-)
angioedema (T78.3)
hereditary vascular edema (E88.0)
L50.0 Allergic urticaria
L50.1 Idiopathic urticaria
L50.2 Urticaria due to exposure to low or high temperature
L50.3 Dermatographic urticaria
L50.4 Vibratory urticaria
L50.5 Cholinergic urticaria
L50.6 Contact urticaria
L50.9 Urticaria, unspecified
L51 Erythema multiforme
L51.0 Non-bullous erythema multiforme
L51.1 Bullous erythema multiforme Stevens Johnson Syndrome
L51.2 Toxic epidermal necrolysis [Lyell's]
L51.8 Other erythema multiforme
L51.9 Erythema multiforme, unspecified
L52 Erythema nodosum
L53 Other erythematous conditions
If it is necessary to identify a toxic substance, an additional external cause code (class XX) is used.
Excludes: neonatal toxic erythema (P83.1)
L53.1 Erythema annular centrifugal
L53.2 Erythema marginal
L53.3 Other chronic patterned erythema
L53.8 Other specified erythematous conditions
L53.9 Erythematous condition, unspecified Erythema NOS. Erythroderma
L54 * Erythema in diseases classified elsewhere
L54.0 * Marginal erythema in acute articular rheumatism (I00 +)
L54.8 * Erythema in other diseases classified elsewhere
DISEASES OF THE SKIN AND SUBCUTANEOUS CELLULARS,
RADIATION-RELATED (L55-L59)
L55 Sunburn
L55.0 First degree sunburn
L55.1 Second degree sunburn
L55.2 Third degree sunburn
L55.8 Other sunburn
L55.9 Sunburn, unspecified
L56 Other acute skin changes caused by ultraviolet radiation
L56.0 Drug phototoxic reaction
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L56.1 Photoallergic drug reaction
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L56.2 Photocontact dermatitis
L56.3 Solar urticaria
L56.4 Polymorphic light rash
L56.8 Other specified acute skin changes due to ultraviolet radiation
L56.9 Acute change skin caused by ultraviolet radiation, unspecified
L57 Skin changes due to chronic exposure to non-ionizing radiation
L57.0 Actinic (photochemical) keratosis
L57.1 Actinic reticuloid
L57.2 Skin rhombic on occiput (neck)
L57.3 Poikiloderma Sivatta
L57.4 Senile atrophy (lethargy) of the skin Senile elastosis
L57.5 Actinic [photochemical] granuloma
L57.8 Other skin changes due to chronic exposure to non-ionizing radiation
Farmer's skin. Seaman's leather. Solar dermatitis
L57.9 Skin change due to chronic exposure to non-ionizing radiation, unspecified
L58 Radiation dermatitis
L58.0 Acute radiation dermatitis
L58.1 Chronic radiation dermatitis
L58.9 Radiation dermatitis, unspecified
L59 Other diseases of skin and subcutaneous tissue associated with radiation
L59.0 Burn erythema [ab igne dermatitis]
L59.8 Other specified diseases of skin and subcutaneous tissue associated with radiation
L59.9Disease of skin and subcutaneous tissue associated with radiation, unspecified
DISEASES OF SKIN SEEDS (L60-L75)
Excludes: congenital malformations of the outer integument (Q84.-)
L60 Diseases of nails
Excludes: clavate nails (R68.3)
L60.5 Yellow nail syndrome
L60.8 Other diseases of nails
L60.9 Disorder of nail, unspecified
L62 * Changes of nails in diseases classified elsewhere
L62.0 * Clavate nail in pachydermoperiostosis (M89.4 +)
L62.8 * Changes of nails in other diseases classified elsewhere
L63 Alopecia areata
L63.1 Alopecia areata universal
L63.2 Acute baldness (ribbon-like)
L63.8 Other alopecia areata
L63.9 Alopecia areata, unspecified
L64 Androgenic alopecia
Included: male pattern baldness
L64.0 Drug-induced androgenetic alopecia
If it is necessary to identify a medicinal product, an additional code of external causes (class XX) is used.
L64.8 Other androgenic alopecia
L64.9 Androgenic alopecia, unspecified
L65 Other non-scarring hair loss
Excludes1: trichotillomania (F63.3)
L65.0 Telogenic hair loss
L65.1 Anagenic hair loss Regenerating Miasms
L65.8 Other specified non-scarring hair loss
L65.9 Non-scarring hair loss, unspecified
L66 Cicatricial alopecia
L66.0 Alopecia macula scarring
L66.1 Deprivation of flat hair. Follicular lichen planus
L66.2 Folliculitis resulting in alopecia
L66.3 Perifolliculitis of the head, abscessing
L66.4 Folliculitis reticularis cicatricial erythematous
L66.8 Other cicatricial alopecia
L66.9 Cicatricial alopecia, unspecified
L67 Hair color and hair shaft abnormalities
Excludes: knotted hair (Q84.1)
telogenic hair loss (L65.0)
L67.0 Trichorexis nodular
L67.1 Changes in hair color. Gray hair. Graying (premature). Hair heterochromia
L67.8 Other anomalies of hair and hair shaft color Breakage of hair
L67.9 Anomaly of hair and hair shaft color, unspecified
L68 Hypertrichosis
Includes: excessive hairiness
Excludes: congenital hypertrichosis (Q84.2)
resistant vellus hair (Q84.2)
L68.1 Hypertrichosis by vellus hair, acquired
If it is necessary to identify the drug that caused the violation, use an additional code of external causes (class XX).
L68.2 Localized hypertrichosis
L68.9 Hypertrichosis, unspecified
L70 Acne
Excludes: keloid acne (L73.0)
L70.0 Common acne [acne vulgaris]
L70.2 Smallpox acne Acne necrotizing miliary
L71 Rosacea
L71.0 Perioral dermatitis
If necessary, identify medicinal product causing the defeat, use the additional external cause code (class XX).
L71.9 Rosacea, unspecified
L72 Follicular cysts of skin and subcutaneous tissue
L72.1 Trichodermal cyst Hair cyst. Sebaceous cyst
L72.2 Stiatocystoma, multiple
L72.8 Other follicular cysts of skin and subcutaneous tissue
L72.9 Follicular cyst skin and subcutaneous tissue, unspecified
L73 Other disorders of hair follicles
L73.1 Beard hair pseudofolliculitis
L73.8 Other specified diseases of follicles Beard sycosis
L73.9 Illness hair follicles unspecified
L74 Diseases of the merocrine [eccrine] sweat glands
L74.1 Crystalline prickly heat
L74.2 Miliaria deep. Tropical anhidrosis
L74.3 Miliaria, unspecified
L74.8 Other diseases of merocrine sweat glands
L74.9 Disorder of merocrine sweating, unspecified Sweat gland affection NOS
L75 Diseases of apocrine sweat glands
Excludes: dyshidrosis [pompholyx] (L30.1)
L75.2 Apocrine prickly heat Fox-Fordyce disease
L75.8 Other diseases of apocrine sweat glands
L75.9 Disorder of apocrine sweat glands, unspecified
OTHER DISEASES OF THE SKIN AND SUBCUTANEOUS CELLS (L80-L99)
L80 Vitiligo
L81 Other pigmentation disorders
Excludes: birthmark NOS (Q82.5)
Peutz-Gigers syndrome (Touraine) (Q85.8)
L81.0 Post-inflammatory hyperpigmentation
L81.4 Other melanin hyperpigmentation Lentigo
L81.5 Leucoderma, not elsewhere classified
L81.6 Other disorders associated with decreased melanin production
L81.7 Pigmented red dermatosis Creeping angioma
L81.8 Other specified pigmentation disorders Iron pigmentation. Tattoo pigmentation
L81.9 Disorder of pigmentation, unspecified
L82 Seborrheic keratosis
Dermatosis papular black
L83 Acanthosis nigricans
Confluent and reticular papillomatosis
L84 Calluses and calluses
Wedge-shaped callus (clavus)
L85 Other epidermal thickenings
Excludes: hypertrophic skin conditions (L91.-)
L85.0 Acquired ichthyosis
Excludes1: congenital ichthyosis (Q80.-)
L85.1 Acquired keratosis [keratoderma] palmar-plantar
Excludes1: hereditary palmar-plantar keratosis (Q82.8)
L85.2 Keratosis punctate (palmar-plantar)
L85.3 Skin conjunctiva Dermatitis of dry skin
L85.8 Other specified epidermal thickenings Cutaneous horn
L85.9 Epidermal thickening, unspecified
L86 * Keratoderma in diseases classified elsewhere
Follicular keratosis> due to insufficiency
L87 Transepidermal perforation changes
Excludes: annular granuloma (perforated) (L92.0)
L87.0 Follicular and parafollicular keratosis invading the skin [Kirle's disease]
Follicular penetrating hyperkeratosis
L87.1 Reactive perforating collagenosis
L87.2 Creeping perforating elastosis
L87.8 Other transepidermal perforation disorders
L87.9 Transepidermal perforation disorder, unspecified
L88 Pyoderma gangrenous
L89 Decubital ulcer
Plaster cast ulcer
Compression ulcer
Excludes1: decubital (trophic) ulcer of the cervix (N86)
L90 Atrophic skin lesions
L90.0 Lichen sclerotic and atrophic
L90.1 Schwenninger-Buzzi anetoderma
L90.2 Jadasson-Pellisari anetoderma
L90.3 Pasini-Pierini atrophoderma
L90.4 Chronic atrophic acrodermatitis
L90.5 Cicatricial conditions and fibrosis of the skin Welded scar (skin). Scar. Disfigurement caused by scarring. Scar NOS
Excludes: hypertrophic scar (L91.0)
L90.6 Atrophic striae (striae)
L90.8 Other atrophic skin changes
L90.9 Atrophic skin change, unspecified
L91 Hypertrophic skin changes
L91.0 Keloid scar... Hypertrophic scar. Keloid
Excludes: keloid acne (L73.0)
L91.8 Other hypertrophic skin changes
L91.9 Hypertrophic skin change, unspecified
L92 Granulomatous changes of skin and subcutaneous tissue
Excludes1: actinic [photochemical] granuloma (L57.5)
L92.0 Granuloma annular. Perforated granuloma annular
L92.1 Lipoid necrobiosis, not elsewhere classified
Excluded: associated with diabetes mellitus(E10-E14)
L92.2 Facial granuloma [eosinophilic granuloma of the skin]
L92.3 Foreign body granuloma of skin and subcutaneous tissue
L92.8 Other granulomatous changes of skin and subcutaneous tissue
L92.9 Granulomatous changes of skin and subcutaneous tissue, unspecified
L93 Lupus erythematosus
systemic lupus erythematosus (M32 .-)
If it is necessary to identify the drug that caused the lesion, an additional external cause code (class XX) is used.
L93.0 Discoid lupus erythematosus Lupus erythematosus NOS
L93.1 Subacute cutaneous lupus erythematosus
L93.2 Other localized lupus erythematosus Lupus erythematosus deep. Lupus panniculitis
L94 Other localized connective tissue changes
Excludes: systemic connective tissue diseases (M30-M36)
L94.0 Localized scleroderma Limited scleroderma
L94.1 Linear scleroderma
L94.5 Poikiloderma vascular atrophic
L94.6 Anyum [spontaneous dactylolysis]
L94.8 Other specified localized connective tissue changes
L94.9 Localized connective tissue change, unspecified
L95 Vasculitis limited to skin, not elsewhere classified
Excludes: creeping angioma (L81.7)
hypersensitivity angiitis (M31.0)
L95.0 Marble skin vasculitis. White atrophy (plaque)
L95.1 Erythema sublime, persistent
L95.8 Other vasculitis limited to skin
L95.9 Vasculitis limited to skin, unspecified
L97 Ulcer of lower limb, not elsewhere classified
L98 Other diseases of the skin and subcutaneous tissue, not elsewhere classified
L98.1 Artificial [artifical] dermatitis. Neurotic skin scratching
L98.2 Sweet's febrile neutrophilic dermatosis
L98.3 Wells eosinophilic cellulitis
L98.4 Chronic skin ulcer, not elsewhere classified Chronic skin ulcer NOS
Tropical ulcer NOS. Skin ulcer NOS
Excludes: decubital ulcer (L89)
specific infections classified in A00-B99
lower limb ulcer NEC (L97)
L98.5 Mucinosis of the skin Focal mucinosis. Lychen myxedema
Excludes: focal oral mucinosis (K13.7)
L98.6Other infiltrative diseases of skin and subcutaneous tissue
Excludes1: hyalinosis of skin and mucous membranes (E78.8)
L98.8 Other specified disorders of skin and subcutaneous tissue
L98.9 Disorder of skin and subcutaneous tissue, unspecified
L99 * Other disorders of skin and subcutaneous tissue in diseases classified elsewhere
Nodular amyloidosis. Spotted amyloidosis
L99.8 * Other specified changes in skin and subcutaneous tissue in diseases classified elsewhere
Share the article!
Search
The last notes
E-mail subscription
Enter your email address to receive the latest news on medicine, as well as the etiology and pathogenesis of diseases, their treatment.
Categories
Tags
Site " Medical practice»Is dedicated to medical practice, which tells about modern methods diagnostics, the etiology and pathogenesis of diseases, their treatment are described
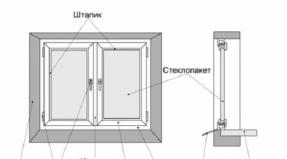
Submandibular lymphadenitis- This is swelling of the lymph nodes located in the lower jaw. These nodes are located between the submandibular glands, which are located under the tongue and the lower jawbone. This disease is not independent, but most often a symptom of any disease. In the world, this symptom affects one in ten for one reason or another.
Lymphadenitis has its own ICD code (International Classification of Diseases). This classification is used in many countries of the world and allows you to find out the description of the disease and the basis of its treatment. According to ICD-10, submandibular lymphadenitis is code L04. This code allows the doctor to correctly diagnose and prescribe the correct treatment.
The mechanism and causes of submandibular lymphadenitis
Lymphatic system - part immune system which helps the body fight disease and other harmful agents. The lymph nodes act as points of filtration and cell multiplication in this system. They cleanse the lymph fluid of unwanted bacteria and serve as an early warning of an infection in the body.
Submandibular nodes are small, usually about 1 cm in adults healthy people... You can feel them yourself. If the submandibular lymph nodes are enlarged, then, most often, this indicates the presence of a bacterial or viral infection.
Among the most common causes of the disease:
- Epstein-Barr virus;
- cytomegalovirus;
- cat scratch disease;
- tuberculosis;
- sexually transmitted diseases;
- bacterial infections (eg, bacterial endocarditis);
Also, lymphadenitis can be triggered by reasons of a non-infectious nature, these include:
- drug-induced lymphadenopathy;
- collagenosis of blood vessels (damage to blood vessels and tissues containing collagen);
- sarcoidosis (formation of granulomas in damaged tissues);
- local and general adenopathy;
Also, lymphadenitis can be a complication of diseases such as tonsillitis, periodontal disease, as well as other diseases associated with organs located in the ChLO (maxillofacial region).
These diseases most often cause bilateral submandibular lymphadenitis. Chronic lymphadenitis on one side, for example, on the right, may indicate the presence of such a dangerous disease as cancer.
Possible complications of submandibular lymphadenitis
Submandibular lymphadenitis is quite dangerous disease if left untreated, it can cause many different complications. Among them:
- The appearance of abscesses, abscesses in the area of inflamed nodes;
- Damage to adjacent tissues, for example, phlegmons;
- The defeat of the whole body with sepsis (blood poisoning).
Symptoms and diagnosis of lymphadenitis
 Most often, on early stages, submandibular lymphadenitis does not have any symptoms. The doctor can detect it only during a routine examination (palpation of the lymph nodes) or complaints of another disease. Among them:
Most often, on early stages, submandibular lymphadenitis does not have any symptoms. The doctor can detect it only during a routine examination (palpation of the lymph nodes) or complaints of another disease. Among them:
- Strongly enlarged soft tissue in the submandibular region;
- The appearance of pain and cyanosis in the area of the lymph nodes;
- Elevated temperature (up to 40 ° and above);
- General malaise, chills, severe sweating;
In this case, urgent treatment is necessary, otherwise the adenopathy will be of a serious nature, in which, subsequently, a fatal outcome is possible.
For correct and effective treatment a competent diagnosis of the disease is necessary. To do this, the doctor must prescribe a number of examinations:
- OAK (general blood test) and OAM (general urine test);
- Chest x-ray;
- Ultrasound of the lymph nodes;
- Mantoux test;
- Biopsy (used when cancer is suspected).
Submandibular lymphadenitis: treatment
Since many diseases can cause submandibular adenopathy, the treatment of lymphadenitis should be aimed at treating the underlying cause of this symptom. Therefore, it is necessary to treat, first of all, the disease that caused the inflammation of the nodes.
In the practice of doctors, there are 2 ways to treat lymphadenitis.
 Drug treatment
Drug treatment
Surgical intervention
In case of ineffectiveness of drug treatment or other indications (for example, allergy to penicillin or the presence of suppuration), an operation is prescribed to remove the inflamed lymph node.
Alternative methods of treatment of submandibular lymphadenitis
In addition to traditional approaches, there are folk remedies for the treatment of adenopathy. As folk remedies various herbal lotions are used for pain, as well as various teas for inflammation. Although it will not be possible to finally cure submandibular inflammation of the lymph nodes with the help of such treatment methods, they will help to relieve unpleasant symptoms.
Basics of prevention of submandibular lymphadenitis
First of all, the prevention of adenopathies of any nature is to prevent the causes and complications of infectious diseases. Do not forget that swelling of the lymph nodes is a disease of the immune system, therefore, after recovery, it is worth strengthening the immune system by hardening and taking immunomodulators.
Also, in order to prevent an exacerbation of lymphadenitis, it is worthwhile to consult a doctor in time for the correct diagnosis and prescription of treatment.
Lymph nodes play an important role as a protective barrier against bacteria, fungi and other disease-causing infections. Lymphadenitis is an enlargement of the lymph nodes against the background of their inflammation, which indicates the development of the disease. Cervical lymphadenitis affects the superficial nodes in the neck, and this makes it possible to visually detect pathologies in the early stages.
Types of cervical lymphadenitis
Cervical lymphadenitis is usually divided into two types, based on the nature and intensity of the inflammation process:
- Acute cervical lymphadenitis... In accordance with international classification diseases of the tenth revision (mkb 10), it is classified as infections of the skin and subcutaneous tissue. In medical practice, such a manifestation of the disease is indicated by the code L0, where the zero after the dot refers to the regional location (face, neck and head);
- Chronic cervical lymphadenitis... This type is often more complex in nature, according to ICB 10 it belongs to the category of diseases of the veins, lymphatic vessels and nodes. The I1 code means lymphadenitis of any type, with the exception of mesenteric lymphadenitis.
Another type is recurrent lymphadenitis. This form develops and exists due to chronic pathologies in organism.
Lymphadenitis of the neck is a frequent occurrence in children, the nodes become inflamed against the background of acute respiratory viral infections, influenza, possibly pneumonia, and does not pose a great danger.
If cervical lymphadenitis is found in adults, then this requires increased attention, since it can be the cause or consequence of a more complex disease. Moreover, in adulthood, both in women and in men, this phenomenon is rare, more often it develops, and.
Spicy
 The cause of acute lymphadenitis is external viral bacteria that have entered the lymph nodes through the bloodstream and lymph flow from lesions on the skin, acne; in connection with surgical operations.
The cause of acute lymphadenitis is external viral bacteria that have entered the lymph nodes through the bloodstream and lymph flow from lesions on the skin, acne; in connection with surgical operations.
Microorganisms in the oral cavity, lack of hygiene and even an untimely visit to the dentist are all causes of acute lymphadenitis of the face and neck. Cervical lymph nodes, being regional for this area, will be the first to take a blow and become inflamed.
In the fight against acute lymphadenitis, the main thing is the reaction, by contacting a specialist in time, you can avoid unpleasant consequences. Launched acute form in some cases it is aggravated and develops into a purulent form, or becomes a chronic process.
Chronic
The cause of chronic lymphadenitis, as mentioned above, is the acute form of this pathology, which has not received appropriate treatment on time. Chronic lymphadenitis speaks of prolonged bacterial and infectious processes in the body.
However, in order to select the necessary course of treatment, it is extremely important to establish the primary cause of the disease. Cervical lymphadenitis can occur not as a local syndrome, but as a consequence of the development of more complex diseases in the body, up to oncology (spread of metastases).
The causes of this disease
There are two types of causes: infectious and non-infectious.
If cervical lymphadenitis is diagnosed, and the examination has determined it as an independent disease, then the cause is infectious. The causative agents are various microorganisms: streptococci, staphylococci, tuberculosis sticks, fungi, HIV.
Infectious cervical lymphadenitis can be caused by damage to the head or neck. It is important that due to the superficial location of the nodes, signs of inflammation are easy to detect at an early stage. The situation is identical with the nodes in the armpit. Read more about the inflammatory processes of the axillary lymph nodes in the article
Non-infectious lymphadenitis appears against the background of other malignant pathologies in the body, often oncology. Cervical lymphadenitis is associated with lymphoma, or the formation of metastases of cancerous tumors in other areas. Non-infectious lymphadenitis can also be caused by foreign body in organism.
Symptoms
With lymphadenitis, symptoms and treatment depend on the nature of the underlying pathology, and its location in the body. A number of the main signs of inflammation are identical:
- Change in the size of the lymph nodes;
- Pain when pressed;
- Headache and general weakness;
- Inflamed cervical nodes make it difficult to swallow;
- Elevated temperature.

Cervical lymph nodes can become inflamed along with the submandibular lymph nodes, which is typical for the manifestation of symptoms of angina. Also, cervical lymphadenitis is a common symptom of a tuberculous infection.
The signs of the chronic form of pathology are identical, but they appear with some frequency over a long time.
Inflammation stages
Depending on the intensity of the inflammation, the process can develop at different rates. At the initial stages, there is a slight increase and pain syndrome on palpation, which when timely treatment leads to a quick recovery from local lymphadenitis. If the reasons are deeper, then this will lead to the ability to diagnose a dangerous disease and immediately begin treatment.
Launched lymphadenitis becomes a serious form, which is characterized by constant pain syndrome. The knots become denser and enlarge even more.
The extreme stage is acute purulent lymphadenitis, which leads to tissue damage. The human condition worsens greatly, the temperature rises to a critical level, the skin in the area of the inflamed nodes changes color.
In the stage of purulent formations, urgent hospitalization and medical supervision are required to prevent pus from entering the body.
Diagnosis of pathology
 To diagnose the disease, you should not expect an increase in the intensity of the first symptoms. Only a specialist can correctly determine the reasons.
To diagnose the disease, you should not expect an increase in the intensity of the first symptoms. Only a specialist can correctly determine the reasons.
The main methods for diagnosing lymph node pathologies are:
- Visual inspection,;
- MRI, CT, ultrasound;
- Biopsy of inflamed lymph nodes
- Conducting histological analysis.
Treatment methods
Depending on the main focus and the stage of development of the disease, a treatment method or their complex is selected. There are several ways:
- Medication;
- Physiotherapy;
- Surgical.
In the early stages of lymphadenitis, it is also necessary to adhere to simple recommendations and maintain rest, do not injure the inflamed area, drink plenty of water.
Drug treatment
If an external infection has become the cause of the development of cervical or other lymphadenitis, then antibiotics are prescribed without fail. In the case of purulent formations, the course of antibiotics can be adjusted or supplemented.
Antibiotics help to destroy the infection, as the main source of the disease, after which the lymph nodes should return to normal.
If, according to the results of the examination, a cancerous cause of lymphadenitis is revealed, then the patient is prescribed a course of chemotherapy or radiation.
Physiotherapy of cervical lymphadenitis
Among the main procedures in physiotherapy are:
- Electrophoresis (improves microcirculation in the area of inflammation);
- UHF therapy (improves immunity);
- Galvanization (used as a recovery procedure after the root cause of the disease has been eliminated).
Physiotherapy treatments are aimed at improving general condition sick. Most often they are carried out in the early stages of pathology, in combination with other methods and to accelerate the recovery processes.
Surgery
 Surgical treatment of lymphadenitis is most often used in the last stages of inflammation, when purulent formations have appeared.
Surgical treatment of lymphadenitis is most often used in the last stages of inflammation, when purulent formations have appeared.
If drug treatment does not lead to a result, then the inflamed area is opened, pus and affected tissues are removed, and drainage is performed. Antibiotics are given immediately after surgery to prevent further spread of the infection.
With the oncological nature of the disease, it is possible to remove part of the regional lymph nodes, both with lymphoma and with metastasis of tumors in other areas.
Treatment of cervical lymphadenitis with folk methods at home
There are a number folk recipes, but how to treat inflammation can only be determined by a doctor.
So, for example, the following are used as compresses:
- Baked onions with the addition of a spoonful of pharmacy tar, wrapped in cheesecloth.
- Echinacea tincture mixed with warm water in a 1: 2 ratio. It is necessary to moisten the gauze in the solution and fix the compress on the inflamed area, it is possible for the whole night.
The most popular drink is the recipe using echinacea tincture. In this case, 20-40 drops are diluted in half a glass of water, and taken orally 2-3 times a day without reference to food intake.
Prevention and prognosis
The main recommendation for the prevention of lymphadenitis is a careful attitude to one's own health. Regular visual examination and palpation of superficial lymph nodes can be carried out at home, and at the first suspicion of symptoms, consult a doctor for advice.
It is necessary to carefully monitor and handle skin lesions in order to prevent infection, undergo a dental examination.
It is recommended to exclude harmful and heavy foods from the diet as much as possible. In the case of the first signs of inflammation of the lymph nodes, do not eat dairy products, but diversify the diet with fruits, vegetables and seafood.
As with other diseases, it is important to help the body maintain immunity, take vitamin complexes.
Inflammation of the lymph nodes is characteristic of many diseases, including submandibular lymphadenitis. The reasons for its occurrence, symptoms of its appearance, methods of treatment and preventive measures.
In the human body there are several basic fluids that constantly circulate through the vessels and do not mix with each other: blood, lymph, cerebrospinal fluid (cerebrospinal fluid).
The causes of submandibular lymphadenitis
Let's start with what is it? Submandibular lymphadenitis is an inflammation of the lymph nodes located under the lower jaw, but why does it occur? The disease does not come on its own, it is one of the symptoms of any disease. V human body there are several groups of lymph nodes that are responsible for certain parts of the body.
Submandibular lymph nodes (sometimes called cervical) are responsible for the processing of lymph in the head and directly in the oral cavity. Responsible for the processing of the lymph that washes the head are: supraclavicular, occipital, anterior ear.
If the cervical lymph node is inflamed, then, most likely, the reason lies in the oral cavity or closely located respiratory organs. The main causes of the disease:
- Sharp respiratory infection bacterial or viral etiology (ARI, ARVI).
- Untreated caries.
- Complications of caries:,.
- Periodontitis or.
- Acute otitis media.
- Acute or chronic inflammation of the sinuses of the nose: frontal sinusitis, sinusitis, sinusitis.
- Chronic or acute inflammation of the pharyngeal organs: tonsillitis, pharyngitis, adenoiditis.
- Injury or other mechanical damage.
- Syphilis, tuberculosis, HIV, rheumatoid arthritis
With reduced immunity, the lymph nodes may enlarge, but soreness and seals do not occur. Most often, if the increase is small and does not bother the person too much, medical help do not apply. But a slight increase in lymph nodes may indicate a developing cancer, therefore, if even a slight seal appears, you should consult a doctor.
Symptoms
As a rule, an increase in the submandibular lymph nodes occurs against the background of acute respiratory infections or acute respiratory viral infections, therefore it is difficult to distinguish symptoms, but characteristic signs can be determined:
- an increase sometimes up to 5-7 cm in diameter, which greatly complicates swallowing;
- hurts on palpation (light pressure);
- the presence of slight redness, localized at the "top" of the inflamed lymph node.
With the progression of the underlying disease, the lymph nodes become more and more painful even at rest, thicken and more and more difficult to swallow. Other symptoms such as high fever, poor appetite, and general malaise are most likely related to the primary illness. The cervical lymph node may not be greatly increased in size, not respond to palpation, and generally not bother the patient in any way. In this case, it is necessary to consult with an otorhinolaryngologist and dentist.
Cervical lymph nodes can become inflamed with strong mechanical stress. This happens with a sharp strong squeezing of the neck. In this case, a characteristic hematoma formation at the site of compression appears to the main symptoms.
In chronic infectious processes, the lymph nodes are not greatly enlarged, not compacted, as a rule, painless on palpation. During periods of exacerbation, inflammation becomes more pronounced. V general analysis blood leukocytosis and accelerated erythrocyte sedimentation (increased ESR).
Submandibular lymphadenitis and its treatment
Adults and children with the same frequency fall ill with acute respiratory infections and acute respiratory viral infections, therefore, submandibular lymphadenitis occurs equally often at any age. Ignoring symptoms is fraught with complications. Suppuration of the inflamed lymph node may develop, which will lead to an abscess and the purulent contents will have to be evacuated.
An abscess is opened, the cavity is surgically cleaned or removed completely. If the abscess is extensive, then drainage is applied, through which the contents gradually exit. Further appointed antibiotic therapy aimed at preventing postoperative complications... UHF therapy, dry heat treatment, or a warming compress may be prescribed. It is important to carry out heat treatment only after opening the abscess in order to accelerate healing.
Lymphadenitis can occur in two forms: acute (odontogenic) and chronic (non-odontogenic). Odontogenic submandibular lymphadenitis is treated by removing the focus of infection:
- treatment of caries, pulpitis and periodontitis or removal of a diseased tooth;
- treatment of periodontitis, gingivitis, periodontal disease;
- treatment acute illness(ARI, ARVI).
It is important to carry out a complete diagnosis, because in some cases the diagnosis may not be made correctly. For example, inflammation of the salivary glands - sialoadenitis. Symptoms are similar to submandibular lymphadenitis, but besides this, there is a characteristic dry mouth and the presence of an unpleasant aftertaste.
What if the cause of the inflammation of the lymph nodes cannot be determined? It is necessary to carry out a thorough differential diagnosis, excluding serious illness(tuberculosis, syphilis, lupus erythematosus). An enlarged lymph node always speaks of inflammatory process and cannot act as an independent disease, which means that there can be no targeted treatment. It just won't be possible to remove the inflammation from the lymph node without eliminating the cause that caused it.
Antibiotics
Antibiotics for submandibular lymphadenitis can only be prescribed by the attending physician. It is very important to get qualified help with full differentiated diagnostics in order to cure qualitatively primary disease... Antibiotics are often prescribed wide range actions:
- Ceftriaxone.
- Cefixime.
- Cephalexin.
- Amoxiclav.
- Amoxicillin.
In the case of tuberculosis or syphilis, anti-syphilitic and anti-tuberculosis drugs are used. The use of antibiotics is justified only in the case of a bacterial origin of the disease. If a virus has become the causative agent, the use of antibiotics will not give the desired effect. It is necessary to take antiviral and immunity-stimulating drugs.
The patient must comply with bed rest. Shown a plentiful drink and intake of fortifying agents. Multivitamin complexes are prescribed. Any heating of the lymph nodes is excluded - this contributes to the spread of infection, generalization of the process and can lead to general blood poisoning.
Folk remedies
With the help of traditional medicine, it is also impossible to cure submandibular lymphadenitis. It is possible to alleviate the patient's condition with non-drug methods, but this cannot provide proper treatment.
- ginger tea - you need to grate the ginger root, pour hot water over it and let it brew for several hours. Lemon and honey can be added;
- infusion of echinacea is good for relieving inflammation. It can be taken internally, 50 drops per glass of water (200 ml). You can apply a compress to the site of inflammation of the lymph node. Proportions - 1: 2 tincture of echinacea to water;
- beet juice has the effect of cleansing lymph and blood. You can take it neat or mixed with celery, carrot, cabbage and basil juices;
- rosehip helps to relieve the main symptoms of intoxication with infectious disease... 100 g of dry rose hips contains over 2000 mg of vitamin C. It is a powerful antioxidant that helps to improve the functioning of all body systems.
Rosehip and ginger tea are very useful remedies in the treatment of any colds... It is very important to properly brew dried berries and grated ginger root. The water temperature should not exceed 98 ° C.
To treat gingivitis, you need to rinse regularly oral cavity... Saline solution in a concentration of 1 tablespoon of salt, preferably iodized, per 250 ml of warm water relieves inflammation well. Instead of ordinary water, you can use decoctions of calendula, chamomile, sage.
Video: submandibular lymphadenitis - what to do?
Prophylaxis
There is no specific prophylaxis for submandibular lymphadenitis. Preventive measures are to prevent the development of causes that cause inflammation of the lymph nodes.
Considering autoimmune diseases contributing to the development of submandibular lymphadenitis, then there is no prevention.
Additional questions
What is the ICD-10 code?
Most likely, submandibular lymphadenitis will be listed as L-04.0 according to ICD 10 revision. Literally it means “Acute lymphadenitis of the face, head and neck”. Common lymph node enlargement is listed as R-59, which excludes acute and chronic lymphadenitis... R-59.9 is an enlarged lymph node of unspecified etiology.
What doctor treats submandibular lymphadenitis?
Most often, therapists are involved in treatment, because it is to him that they come with the main symptoms. If the therapist doubts the diagnosis, then he sends for consultation to the otorhinolaryngologist and dentist.
Why is it dangerous?
In the normal course of the underlying disease, lymphadenitis is not dangerous. The increase goes away by itself as the patient recovers. If the lymph nodes in the neck are enlarged, but painless on palpation, the condition does not go away for more than six months, that is, there is a fear of the development of tumor formation or oncology. A biopsy and a study using tumor markers are shown.