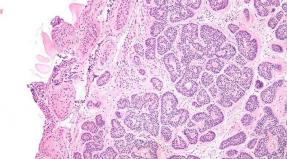
Classification and risk factors for chronic kidney disease. All about chronic renal failure: from symptoms to the prevention of XP renal failure Code on the ICD 10
Chronic renal failure (CPN) of the ICD 10 is a disease at which irreversible changes in the kidney structure occur. This leads to disorders inside the body, which is distinguished by the work of other organs. Before switching to chronic form The disease can manifest itself with sharp attacks.
Doctors allocate four pronounced diseases of the disease:
- Latent usually proceeds asymptomatic and is usually detected only when clinical studies. It is characterized by a stage is characterized by the fact that periodic proteinuria appears.
- Compensated is characterized by a decrease in glomerular filtration. During this period, weakness is noted, dry mouth, polyuria, as well as fast fatigue. Analysis reveals increased urea content and such a substance as creatinine, in the blood.
- The intermittent stage of the disease is associated with even greater decrease in filtration rate, an increase in creatinine and the development of acidosis. The patient's condition is seriously deteriorating, symptoms of diseases can appear - complications.
- The terminal stage is most serious, and therefore there are several of its stages:
- at the first stage, the water release function is preserved, and the filtering of kidney glomers is reduced to 10 ml / min. Change water balance can still be adjusted by conservative therapy;
- at the second, decompensated acidosis occurs, the fluid delay in the body comes, symptoms of hyperkathemia appear. In the cardiovascular system and the lungs there are reversible disorders;
- in the third stage, which is characterized by the same symptoms as on the second, only disorders in the lungs and the vascular system are irreversible;
- the last stage is accompanied by the liver dystrophy. Treatment at such a stage is limited, and modern methods ineffective.
The main causes of renal failure
Call chronic renal failure (CPN) Code of ICD 10 may series of factors:
- which are striking the clusters: acute and chronic glomerulonephritis, nephrosclerosis, endocarditis, malaria.
- Secondary lesions of the tissue of the organ due to vascular disorders: hypertension, stenosis of the arteries or hypertensive disease of the oncological nature.
- Diseases of urinary organs, which are characterized by urine outflows, toxins poisoning.
- Heredity. Vices for the development of the pair of organ and ureters: various cysts, hypoplasia, neuromuscular dysplasia.
Regardless of the cause of the occurrence, all changes in the kidneys are reduced to a significant decrease in the functioning tissues of the kidneys. Increased content Azotist substances makes the work of the kidneys. Since the kidneys do not cope with the load, the body begins to "self-diverge". The attacks of nausea and vomiting, muscle cramps and bone pain can appear. The skin acquires a jaundice shade, the smell of ammonia appears from the mouth.
Other causes of the disease can be:
- intolerable skin itch, most acutely manifested at night;
- increasing sweating;
- heart failure;
- arterial hypertension.
For the diagnosis of pathological disorders, a number of studies are applied:
- general I. biochemical analysis blood;
- urine study;
- Ultrasound kidneys and urinary bodies;
- cT scan;
- arteriography;
- pyelography;
- radioisotope renography.

They provide an opportunity to assess the degree of damage to the body, changing the structure, as well as identify education in the urinary system.
Most effective methods Treatment of the disease is considered:
- Hemodialysis. This is the most effective method Treatment that cleans the body from toxins using blood run through a special machine.
- Peritoneal dialysis is prescribed by patients suffering from severe diseases that have the intolerance to heparin. The mechanism is to introduce a solution in the peritoneum and bringing it through the catheter.
- The most cardinal is the kidney transplantation.
As preventive treatment Applied conservative therapy With several types of preparations:
- corticosteroids (methylprednisolone);
- antilimphocytic globulin;
- cytostatic (Imuran, Azatioprin);
- anticoagulants (heparin);
- antiagregants (Kuraltil, Trental);
- vasodialators;
- antibacterial drugs (Neomycin, streptomycin, kanamycin).

Before applying any drugs, it is necessary to undergo a full examination, as it is possible to choose a better treatment scheme can only professional specialist.
Treatment of the disease with the help of popular recipes and prevention
How to spend? Lots of medicinal plants Can take symptoms. The most common recipes:
- collected from the following ingredients:
- Brusnel sheets.
- Violet.
- Flax seeds.
- Linden blossom.
- Corn silk.
- Motherwort.
- Truck.
- Blueberry.
- Rephetka.
- collecting from the fruits of a hawthorn, nettle, laurel, chamomile, rosehip, dill and currants;
- collection made from birch leaf, calendula, hunter, viburnum, dyeing, mint, sage and apples peel;
- each of them has a beneficial effect on the state of the urinary system, support the function of the kidneys.
For people prone to the development of kidney disease, it is important to comply with some prevention measures:
- refusal of cigarettes and alcohol;
- development and compliance with low cholesterol and fats diet;
- physical exercise, beneficially affecting the patient's condition;
- control over cholesterol and blood sugar levels;
- regulation of fluid consumed;
- limitation of salt and protein in the diet;
- providing a full sleep.
All this will help support functionality. internal organs and improve the overall condition of the patient.
The term "chronic kidney disease" (HBP) appeared recently - a previously similar condition was called chronic kidney failure.
It is not a separate disease, but syndrome, that is, a complex of disorders that are observed in a patient for three months.
According to statistics, the disease occurs about 10% of people, and it is subject to both women and men.
 The factors that cause kidney dysfunction exists quite a lot, the most probable causes include:
The factors that cause kidney dysfunction exists quite a lot, the most probable causes include:
- arterial hypertension. Constantly increased blood pressure and violations that accompany hypertension causes chronic insufficiency;
- diabetes. The development of diabetes mellitus provokes diabetic kidney damage, which leads to chronic disease;
- age changes in the body. For most people, after 75 years, HBS develops, but if there are no accompanying diseases, the syndrome does not lead to serious consequences.
In addition, HBS can provoke states that are associated with kidney dysfunction and (renal artery stenosis, urine outflow disturbances, polycystic diseases, infectious diseases), poisoning, accompanied by kidney damage, autoimmune diseases, obesity.
The arterial hypertension and the work of the kidneys are directly related to each other - people with a diagnosis of HBE eventually cause problems with arterial pressure.Symptoms
In the first and second stage of the disease, it does not exhibit itself, which makes it difficult to make a diagnosis.
 As the alert progresses, other signs appear, including:
As the alert progresses, other signs appear, including:
- fast and inexplicable weight loss, decline in appetite, anemia;
- reducing performance, weakness;
- pallor of skin, dryness and irritation;
- the appearance of edema (limbs, face);
- , reducing the amount of urine;
- dry language, ulceration of mucous membranes.
Most of these symptoms are perceived by patients as signs of other ailments or ordinary overwriting, but if they continue for several months, you should consult a doctor as soon as possible.
Characteristic features of HBS are stable with the corresponding symptoms and a violation of the outflow of urine.Classification
The pathological process is developing gradually, sometimes for several years. Passing through several stages.
 With such pathology, as chronic kidney disease, the stages are allocated as follows:
With such pathology, as chronic kidney disease, the stages are allocated as follows:
- initial. Analyzes of the patient at this stage may not show major changes, but there is already dysfunction. Complaints, as a rule, are also absent - a small decrease in performance and the participation of urges for urination is possible (usually at night);
- compensated. The patient often gets tired, feeling drowsiness and overall malaise, begins to drink more liquid and more often go to the toilet. Most analyzing indicators may also be within the normal range, but dysfunction progresses;
- intermittent. Signs of the disease are growing, become pronounced. The appetite of the patient is worsening, skin covers become pale and dry, sometimes blood pressure rises. In blood test at this stage increases the level of urea and creatinine;
- terminal. A person becomes sluggish, feels permanent drowsiness, skin covers become yellow and flabby. In the body is disturbed by water electrolyte balanceThe work of organs and systems is violated, which can lead to early death.
Diagnostics
The diagnosis of HBS is raised on the basis of a study complex, which include (general, biochemical, Zimnitsky) and blood, and CT, isotopic scintigraphy.

Isotopic scintigraphy
The presence of the disease may indicate protein in the urine (proteinuria), an increase in the size of the kidneys, and tumors in tissues, violation of functions.
One of the most informative studies to identify the HBA and its stage is to determine the speed of glomerular filtration (SCF). A significant reduction in this indicator can speak about the HBE, and the lower the speed, the stronger the kidneys are affected. According to the level of SCF, chronic kidney disease has 5 stages.
The decrease in the SCF to 15-29 units and below indicates the last stages of the disease, which carries a direct threat to human life.What is dangerous renal failure?
 In addition to the risk of transition of the disease in the terminal stage, which carries with them the risk of death, the HCB may cause a number of serious complications:
In addition to the risk of transition of the disease in the terminal stage, which carries with them the risk of death, the HCB may cause a number of serious complications:
- disorders of the cardiovascular system (myocarditis, pericarditis, stagnant heart failure);
- anemia, blood clotting disruption;
- target diseases, including ulcers duodenal gut and stomach, gastritis;
- osteoporosis, arthritis, bone deformation.
Treatment
HBS therapy includes treatment primary diseasewhich caused the syndrome, as well as maintaining the normal kidney function and their protection. Russia has regarding chronic kidney disease National Recommendationscreated by experts of the scientific community of nephropologists of the Russian Federation.
 Chronic kidney disease treatment implies the following:
Chronic kidney disease treatment implies the following:
- reduced load on healthy kidney fabrics;
- correction of violation of the electrolyte balance and metabolic processes;
- purification of blood from toxins and decay products (,);
- replacement therapy, organ transplantation.
If a parable is detected at a compensated stage, the patient is prescribed operational treatmentwhich restores the normal stroke of urine and returns the disease to the latent (initial) stage.
On the third (inthyrmitting) stage of the HBA, surgical intervention is not carried out, as it is associated with a large risk for the patient. Most often, in this case, palliative treatment techniques are used, which facilitate the patient's condition, and the organism detoxification is also carried out. Operation is possible only if the kidney function is restored.
 Approximately 4 times a year, all patients with HBA recommended infusion treatment under hospital conditions: the introduction of glucose, diuretic products, anabolic steroids, vitamins.
Approximately 4 times a year, all patients with HBA recommended infusion treatment under hospital conditions: the introduction of glucose, diuretic products, anabolic steroids, vitamins.
With chronic kidney disease, hemodialysis is carried out in chronic times in a few days, and people with severe concomitant pathologies and intolerance to heparin are peritoneal dialysis.
The most radical method of treatment of HBS is the organ transplantation, which is carried out in specialized centers. This is a complex operation that requires the tissue compatibility of the donor and the recipient, as well as the lack of contraindications to intervention.Prevention
To reduce the risk of developing HBS, it is necessary to follow the following rules:- balance the diet, abandon fat, smoked and sharp dishes, reduce the consumption of animal protein and salt;
- in time to treat infectious diseases, especially diseases of the urogenital system;
- reduce physical exertion, if possible, avoid psycho-emotional stress;
- The pathology of the cardiovascular system, which violate the process of blood supply to all organs, including kidneys:
- arrhythmia;
- atherosclerosis;
- heart failure.
- Dehydration Against the background of the subsequent ailments, which is the cause of changes in blood indicators, or rather, the increase in its prothrombin index, and, as a result, the difficult operation of the glomeruli:
- dyspeptic syndrome;
- extensive burns;
- blood loss.
- Anaphylactic shock, which is accompanied by a sharp decrease in blood pressure indicators, which negatively affects the work of the kidneys.
- Acute inflammatory phenomena in the kidneys, which lead to damage to the tissues of organs:
- pyelonephritis.
- Physical obstacle for urine outflows under urolithiasis, which first leads to hydronephrosis, and then due to pressure on the kidney tissue, damage to the tissues.
- Reception of nephrotoxic drugs, to which the contrasting composition includes X-ray, it becomes the cause of the body poisoning, with which the kidneys cannot cope.
- Preenal OPN - the cause of the ailment is not directly interconnected with the kidneys. The most popular example of the preenal type of OPN can be called violations in the heart of the heart, because the pathology is often called hemodynamic. Less often it occurs against the background of dehydration.
- Renal acute renal failure - the root cause of pathology can be found in the kidneys themselves, in connection with which the second name of the category is parenchymal. Renal functional insufficiency in most cases follows from acute glomerulonephritis.
- The launched OPN (obstructive) is a form that occurs when the conversion paths of urin with the concretions and the subsequent violation of urine outflows.
- initial stage;
- oliguric stage;
- polyuric stage;
- recovery.
- loss of forces;
- headache.
- With oliguric syndrome, on the background of OPN, symptoms become specific, easily recognizable and stacked in the overall picture of pathology:
- reducing diurea;
- dark foaming urine;
- dyspepsia;
- inhibition;
- warms in the chest due to fluid in the lungs;
- exposure to infections due to reduced immunity.
- Polyuric (diuretic) stage is characterized by an increase in the amount of urine allocated, so all patient complaints flow from this fact, and the fact that the body loses a large number of potassium and sodium with urinous organism:
- violations in the heart of the heart are recorded;
- hypotension.
- The period of recovery, occupying from 6 months to one year, is characterized by fatigue, changes in the results of laboratory urine research (specific gravity, red blood cells, protein), blood (general protein, hemoglobin, EE, urea,).
- survey and examination of the patient makes it an anamnesis;
- clinical analysis of blood showing reduced hemoglobin;
- biochemical blood test, with which elevated creatinine, potassium, urea is revealed;
- monitoring Diurea, that is, control over how much fluid (including soups, fruits) consumes a person in 24 hours, and how much it highlights;
- the ultrasound method, with the OPN often showing the physiological sizes of the kidneys, the decrease in size indicators is a bad sign that speakers the damage to the tissues that may be irreversible;
- nephrobiopsy - fence piece of organ with a long needle for microscopic research; carried out infrequently due to high degree traumatic.
- The identification of the root cause of the pathological state is carried out with the help of diagnostic methods, the study of symptoms, specific patient complaints.
- Elimination of the reasons for OPN - the most important stage of treatment, because without the treatment of the root causes of the disease, any measure of therapy will be ineffective:
- in identifying the negative influence of nephrotoxins on the kidneys, an extracorporeal hemocorrection is used;
- when the autoimmune factor is detected, glucocorticosteroids ("prednisolone", "Methipred", "Predizol") and Plasmapheresis are prescribed.
- with urolithiasis, drug litholism or surgical intervention is carried out to remove the calculation;
- in infection, antibiotics are prescribed.
- violation of cardiovascular activities;
- anemia;
- increased risk of infections;
- neurological violations;
- dyspeptic disorders;
- uremic coma.
- Avoid receiving nephrotoxic medicines.
- Timilely treat chronic ailments of urinary and vascular system.
- Monitor indicators arterial pressureWhen identifying signs of chronic hypertension, immediately refer to a specialist.
- Latent usually proceeds asymptomatic and is usually detected only with clinical studies. It is characterized by a stage is characterized by the fact that periodic proteinuria appears.
- Compensated is characterized by a decrease in glomerular filtration. During this period, weakness is noted, dry mouth, polyuria, as well as fast fatigue. Analysis reveals increased urea content and such a substance as creatinine, in the blood.
- The intermittent stage of the disease is associated with even greater decrease in filtration rate, an increase in creatinine and the development of acidosis. The patient's condition is seriously deteriorating, symptoms of diseases can appear - complications.
- The terminal stage is most serious, and therefore there are several of its stages:
- at the first stage, the water release function is preserved, and the filtering of kidney glomers is reduced to 10 ml / min. Water balance changes can still be adjusted using conservative therapy;
- at the second, decompensated acidosis occurs, the fluid delay in the body comes, symptoms of hyperkathemia appear. In the cardiovascular system and the lungs there are reversible disorders;
- in the third stage, which is characterized by the same symptoms as on the second, only disorders in the lungs and the vascular system are irreversible;
- the last stage is accompanied by the liver dystrophy. Treatment at such a stage is limited, and modern methods are ineffective.
- Expert opinion: Today it is one of the most effective tools In the treatment of kidney disease. I have been using German droplets in my practice for a long time ...
- Diseases of the kidneys that are affixed by the clusters: acute and chronic glomerulonephritis, nephrosclerosis, endocarditis, malaria.
- Secondary lesions of the tissue of the organ due to vascular disorders: hypertension, stenosis of the arteries or hypertensive disease of the oncological nature.
- Diseases of urinary organs, which are characterized by urine outflows, toxins poisoning.
- Heredity. Vices for the development of the pair of organ and ureters: various cysts, hypoplasia, neuromuscular dysplasia.
- unbearable skin itching, most acutely manifested at night;
- increasing sweating;
- heart failure;
- arterial hypertension.
- general and biochemical blood test;
- urine study;
- Ultrasound kidneys and urinary bodies;
- cT scan;
- arteriography;
- pyelography;
- radioisotope renography.
- Hemodialysis. This is the most effective method of treatment that purifies the body from toxins using blood run through a special device.
- Peritoneal dialysis is prescribed by patients suffering from severe diseases that have the intolerance to heparin. The mechanism is to introduce a solution in the peritoneum and bringing it through the catheter.
- The most cardinal is the kidney transplantation.
- corticosteroids (methylprednisolone);
- antilimphocytic globulin;
- cytostatic (Imuran, Azatioprin);
- anticoagulants (heparin);
- antiagregants (Kuraltil, Trental);
- vasodialators;
- antibacterial drugs (neomycin, streptomycin, kanamycin).
- collected from the following ingredients:
- Brusnel sheets.
- Violet.
- Flax seeds.
- Linden blossom.
- Corn silk.
- Motherwort.
- Truck.
- Blueberry.
- Rephetka.
- collecting from the fruits of a hawthorn, nettle, laurel, chamomile, rosehip, dill and currants;
- collection made from birch leaf, calendula, hunter, viburnum, dyeing, mint, sage and apples peel;
- each of them has a beneficial effect on the state of the urinary system, support the function of the kidneys.
- refusal of cigarettes and alcohol;
- development and compliance with low cholesterol and fats diet;
- physical exertion, beneficially affecting the patient's condition;
- control over cholesterol and blood sugar levels;
- regulation of fluid consumed;
- limitation of salt and protein in the diet;
- providing a full sleep.
- It is important to know! The kidneys will be cleaned instantly if there is an empty stomach in the morning ... a unique health recipe from Germany!
- Deviations in blood studies (creatinine, urea, electrolyte flaws).
- Change in urinic analysis indicators (hematuria, leukocyturia, proteinuria).
- Speed \u200b\u200bof glomerular filtration.
- Structural deviations of the kidneys (ultrasound, X-ray examination).
- Diabetes. Each person has friends or acquaintances having a blood sugar deficit. This is one of the most common diseases on the planet.
- Nephrolithiasis - a disease in which they determine the presence of stones in the kidneys.
- Glomerulonephritis - while this pathology is amazed by the balls of kidneys and another structure of the fabric.
- Pyelonephritis is an inflammatory disease that affects the kidney fabrics due to the penetration of pathogenic microflora.
- Pathology of vessels - hypertension, stenosis.
- Gapoplasia - kidney spell expressed by a decrease.
- tracheitis;
- pleurisy;
- bronchopneumonia.
- 1. Clinical recommendations. Formulary. Vol. 1. Publishing house "Geotar-Honey", 2004. 2. Jukka Mustonen, Treatment of Chronic Renal Failure. EBM Guidelines 11.6.2005. www.ebmguidelines.com 3. Proof medicine. Clinical recommendations for practical doctors based on evidence-based medicine. 2 ed. Geotar, 2002.
- By self-medication, you can apply irreparable harm to your health.
- The information posted on the MedElement website and in MEDElement mobile applications, "Lekar Pro", "Dariger Pro", "Diseases: Therapist's Directory", cannot and should not replace a full-time doctor consultation. Be sure to contact B. medical institutions If there are any diseases or disturbing symptoms.
- Choice medicines And their dosages should be agreed with a specialist. Only a doctor can prescribe the necessary medicine and its dosage, taking into account the disease and the state of the patient's body.
- Website MedElement and Mobile Applications "MedElement (Medleylement)", "Lekar Pro", "Dariger Pro", "Diseases: Directory of Therapist" are exclusively information and reference resources. The information posted on this site should not be used for unauthorized changes to the doctor's prescriptions.
- The editorial office of MedElement is not responsible for any damage to health or material damage resulting from the use of this site.
Acute renal failure (OPN) - fast, but reversible, depression of renal function, sometimes before the stage of complete failure of one or both of the organs. The pathology is deservedly characterized as a critical state that requires immediate intervention of physicians. Otherwise, the risk of adverse outcome in the form of loss of organs of organs is much increasing.
Acute renal failure
The kidneys are the main "filters" of the human body, the neubrahons of which are continuously passed through their blood membranes, deriving excess liquid and toxins with urinus, sending the necessary substances back to the bloodstream.
Kidneys - organs, without which human life is impossible. Therefore, in that situation, when they cease to carry out their under the influence of provoking factors functional task, Doctors provide a person emergency medical care, putting him a diagnosis - acute renal failure. Code of somatic pathology on the ICD-10 - N17.
To date, statistical information makes it clear that the number of people encountered with this pathology is growing every year.
Etiology
The reasons for djpybryjdtybz acute renal failure are as follows:
OPON classification
The process of acute kidney failure is divided into three types:
Classification of acute renal failure
Pathogenesis
OPON develops for four periods that always follow in the specified order:
The duration of the first stage can last from several hours to several days, depending on what is the root cause of the alend.
Oliguria is a term, with the help of which briefly indicate a decrease in the volume of urins. Normally, a person must distinguish approximately the amount of fluid that used, minus part, "spent" by the body for sweating and breathing. With Oliguria, the volume of urins becomes less than half a liter, out of a direct connection from the amount of drilled liquid, which entails increasing in the tissues of the body of the fluid and decay products.
The complete disappearance of diuresis -, it happens only in extremely severe cases. And it rarely happened statistically.
The duration of the first stage depends on how quickly adequate treatment has begun.
Polyuria, on the contrary, means an increase in diuresis, in other words, the amount of urine can reach five liters, although 2 liters of urine per day are already a reason for the diagnosis of polyuric syndrome. This stage lasts about 10 days, and its main danger is that loss of substances necessary to it with urine, as well as dehydration.
After the completion of the polyuric stage, a person, with a favorable development of the situation, recovering. However, it is important to know that this period can delay for one year, during which deviations will be detected in deciphering analyzes.
Stage OPON 
Clinical picture
The initial stage of the OPN does not have specific symptoms, on which it was possible to recognize the illness, the main complaints during this period are:
The symptomatic picture is complemented by signs of pathology that caused OPN:
Diagnostics
The diagnosis of the OPN is carried out using:
Treatment
Therapy of the OPN takes place in the resuscitation department of the hospital, less often - in the nephrological department of the hospital.
All therapeutic manipulations conducted by a doctor and medical staff can be divided into two stages:
At each stage, the doctor adjusts the appointment, based on the symptomatic picture at the moment.
During Oliguria, it is necessary to appoint diuretics, a strict diet with a minimum amount of protein and potassium, if necessary, hemodialysis.
Hemodialysis - the procedure for cleansing blood from the decay products and removal of excess fluid from the body, has an ambiguous attitude of nephropologists. Some doctors argue that preventive hemodialysis is needed in order to reduce the risk of complications. Other specialists warn about the trends of full loss of kidney function from the moment of the use of artificial blood purification.
During the period of polyuria, it is important to fill in the patient the missing blood volume in the patient, to restore the electrolyte balance in the body, continue diet No. 4, take care of any infection, especially when taking hormonal drugs.
General principles of treatment OPN 
Forecasts and complications
OPON Against the background of proper treatment, it has a favorable forecast: after a submitted agence, only 2% of patients need life hemodialysis.
Complications from acute kidney failure are associated with, that is, with the process of organism poisoning with its own decay products. As a result, the latter are not removed by the kidneys under oliguria or with a small blood filtration rate by glomers.
Pathology leads to:
It is important to note that with acute nephrological failure, in contrast to chronic, complications rarely occur.
Prevention
The prevention of the OPN is as follows:
On video about the causes, symptoms and treatment of acute renal failure:
The human body is a reasonable and fairly balanced mechanism.

Among all famous science infectious diseases, infectious mononucleosis is given a special place ...

About the disease that official medicine calls "angina region", the world has already been known for a long time.

Pig (scientific name - epidemic vapotitis) is called an infectious disease ...

The hepatic colic is a typical manifestation of gallstone disease.

The edema of the brain is the consequences of excessive loads of the body.

There are no people in the world who have never been sick orvi (acute respiratory viral diseases) ...

A healthy human body is able to assimage as many salts obtained with water and food ...
Bursitis knee Sustava It is a widespread disease among athletes ...
Chronic kidney disease Code on the ICD 10
Chronic renal failure
Diagnostic criteria
Complaints and history: symptoms of chronic kidney disease or characteristic CPN syndromes (hematuria, swelling, ag, dysuria, lower back pain, bones, niccountura, lag in physical development, bone deformation).
Physical examination: itching, calculations, urinary smell of mouth, dry skin, pallor, niccountura and polyuria, ag.
Laboratory studies: anemia, hyperphosphatemia, hyperparathyroidism, an increase in urea and creatinine levels, OAM - Isostenuria, SCF less than 60 ml / min.
Tools:
Ultrasound of the kidneys: no, decrease in size, change in the shape of the kidneys, irregularity of contours, the expansion of collective kidney systems, ureters, increase the echogenicity of parenchyma;
Doppler Kidney Vessels - Detection of Bloodstock;
Cystography - bubble-ureteral reflux or state after an antirefluxus operation;
NEFROMYCINTIGRAPHY - Foci of sclerosis of the kidneys, reducing the excretory and evacuation function of the kidneys.
Indications for consultation of specialists:
ENT doctor; - dentist;
Gynecologist - for the sanitation of the nasopharynx infection, oral cavity and external genital organs;
Okulist - to assess changes in microsuds;
Pronounced arterial hypertension, violations by the ECG, etc. are an indication for consulting a cardiologist;
In the presence of viral hepatitis, zoonotic and intrauterine and other infection - infectious diseases.
List of basic diagnostic events:
General analysis blood (6 parameters);
General urine analysis;
Urine analysis in Zimnitsky;
Rebarga's test;
Determination of residual nitrogen;
Determination of creatinine, urea, intact hospital hormone, kSHS;
Defining potassium / sodium.
Calcium definition;
Determination of chlorides;
Magnesium definition; - definition of phosphorus;
The level of syrontary ferritin and serum iron, the saturation coefficient of transferlic iron;
Uzi organs abdominal cavity;
USDG vessels.
List of additional diagnostic events:
Determination of glucose, free iron, the number of hypochromic erythrocytes;
Coagulogram 1 (prothrombin time, fibrinogen, thrombin time, APTTV, fibrinolytic plasma activity, hematocrit);
Definition of Alt, Ast, Bilirubin, Timol Sample;
IFA markers vg;
Determination of common lipids, cholesterol and lipid fractions;
CT scan;
Consultation ophthalmologist.
deseass.medElement.com.
CPN (chronic renal failure) - code on the ICD 10
CPN MKB 10 - What does this code mean and how to deal with it?
Chronic renal failure (CPN) of the ICD 10 is a disease at which irreversible changes in the kidney structure occur. This leads to disorders inside the body, which is distinguished by the work of other organs. Before moving into a chronic form, the disease can manifest itself with sharp attacks.
Medications
Expand
Doctors allocate four pronounced diseases of the disease:

Call chronic renal failure (CPN) Code of ICD 10 may series of factors:
Regardless of the cause of the occurrence, all changes in the kidneys are reduced to a significant decrease in the functioning tissues of the kidneys. Increased content of nitrogen substances makes the kidney work. Since the kidneys do not cope with the load, the body begins to "self-diverge". The attacks of nausea and vomiting, muscle cramps and bone pain can appear. The skin acquires a jaundice shade, the smell of ammonia appears from the mouth.
Other causes of the disease can be:
For the diagnosis of pathological disorders, a number of studies are applied:

They provide an opportunity to assess the degree of damage to the body, changing the structure, as well as identify education in the urinary system.
The most effective methods of treating the disease are considered:
Conservative therapy applies to the use of several types of preparations as preventive treatment:

Before applying any drugs, it is necessary to undergo a full examination, as it is possible to choose a better treatment scheme can only professional specialist.
How do kidney treatment at home folk remedies? Many medicinal plants can withdraw symptoms. The most common recipes:
For people prone to the development of kidney disease, it is important to comply with some prevention measures:
All this will help maintain the functionality of the internal organs and improve the overall condition of the patient.

Urgent states
What is urethral fistula
pochke.ru.
The appearance and value of the wording of the HBP
Chronic kidney disease is modern classificationwhich determines the presence of various pathological changes that exist in the human body for 3 months.
Changes can be manifested in urine and blood studies, with kidney biopsies or tool examination of the body.
In itself, the concept of chronic disease cannot be attributed to the exact diagnosis of the renal status. Rather, this is a medical and social formulation. An unequivocal criterion showing the deviation in the work of the kidney is the speed of glomerular filtration (SCF).
Earlier, the diagnosis of "chronic renal failure" was put in the patient at the initial stage of chronic kidney disease. At the same time, the first stages of CPN were ignored and did not fall under the concept of any pathology. This nature of the change can lead to the terminal stage with all the ensuing consequences.
Thus, the diagnosis of HBS was introduced for early diagnosis of damage to the kidneys, by identifying initial stages Diseases using the CRP. This allows you to prevent the development of potential complications to increase the working capacity of the kidneys.
Generally accepted classification of HBC
To determine kidney diseases, several indicators are used to estimate the functionality of the organ:
One of the exact indicators when determining the kidney function is the speed of glomerular filtration. The SCF determines the mass of the operating nephrons and takes into account the mass of the body, sexuality, age framework.
A few classifications are adopted in chronic kidney disease. But the common and relevant - the classification of KDOQI, it is used since 2002 and takes into account the indicator of the SCF. The classification of chronic kidney disease, which takes into account the indicator of the SCF represents five stages.
Chronic kidney disease stage:
When the patient, the SCF is permissible, but there are damage on other indicators, for example, in urine or blood analyzes, then the first stage takes place. Various diseases of the kidneys at a certain point acquire a similar degree of damage. With chronic kidney disease - the 3rd stage. At this stage, whatever the pathology of the kidney does not arise, people have the same mechanisms for the progression of the disease.
At this stage, the intervention of the nephrologist is necessary to assign protective therapy to prevent the progression of the disease. Therefore, the first 3 stages in the magnitude of the SCF are for the patient a certain indicator followed by a significant deterioration in his health and lifestyle.
The indicator of SCF less than 60 means the death of about half of the nephron. In the framework of Russian terminology, the last three stages of chronic kidney disease are classified as chronic renal failure.
Manifestations and clinical consequences
Chronic kidney disease is mainly characterized by the progress of the main disease caused the development of pathology. With renal disease, changes occur in organism organs under the influence of toxic products. It is known about 200 substances of the increasing disease, with their accumulation.
The first stages of the disease can be accompanied by very weak symptoms or with its complete absence. Only after the reinforced effect on the kidneys: excessive use of salt, low-alcohol drinks, can manifest itself in the form of swelling on face, fatigue and weakness.
The strengthening of the main disease leads to a general deterioration of the patient's condition, and in violation of the work of many organs. Nikturia appears, polyuria, dry mouth. The skin of patients with HZP acquires a yellowish tint, becomes more dry. There is a significant reduction in the intensity of sweating due to atrophy of the sweat glands. The patient has nausea, vomit, generalized and skin itching with strong intensity, feeling of an indefinite taste in oral cavity.
In the body of the patient there is a liquid accumulation, which can cause congestive heart failure. Stagnation of the liquid is aggravated when hypertensive disease appears. This disease faces an overwhelming number of patients at the late stage of renal disease.
Renal failure leads to chronic uremia, which arises due to intoxication of the body. One of the symptoms with this pathology is lethargy, apathy, drowsiness. Tissue hypoxia is the result of chronic uremia. It manifests itself as a result of the isolation of the urea with then on the skin of the patient, the resulting the ventilation ability of the lungs is reduced and the process is disturbed. metabolic acidosis.
The violation of the functional feature of the kidneys leads to a decrease in the antitoxic function of the liver. The close relationship of organs in chronic kidney disease entails a failure in protein and carbohydrate exchange.
Disorders in the field of the CSS are played by a significant role in the HCB. Cardiovascular dysfunction for third patients acts as a causal factor in the death of patients at the thermal stage of the disease.
The degree of cardiac pathology determines the course of treatment in the later stages of chronic kidney disease. The lack of oxygen in the delay in poisoning substances during kidney disease (uremia) is very strongly affected by the work of the heart muscle. Failure of acid-alkaline balance, water balance disruption, acidosis - factors provoke various violations of the heart rhythm. Hemodialysis causes a significant reduction in blood pressure indicators, which further increases the frequency of arrhythmia.
Chronic kidney disease leads to the malfunction of the operation of the gastrointestinal tract. It becomes the cause of the constant release of urea, ammonia, creatinine, and this entails the manifestation of such symptoms as: a metal taste in the oral cavity, a vomiting urge, stomatitis develops.
Most patients with renal pathology observes anemia. On the latter, the terminal stage of anemia is already available in 100% of cases. The source of anemia in chronic kidney disease is: deterioration of bone marrow activity, increased bleeding against hemodialysis, decreases the volume of erythropoietin produced by the kidneys.
What diseases cause HBS
As mentioned above, the designation "Chronic disease" is not a separate diagnosis that determines the pathological change in the kidneys. This term in modern medicine was introduced to determine the degree of progression of the underlying disease directly affecting the kidney.
Frequent primary diseases include:
Late stages of the progress of kidney disease are accompanied by pulmonary diseases:
Pulmonological and cardiovascular pathologies cause the manifestation of pneumonia and edema of the lungs.
Risk factors
Risk factors for renal failure include not only diseases accompanying diseases, but also phenomena that negatively affect the course of the disease. These factors enhance the flow of pathology and increase the risk of further worsening the patient's health. Therefore, facing them, the elimination of these phenomena comes to the first place to reduce the progress of renal pathology.
But not all risks can be eliminated or prevented.
These include:
Considering these factors it can be noted that patients with age are more susceptible to the risk of the disease, and the genetic predisposition - well, God himself ordered. Paul patient can play a role in the appearance of a causal factor, such as women, are more susceptible to the diseases of the lower urinary tract.
Banal smoking and alcoholism can be attributed to the risks of the risks of "artificial". The refusal to smoking may well be a pledge to reduce progress in the development of renal failure, it has also been proven that smokers increases the risk of renal pathologies.
The close relationship of changes in kidneys with diseases of the vessels leads to a hazardous increase in the concentrations of low density lipoproteins in the human body. Such a complication entails the development of atherosclerosis.
It is impossible to get rid of the blockage of blood vessels without operational effect. The cause of cholesterol will be overweight. Therefore, the normalization of cholesterol level is an important component in renal pathology.
HBS in children
A distinctive feature Chronic kidney diseases in children are congenital pathologies. There is a notion of chronic renal failure in children. The baby has no kidneys from birth. A child with pathology from birth passes replacement therapy. It includes types of dialysis or kidney transplant.
Chronic kidney disease in children does not always proceed with a pronounced clinic and depends on the primary disease. If the cause is congenital diseases, then there may be a lag in physical development and a ricket-like change in bone.
Main pledge successful treatment It will depend on the tight cooperation of parents with a doctor. All recommendations of the attending physician at the reception of drugs and testing are required. Preparations will be appointed depending on the disease caused renal failure. Therefore, it is necessary to comply with all recommendations for the correction of violations identified on different stages renal disease.
Treatment of HBC
 When it comes to the treatment of renal pathologies, the motivation of American nephrologists becomes clear, which introduced the concept of "chronic kidney disease". Before appointing therapy, the main role is played by the diagnosis of deviations on the CRF criterion.
When it comes to the treatment of renal pathologies, the motivation of American nephrologists becomes clear, which introduced the concept of "chronic kidney disease". Before appointing therapy, the main role is played by the diagnosis of deviations on the CRF criterion.
The first stage means that this indicator does not have deviations from the norm, but there are deviations in the diagnosis of other markers (urine or blood analysis). Treatment in this case is aimed at eliminating the concomitant pathology.
The second stage is characterized by some decrease in glomerular filtration rate. For this stage, the main thing is to assess the reduction of nephrons, assess the risks of further complication. It is the first stages that the sign of the nephrologists that the patient should be taken into account, for the possible prevention of complications.
The third stage according to the generally accepted Russian classification means the beginning of CPN. The causal factor enhances the frequency of metabolic disorders and requires treatment-controlled by a specialist.
The fourth and fifth stage require the urgent intervention of the nephrologist's doctor, and renal therapy or hemodialysis are carried out, respectively.
Chronic kidney disease and its treatment will be to eliminate the reasons for reducing nephrons. This requires a reduction in the load on already active nephrons. Medicia treatment allowing you to restore mineral and electrolyte imbalance. Polyfepan preparation allows you to correct an imbalance with renal pathology. For the removal of potassium from the body prescribe ebys and laxatives. For the correction of homeostasis, drug therapy is prescribed: a solution of glucose, diuretic drugs, vitamins B, C.
Hemodialysis is carried out to replace the work of the kidneys. This is the most effective, but at the same time a fairly costly method.
The next step after hemodialysis is kidney transplantation. This method is the most radical and is carried out in specialized clinics.
In the clinics, a nephrologist is very rare. Patients for the most part go to therapists or urologists. Conducted by early stages Diagnostics and therapy makes it possible to further avoid complications and huge costs associated with them.
wMedik.ru.
Compliance with the stages of chronic kidney disease encoding MKB-10
| Stage HBC | ICB-10 code |
| Stage is not clarified |
Implementation in real clinical practice Key approaches to the diagnosis of HBS had important consequences. Over the ten years that have passed since the adoption of the HBS concept, awareness and alertness of the doctors of various specialties in relation to the HBA as a significant health problem has increased significantly. The introduction of the automatic calculation of the SCF in laboratories and the inclusion of its value into the results of a laboratory study in addition to the level of creatinine serum contributed to an increase in the primary appeal to the nephrologist of patients with HBP by 68.4%.
The use of categories of the SCF and albuminuria allows you to strateg the patients with HBE risk risk (decrease in the SCF, the progression of albuminuria, OPP, TPN) and other complications (cardiovascular morbidity and mortality, endocrine and metabolic disorders, drug toxicity) (Table 5).
Table 5.
Combined risk of the progression of HBC and the development of cardiovascular complications, depending on the degree of decrease in the SCF and the severity of Albuminuria
| Albuminuria** |
|||||||||||||||||||||||
| Optimal or slightly elevated | Very high |
||||||||||||||||||||||
| 30 mg / mol |
|||||||||||||||||||||||
| High or optimal | Moderate | ||||||||||||||||||||||
| Slightly reduced | Moderate | ||||||||||||||||||||||
| Moderately reduced | Moderate | Very tall |
|||||||||||||||||||||
| Significantly reduced | Very tall | Very tall |
|||||||||||||||||||||
| Sharply reduced | Very tall | Very tall | Very tall |
||||||||||||||||||||
| Renal failure |
RCRZ (Republican Center for Health Development MD RK) Chronic renal failure uncomfortable (N18.9) general informationShort description Protocol code: H-T-028 "Chronic renal failure" ClassificationNKF K-DOQI (National Kidney Foundation - Kidney Disease Outcomes Quality Initiative) DiagnosticsDiagnostic criteria Physical examination: Itching, calculations, urinary smell of mouth, dry skin, pallor, niccountura and polyuria, ag. Ultrasound of the kidneys: no, decrease in size, change in the shape of the kidneys, irregularity of contours, the expansion of collective kidney systems, ureters, increase the echogenicity of parenchyma; Doppler Kidney Vessels - Detection of Bloodstock; Cystography - bubble-ureteral reflux or state after an antirefluxus operation; NEFROMYCINTIGRAPHY - Foci of sclerosis of the kidneys, reducing the excretory and evacuation function of the kidneys. ENT doctor; Okulist - to assess changes in microsuds; Pronounced arterial hypertension, violations by the ECG, etc. are an indication for consulting a cardiologist; In the presence of viral hepatitis, zoonotic and intrauterine and other infection - infectious diseases. List of major diagnostic activities: Common blood test (6 parameters); General urine analysis; Urine analysis in Zimnitsky; Rebarga's test; Determination of residual nitrogen; Determination of creatinine, urea, intact hospital hormone, kSHS; Defining potassium / sodium. Calcium definition; Determination of chlorides; Magnesium definition; The level of syrontary ferritin and serum iron, the saturation coefficient of transferlic iron; Ultrasound of the abdominal organs; USDG vessels. List of additional diagnostic events: Determination of glucose, free iron, the number of hypochromic erythrocytes; Coagulogram 1 (prothrombin time, fibrinogen, thrombin time, APTTV, fibrinolytic plasma activity, hematocrit); Definition of Alt, Ast, Bilirubin, Timol Sample; IFA markers vg; Determination of common lipids, cholesterol and lipid fractions; CT scan; Consultation ophthalmologist. Differential diagnosis
Treatment abroad Treat treatment in Korea, Israel, Germany, USAGet advice on medical examination Treatment Treats of treatment: Diet, table number 7 (№7A or No. 7B - with pronounced CPN, No. 7G - in patients in hemodialysis). Reducing the consumption of protein to 0.6 g / kg / day., In the 5 stages, the protein consumption is increased to 1.2 g / kg / day. In hypercalemia (oliguraury, Anuria) - limitation of products containing potassium salts. Reducing phosphorus and magnesium consumption. The volume of the consumed fluid is 500 ml above the daily diurea. Restriction of the cook salt, with the exception of the soluble syndrome. Medicia treatment 1. Correction arterial hypertension
: 2. Correction of hyperphosphatemia and hyperparathyroidism: Gluconate or calcium carbonate, lanthana carbonate, Severmer hydrochloride, calcitriol. Further maintenance: Control of filtration, concentration functions of the kidneys, urine tests, blood pressure, kidney ultrasound, kidney nephrocintigraphy, vaccination against viral hepatitis B; List of basic medicines: 1. IAPF (Fozinopril) 2. Angiotensin II receptor blockers 3. * Atenolol 50 mg, Table., Dilatrend, Concorp 4. * Verapamil hydrochloride 40 mg, Table., Diltiaze 5. * Furosemid 20 mg / 2 ml, AMP. 6. * Beta Epoetin, 1000MA and 10 000 IU, Syringe Tubes 7. * Calcium gluconate 10 ml, AMP, Calcium carbonate, Lantana Carbonate, Selelamera Hydrochloride, Alfakalcidol, Rockaltrol, Calcitriol 8. * Iron-III preparations for intravenous administration, low molecular weight decar of iron, 2 ml / 100 mg, AMP. 9. Hemodialysis at SCF less than 15 ml / min. 10. * Iron sulfate monohydrate 325 mg, Table. 11. Amlodipine InformationList of developers Kanatubaeva A.B., Professor, KazNMU, Department of Children's Diseases of the Medical Faculty Kabulbaev K.A., Consultant, GKB №7, Department of nephrology and hemodialysis Attached filesAttention!Read also ...We recommend to read |