Viral conjunctivitis. How to recognize and treat acute conjunctivitis How to find conjunctivitis by ICD
1 Classification of pathology
A source:
H10 Conjunctivitis. H10.2 Other acute conjunctivitis. H10.3 Acute conjunctivitis, unspecified. H10.5 Blepharoconjunctivitis H10.8 Other conjunctivitis.
Local glucocorticoid drugs (0.1% dexamethasone solution, etc.) are an essential component in spring keratoconjunctivitis and corneal lesions. Given that long-term treatment with glucocorticoids may develop side effects, it is necessary to use lower concentrations of dexamethasone (0.01-0.05%), which are prepared ex tempore. Corneal regeneration stimulants (taurine, dexpanthenol 2 times a day) and lacrimal preparations (hypromellose + dextran 3-4 times a day, sodium hyaluronate 2 times a day) for corneal lesions.
ICD-10. H10 Conjunctivitis. H10 H10 .
Other acute conjunctivitis. H10 H10 .
Epidemiology
Prevention
- Exclusion of contact with causative allergens.
- Timely and adequate use of drugs for symptomatic and pathogenetic therapy.
- Carrying out medical and diagnostic activities using allergens only in specialized hospitals and offices under the supervision of an allergist-immunologist.
- ^ 1.01.1 Conjunctivitis
Links
With moderate severity of symptoms, erased clinical picture scraping from the edge of the eyelid to the demodex microorganism is mandatory. It sounds scary, but you shouldn't be afraid. A doctor or laboratory technician will tear out one or two cilia and examine them under a microscope. Of course, you shouldn't wash your face and put on makeup before the test. Demodex is a fairly common microorganism that has the ability to cause similar symptoms. If an infection is suspected, cultures of eye secretions for microflora may be required. Preparation of skin tests. Old enough, but, nevertheless, one of the most informative (if not the most informative) ways to find out what the allergy is. The optimal age of the patient is up to 50 years. Not for children under 3.5-4 years old. Antihistamines (Zyrtec, Diazolin, etc.) should not be taken before the examination. Contraindications for making skin tests: exacerbation of an allergic disease at the time of the study, pregnancy, breastfeeding, tuberculosis, the presence of cancer, skin diseases. Advantages of the method: very high diagnostic value, the result will be known in 30 minutes. Provocative tests. During the study, various solutions of allergens are instilled into the eyes and the reactions of the mucous membranes are assessed. If a local reaction occurs, the instilled solution contains a causally significant allergen. A rather dangerous method for the patient with a large number of complications. If a similar method is offered to you, then I recommend finding an excuse to refuse and think about changing the medical institution.
Treatment
Basic principles of therapy:
exclusion of the allergen, if possible; it is the most effective and safest method for the prevention and treatment of allergic conjunctivitis; symptomatic drug therapy (local, with the use of ophthalmic drugs, the general one involves the use of antihistamines by mouth for severe lesions) takes the main place in the treatment of allergic conjunctivitis; specific immunotherapy is carried out in hospitals, if drug therapy is not effective enough and it is impossible to exclude the "guilty" allergen.
Prevention
More details on the website
ICD-10 code
H10.0 Muco-purulent conjunctivitis. H10.1 Acute atopic conjunctivitis. H10.4 Chronic conjunctivitis.
Spring Qatar
Antiallergic drops: antazoline + tetrizoline or diphenhydramine + naphazoline or olopatadia 2-3 times a day no more than 7-10 days (combined drugs for acute allergic reaction); preparations of ketotifen, olopatadin or cromoglycic acid 2 times a day, if necessary, in long courses from 3-4 weeks to 2 months (after stopping an acute or subacute, chronic reaction). NSAIDs (indomethacin, diclofenac) 1-2 times a day. Ointments with glucocorticoids on the edges of the eyelids - prednisolone, hydrocortisone (in case of involvement of the eyelids and concomitant blepharitis). Systemic desensitizing treatment - loratadine: children over 12 years old, 10 mg once a day, children 2-12 years old, 5 mg once a day. With long courses, change the antihistamine once every 10 days.
More details
Chronic conjunctivitis. H10 ... Conjunctivitis, unspecified.
Elimination of contact with nonspecific irritants. Elimination of professional irritants.
Screening
Options
Etiology, pathogenesis
adenoviral conjunctivitis
Symptoms
When allergic conjunctivitis
When chronic conjunctivitis
Bacterial conjunctivitis
Allergic conjunctivitis
Literature
Material
Diagnostics
A specially conducted test is of great diagnostic value, in particular, the identification of eosinophils in scraping from the conjunctiva. Blood test for IgE-specific (specific immunoglobulins E). Allergic conjunctivitis is characterized by an increase in total IgE (total immunoglobulin E) in the blood test higher age norm (more than 100-150 IU). For this method there are no contraindications (can be done at any age, against the background of an exacerbation and taking medications). Cons: relatively high cost and rather high (up to 13-20%, depending on the manufacturer of the reagents) the frequency of false results.
a diet with limited carbohydrates and a high content of vitamins A, C, D and group B;
Portal editorial staff
A source:
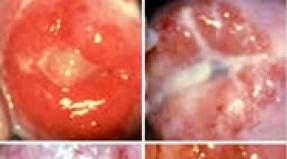
Conjunctivitis is one of the most common eye diseases. Today it is difficult to find a person who has never stumbled with the symptoms of this insidious disease. Treatment of conjunctivitis is complicated by the fact that viruses, fungi or bacteria can affect its development. So before prescribing treatment, you need to accurately determine the nature of the pathology.
Definition of disease
Acute conjunctivitis is an inflammatory process that affects the lining of the eye due to allergies or infections. The acute form of the disease is characterized by a pronounced symptomatology, which occurs suddenly, and with competent and timely treatment leaves quickly.
Given the cause of the development of the disease, conjunctivitis can be of the following types:

Taking into account which pathogen affects the development of conjunctivitis, the further therapy regimen is determined.
Causes of occurrence
Influence on the development of infectious conjunctivitis can be:

Among viral pathogens, the most common are:
- adenovirus infection,
- herpes virus,
- measles virus.
If we are talking about bacterial conjunctivitis, then its development is influenced by such agents:
- staphylococci,
- pneumococci,
- escherichia coli
- streptococci,
- diphtheria sticks,
- gonococci,
- koch's sticks.
Allergic conjunctivitis can occur when exposed to allergens such as medication, household chemicals, cosmetics. The pathological process can occur when physical and chemical factors affect the mucous membrane of the organ of vision, the presence of a chronic disease. 
Symptoms
Acute conjunctivitis can be recognized by the following symptoms:

It happens, so that when one eye is damaged, the infection spreads to the second, which makes the situation worse.
Possible complications
If you do not start the treatment of acute conjunctivitis, which has arisen against the background of chlamydia, then this is fraught with deformation of the eyelids and pathology of eyelash growth. If other bacteria have influenced the development of the disease, the following complications may occur:
- meningitis;
- sepsis;
- otitis.
Newborn babies may progress after conjunctivitis eye diseases... The result of adenovirus infection can be corneal opacity and damage to the tear film. The most frequent complication of the allergic form of conjunctivitis is its chronicity. After frequently recurring herpesvirus conjunctivitis, scars remain. The infectious form of the disease can lead to keratitis - inflammation of the cornea.
Diagnostics
Acute conjunctivitis can be diagnosed in several ways. An accurate and complete result can be obtained only after an external examination of the patient using a slit lamp. It is important to understand the history when making a diagnosis. The patient should carefully tell the doctor about the symptoms he is visiting.
Additional diagnostic methods include:
- sowing the conjunctiva;
- examinations of a smear or scraping;
- blood test, fluorography, organ x-ray chest (if there are concomitant symptoms). Sowing conjunctiva
Treatment Medicines
The doctor will be able to prescribe treatment only after an accurate diagnosis. It is from the cause of the development of pathology that the following therapy scheme can be determined:
- Bacterial conjunctivitis. For treatment, antibacterial drugs are used in the form of drops. Such drugs as Levomycetin, Sulfacil sodium remain effective. If mucus or pus is secreted from the eye, then it is necessary to use a solution of furacilin (1: 5000), potassium permanganate (1: 5000), 1% Oletetrin ointment for washing. The last drug it is necessary to lay on the eyelid 2-3 times a day.
- Viral conjunctivitis. For treatment, human leukocyte interferon or interferonogens are prescribed. These include Pirogenal, Poludan. Dripping drops into the conjunctival sac 6-8 times a day. You can use ointments: 0.5% Florenal, 0.05% Bonafton.
- Chlamydial conjunctivitis... Prescribe systemic administration of such drugs: Doxycycline, Tetracycline or Erythromycin.
- Fungal conjunctivitis. Local infusion of Nystatin, Levorin, Amphotericin B is used.
Tetracycline is used in the treatment of chlamydial conjunctivitis
- Allergic conjunctivitis. Prescribe drops with a vasoconstrictor and antihistamine effect, corticosteroids, tear substitutes, desensitizing drugs.
- Fungal conjunctivitis. For treatment, antimycotic ointments and drops are used - Levorin, Nystatin, Amphotericin B.
- Dry eye syndrome. This pathological process develops as a secondary lesion of the lacrimal apparatus. Artificial tear preparations - Oksial are used. Oxial is used to treat dry eye syndrome
Drops with conjunctivitis
When treating conjunctivitis, the doctor must prescribe eye drops to patients. The following medicines remain effective:
- The bacterial form is Floxal, Ciprofloxacin. To get the maximum result, it is necessary to lay Tetracycline ointment on the eyelids.
Floxal is used in the treatment of bacterial conjunctivitis
If you use these drugs according to the indicated scheme, then you can very quickly cure a mild form of conjunctivitis at home.
- Allergic form. Use drops with an antihistamine effect - Lekrolin, Opatanol. In addition, appoint hormonal ointments and drops - Hydrocortisone eye ointment, Dexamethasone.
- Viral form. Drops with antiviral effect are prescribed. They should contain interferon - Poludan, Oftalmoferon.
Poludanum is used in the treatment of viral conjunctivitis
Often, the infection can be of a mixed form, then the doctor prescribes a set of drops.
Folk remedies
In some cases, it is possible to treat conjunctivitis at home. In addition to basic therapy, your doctor may recommend using the following folk remedies:
- Aloe. Tear off fresh aloe leaves, wash, squeeze out the juice and moisten cotton pads in it. Apply to eyes for 15 minutes.
- Baking soda... Take 5 g of soda, 100 ml of water. Combine components and use eye wash solution.
- Barberry root. Take raw materials in an amount of 5 g (powder), pour 200 ml of water. Simmer on the fire for 15-30 minutes. Use a decoction for rinsing or compress. The barberry contains berberine and antibacterial compounds.
Dry your eyes thoroughly after each procedure and then rinse them. boiled water.
- Bread. Apply cold bread to your eyes. This will help reduce inflammation and itching.
- Castor oil... It is necessary to drip it, 1 drop into each eye. Do this every day.
- Chamomile. Take 10 g of raw materials, pour 200 boiling water. Insist 5 minutes, filter, cool and use for rinsing or compress. You can also take equal amounts of chamomile and eyebright. For 20 g of raw materials, a glass of boiling water. Apply rinsing solution.
- Goldenseal canadian. This plant effectively copes with infectious conjunctivitis, since it contains berberine. It is especially effective to use the agent in the treatment of streptococcal conjunctivitis. Take 20 g of raw materials, pour a glass of boiling water. Apply a filtered compress solution. You can also drip 2-3 drops into each eye daily.
- Eyebright medicinal. This plant is in great demand in the treatment of various eye diseases. It has an astringent and antibacterial effect, relieves eye irritation. You need to take 10 g of raw materials, pour 200 ml of boiling water. Filter, refrigerate and use for eye wash. Carry out the procedure 3-4 times a day.
- Rusty elm. Apply a compress using a rusty elm compress. It has bactericidal, astringent, analgesic and antioxidant effects. Apply the compress to the eyes for 15 minutes.
If swelling is present, the sachet can be moistened with cool water.
Prevention
IN the basis for the prevention of acute conjunctivitis is the observance of hygiene rules. It is important to wash your hands with soap, do not touch your face and eyes, do not use other people's cosmetics and personal hygiene products. But the prevention of allergic conjunctivitis involves the timely detection of the allergen. Next, you need to try to avoid contact with him.
Acute conjunctivitis is a disease characterized by unpleasant symptoms of a pronounced nature. To start dealing with a disease, you need to understand the nature of pathology. For the treatment of allergic, viral and bacterial conjunctivitis, completely different drugs are used.
Conjunctivitis ICD 10 is a disease that causes inflammation of the mucous membrane of the eye. Its signs can be redness, itching, irritation, pain when exposed to light rays, profuse unreasonable lacrimation, etc.
Like most diseases, conjunctivitis is included in the ICD 10 - the international medical classification of diseases. It is confirmed by the relevant document and is applied all over the world.
How to find conjunctivitis by ICD
In the international classification, conjunctivitis corresponds to the H10 code. Moreover, as you know, this disease has several varieties, which are also indicated in the ICD:
- H10.0 - purulent;
- H10.1 - atopic;
- H10.2 - all acute;
- H10.3 - acute, unspecified;
- H10.4 - chronic;
- H10.5 - blepharoconjunctivitis;
- Н10.8 - others;
- H10.9 - unspecified.
A number of conjunctivitis, not listed in this list, are indicated in international documentation using the H10-H13 coding, depending on the characteristics.
ICD classification allows physicians and pharmacists different countries determine the disease and methods of its treatment, which allows them to use the methods of treatment already proven in practice. And it is also used in the release of drugs for conjunctivitis for export by some countries, and by others in the purchase and use, knowing in which case they should be used.
Types and features of the disease
Like other diseases, conjunctivitis is expressed in two forms:
- acute;
- chronic.
The acute form occurs suddenly and is characterized by a sharp manifestation of symptoms, severe pain, cramps, redness and itching appear. Chronic, however, provides for repeated re-manifestation of the disease, and it is not as pronounced as in the first case. In this case, both eyes are inflamed, symptoms appear gradually.
Also, conjunctivitis is divided into the following types:
- The viral develops, as a rule, in parallel with other viral diseases, proceeds quickly and affects both eyes, profuse lacrimation and purulent discharge are characteristic, and may also be accompanied by damage to other otolaryngic organs.
- Bacterial is a consequence of damage by coccal bacteria, it is distinguished by purulent discharge of a grayish color, due to their thick consistency, the eyelids stick together, and also affects the skin around the eyes.
- Fungal is a consequence of exposure to the mucous membrane of fungi.
- Allergic caused by an allergenic irritant, may be accompanied by damage to the respiratory tract mucosa.
- Chemical appears as a result of mucosal lesions toxic substances, of the symptoms, only pain is present.
- Medicinal is a side effect of the use of certain medications, from the symptoms there is a burning sensation and lacrimation.
This classification is used to establish a treatment method that depends on the form and type of conjunctivitis.
Treatment of the disease
Treatment for each type of conjunctivitis has its own characteristics. When allergic or medicinal type it is necessary to limit contact with the allergen, which will lead to a weakening of the symptoms, and subsequently, complete elimination of them. If it is impossible to break contact, antihistamine blockers are used.
Important! Despite the fact that conjunctivitis code, which is H10 according to the ICD, is a common disease, in no case should you self-medicate. In case of occurrence of the corresponding symptoms, be sure to undergo a medical examination.
Viral species are treated with special drops, but besides this, do not forget that, as a rule, in this case, conjunctivitis has concomitant diseases, which should also be eliminated.
In the case of bacterial diseases, the doctor without fail prescribes antibiotics that affect the source of the problem, and ointments are used to relieve symptoms. Fluoroquinol preparations are also used.
Conjunctivitis encoding in ICD
Ophthalmologists consider conjunctivitis to be the most common eye disease. This is the name of the inflammatory processes of the mucous membrane of the eyes, which are encrypted for medical documentation under the code H10, implying conjunctivitis in the ICD 10 revision.
The etiology of this eye lesion is very diverse. Children, people with weakened immune systems and persons suffering from lingering chronic diseases... The nature of the inflammation can be infectious or non-infectious, and the course is acute or chronic.
In children, inflammatory processes of the eyes are usually observed against the background of a viral infection or the common cold, as well as in the case of pathological processes of the accessory organs (maxillary sinuses, ears).
In other cases, damage to the conjunctiva occurs due to the effects of such foreign agents:
pathogenic microorganisms (staphylococci, streptococci, pneumococci, mycobacteria); fungal infections; a variety of allergens (dust, fluff, chemicals, makeup, pollen) can provoke atopic or allergic conjunctivitis; viruses.
Varieties of inflammatory lesions of the organ of vision are determined by the pathogen, due to which the encoding in the ICD will differ.
The initial form of inflammation of the conjunctiva is very often confused with the manifestation of the usual symptoms of a cold or ARVI, but specific symptoms begin to appear soon enough and indicate targeted eye damage. All forms of this disease have almost the same characteristic features. An accurate diagnosis can only be made by a specialist in this matter, that is, an ophthalmologist. Questioning and examination of the patient is very important here.
Acute conjunctivitis manifests itself in the presence of such subjective complaints:
A source:
What is conjunctivitis and the ICD-10 disease code
1 Classification of pathology
Conjunctivitis is also listed in the ICD-10 system. This disease is numbered H10. However, conjunctivitis has many varieties. For example, if conjunctivitis differs in the secretion of mucus and pus, then the code will be H10.0. If the disease has an acute atopic form, then the code will be H10.1. Other acute forms of the disease are listed under the number H10.2. If conjunctivitis is acute, but unspecified, then its number is H10.3. In the chronic form of conjunctivitis, the number H10.4 is set. For blepharoconjunctivitis there is a code with numbering H10.5. For other forms of this disease, the code H10.8 is used. And if the disease could not be clarified, then the number H10.9 is written.
2 Forms of disease and characteristics
A source:
Allergic conjunctivitis mkb 10
Allergic conjunctivitis in children
Allergic conjunctivitis in children is an inflammatory reaction of the conjunctiva that occurs with an increased, genetically inherent sensitivity of the body to one or another allergen. The conjunctiva is the most frequent localization of an allergic reaction on the part of the organ of vision (up to 90% of all allergies). Allergic conjunctivitis is often combined with other allergic diseases (bronchial asthma, allergic rhinitis, atopic dermatitis).
ICD-10 code
H10 Conjunctivitis. H10.0 Muco-purulent conjunctivitis. H10.1 Acute atopic conjunctivitis. H10.2 Other acute conjunctivitis. H10.3 Acute conjunctivitis, unspecified. H10.4 Chronic conjunctivitis. H10.5 Blepharoconjunctivitis H10.8 Other conjunctivitis.
Pollinous (hay) conjunctivitis
Pollinous conjunctivitis is a seasonal allergic eye disease caused by pollen during the flowering period of grasses, cereals, and trees. Pollinosis belongs to the group of exoallergic diseases occurring in an immediate manner. Inflammation of the mucous membrane of the eyes can be combined with damage to the upper respiratory tract, skin, gastrointestinal tract, and various parts nervous system or other organs.
This conjunctivitis is characterized by an acute onset. Against the background of pronounced unbearable itching, there are edema of the skin and hyperemia of the edges of the eyelids, pronounced edema of the conjunctiva, up to the development of chemosis; a transparent, mucous, thick sticky discharge appears in the conjunctival cavity; on the conjunctiva of the upper eyelid, diffuse papillary hypertrophy is noted. In the cornea, marginal superficial infiltrates, prone to ulceration, may occur. Diffuse epitheliopathy is possible. Often, polynous allergosis proceeds as seasonal chronic conjunctivitis.
Spring Qatar
It occurs in children aged 5-12 years (more often in boys) and has a chronic, persistent course with exacerbations during the sunny season. Complaints of visual fatigue, feeling of a foreign body and severe itching... There are conjunctival, limbal and mixed forms of the disease.
Characterized by papillary growths on the conjunctiva of the cartilage of the upper eyelid, flattened, medium and large in the form of "cobblestone pavement". The conjunctiva is thickened, milky-pale, matte, with a sticky, viscous mucous discharge. The conjunctiva of other departments is not affected.
In the area of \u200b\u200bthe limbus, the growth of a gelatin-like roller of yellow or pink-gray color. Its surface is uneven, shiny with prominent white dots (Trantas spots), consisting of eosinophils and altered epithelial cells. During the period of regression, depressions are formed in the affected area of \u200b\u200bthe limb.
In the mixed form, simultaneous damage to the tarsal conjunctiva and the limbus zone is characteristic. The defeat of the cornea occurs against the background of severe changes in the conjunctiva of the upper eyelid: epitheliopathy, erosion, thyroid corneal ulcer, hyperkeratosis. Corneal pathology is accompanied by a decrease in vision.
Hyperpapillary (large papillary) conjunctivitis
The disease occurs with prolonged contact of the conjunctiva of the upper eyelid with a foreign body ( contact lenses, eye prostheses, sutures after cataract extraction or keratoplasty). Patients complain of itching and mucous discharge; in severe cases, ptosis occurs. On examination, giant (1 mm or more) papillae of the conjunctiva of the upper eyelid are revealed. The clinical picture is similar to the manifestations of the conjunctival form of spring catarrh, but there is no itching, sticky mucous discharge, lesions of the limbus and cornea. The main treatment is foreign body removal and local antiallergic therapy.
Medicinal conjunctivitis in a child
The disease can occur acutely (within the first hour after the use of any drug) and subacutely (within the first day after using the drug). Most often (in 90% of cases) drug conjunctivitis occurs with prolonged use of drugs (several days or weeks). An allergic reaction can develop both to the drug itself and to the preservative of the eye drops, most often with topical application antibacterial drugs and local anesthetics.
In acute allergic conjunctivitis, the appearance of a rapidly growing vitreous chemosis and conjunctival edema is characteristic, there is severe itching, burning, copious mucous (sometimes filmy) discharge from the conjunctival cavity. Some areas of the mucous membrane can be eroded. Papillary hypertrophy of the upper eyelid is noted, follicles appear in the conjunctiva of the lower transitional fold and lower eyelid.
Infectious-allergic conjunctivitis in children
The most common cause of inflammation among microbial allergens is staphylococcal exotoxins produced by saprophytic strains. The disease is referred to as delayed-type allergic reactions. Characterized by a chronic course, pronounced subjective symptoms and moderate objective data (conjunctival hyperemia, papillary hypertrophy of the eyelid conjunctiva). The causative agent in the conjunctiva is absent.
Tuberculosis-allergic phlyctenular keratoconjunctivitis (scrofulous keratoconjunctivitis, or scrofula). Characterized by the appearance in the conjunctiva and on the cornea of \u200b\u200bsingle or multiple nodules (flicken). They contain lymphocytes, macrophages, but the causative agent and caseous necrosis are absent from the inflammatory process - an allergic reaction to the decay products of mycobacteria circulating in the blood. As a rule, the nodules disappear without a trace, but sometimes they can ulcerate with subsequent scarring. The triad of subjective corneal symptoms (photophobia, lacrimation, blepharospasm) is pronounced; the patient with drip anesthesia cannot open his eyes. Convulsive constriction of the eyelids and constant watery eyes cause swelling and maceration of the skin of the eyelids and nose. The disease begins acutely, then takes a protracted course, characterized by frequent relapses.
Treatment of allergic conjunctivitis in children
The basis of treatment is the elimination of the allergen or the withdrawal of the drug that caused the allergic reaction.
Antiallergic drops: antazoline + tetrizoline or diphenhydramine + naphazoline or olopatadia 2-3 times a day no more than 7-10 days (combined drugs for an acute allergic reaction); preparations of ketotifen, olopatadin or cromoglycic acid 2 times a day, if necessary, in long courses from 3-4 weeks to 2 months (after stopping an acute or subacute, chronic reaction). NSAIDs (indomethacin, diclofenac) 1-2 times a day. Local glucocorticoid drugs (0.1% dexamethasone solution, etc.) are an essential component in spring keratoconjunctivitis and corneal lesions. Given that long-term treatment with glucocorticoids may develop side effects, it is necessary to use lower concentrations of dexamethasone (0.01-0.05%), which are prepared ex tempore. Ointments with glucocorticoids on the edges of the eyelids - prednisone, hydrocortisone (in case of eyelid involvement and concomitant blepharitis). Corneal regeneration stimulants (taurine, dexpanthenol 2 times a day) and lacrimal preparations (hypromellose + dextran 3-4 times a day, sodium hyaluronate 2 times a day) for corneal lesions. Systemic desensitizing treatment - loratadine: children over 12 years old, 10 mg once a day, children 2-12 years old, 5 mg once a day. With long courses, change the antihistamine once every 10 days.
The most effective method of treating severe allergic conjunctivitis in children is specific hyposensitization with pollen allergens, which is carried out outside the period of exacerbation of the disease.
More details
Allergic conjunctivitis is a disease characterized by inflammation of the conjunctiva of the eyes caused by a causal allergen and clinically manifested by lacrimation, sensation of a foreign body in the eyes, conjunctival hyperemia and itchy eyelids.
ICD-10. H10 Conjunctivitis. H10 ... Acute atopic conjunctivitis. H10 .
Other acute conjunctivitis. H10 ... Acute conjunctivitis, unspecified. H10 .
Chronic conjunctivitis. H10 ... Conjunctivitis, unspecified.
Epidemiology
Allergic conjunctivitis is one of the most common allergic diseases. In a large percentage of cases, a combination of allergic rhinitis and conjunctivitis (rhinoconjunctivitis) is noted. The onset of the disease more often occurs in childhood and adolescence, less often at an older age.
Prevention
These preventive measures reduce the frequency and severity of exacerbations of conjunctivitis, prevent the occurrence of other allergic diseases.
Elimination of contact with causative allergens. Elimination of contact with nonspecific irritants. Elimination of professional irritants. Timely and adequate use of drugs for symptomatic and pathogenetic therapy. Carrying out medical and diagnostic measures using allergens only in specialized hospitals and offices under the supervision of an allergist-immunologist.
Screening
Registration is required to proceed. shown 1 among 18
Material from the site
Conjunctivitis - inflammation of the mucous membrane of the eye (conjunctiva). caused, most often, by an allergic reaction or infection (viral, less often bacterial).
Distinguish between adenoviral (pharyngoconjunctival fever). enterovirus, herpetic, bacterial, chlamydial, allergic, acute and chronic conjunctivitis. In adults, 85% of cases of conjunctivitis are caused by adenoviruses and only 15% by bacteria; in children, bacterial and adenoviral conjunctivitis occur with the same frequency.
Options
Blepharoconjunctivitis - a combination of conjunctivitis with blepharitis (inflammation of the eyelids).
Keratoconjunctivitis - a combination of conjunctivitis with keratitis (inflammation of the cornea).
Episclerite - an inflammatory process that runs in the same way as conjunctivitis, but without discharge from the eyes and lacrimation.
Etiology, pathogenesis
adenoviral conjunctivitis - the virus is transmitted by airborne droplets. The disease occurs in the form of epidemic outbreaks mainly in children's groups (kindergartens, schools).
acute conjunctivitis - pathogens: Koch-Weeks bacillus, Morax-Axenfeld's stick, pneumococci, gonococci, streptococci, staphylococci. Basically, an exogenous infection of the conjunctiva occurs, autoinfection is possible.
Predisposing factors may be cooling or overheating of the body, general weakening, microtrauma of the conjunctiva, myopia, astigmatism, past infections. Koch-Weeks conjunctivitis (acute epidemic conjunctivitis) is transmitted through the patient's contaminated hands and infected objects, gives epidemic outbreaks and is observed mainly in the summer among children living in hot climates.
Conjunctivitis caused by gonococcus (blennorrheal conjunctivitis). occurs in newborns when the head passes through the birth canal of a mother suffering from gonorrhea. Unlike acute conjunctivitis, conjunctivitis caused by the Morax-Axenfeld bacillus is subacute or chronic course and predominant localization in the corners of the palpebral fissure.
chronic conjunctivitis - long-term irritation of the conjunctiva (dust, smoke, chemical impurities in the air). vitamin deficiency, metabolic disorders, chronic damage to the nose and lacrimal ducts, ametropia.
allergic conjunctivitis is an allergic inflammation of the conjunctiva of the eyes, which is manifested by redness of the eyes, swelling of the eyelids, itching, lacrimation, photophobia.
Symptoms
In general cases, edema of the eyelids, edema and hyperemia of the conjunctiva, photophobia, lacrimation, reddening of the white of the eye.
When allergic conjunctivitis patients, as a rule, experience severe itching of the eyes, sometimes pain in the eyes, often slight swelling of the eyelids. When going to chronic form only symptoms such as itching and eye irritation persist.
Viral conjunctivitis... most often associated with an upper respiratory tract infection (adenovirus or herpes). may appear with a common cold and / or sore throat. Symptoms: watery eyes and intermittent itching.
Usually, these conjunctivitis starts in one eye and then spreads to the other eye. When adenoviral conjunctivitis damage to the eyes is preceded and accompanied by damage to the upper respiratory tract, an increase in body temperature, an increase in the pre-aural lymph nodes (more often in children). Moderate blepharospasm, scant purulent discharge are noted. Often, the disease is accompanied by the appearance of follicles or films (more often in children).
Bacterial conjunctivitis... Caused by pyogenic (pus-producing) bacteria. The first symptom is a viscous, cloudy, gray or yellowish discharge from the eyes, which can cause the eyelids to stick together, especially after sleep.
However, discharge is not the main symptom of bacterial conjunctivitis. For example, bacteria such as Chlamidia trachomatis or Moraxella can cause non-exudative but persistent conjunctivitis without significant conjunctival hyperemia.
In some patients, bacterial conjunctivitis manifests itself only as a foreign body sensation in the eye. Another symptom that distinguishes bacterial conjunctivitis is dryness of the infected eye and surrounding skin. Acute pyogenic infections can cause pain.
Like viral conjunctivitis, bacterial, most often affect only one eye, but then can easily go to the other. Symptoms usually do not appear until the third day after infection.
Conjunctivitis caused by toxic and toxic substances... The main symptom is irritation and pain in the eye when looking up or down. Discharge and itching are usually absent.
This is the only group of conjunctivitis that can be accompanied by severe pain.
When acute conjunctivitis there is a feeling of pain in the eyes, mucopurulent or purulent discharge. For blennorrhea conjunctivitis, it is characterized at first by serous-bloody, and after 3-4 days, profuse purulent discharge.
Formation of infiltrates, corneal ulcers is possible. In case of Koch-Weeks conjunctivitis, multiple small hemorrhages in the conjunctiva of the sclera and its edema in the form of triangular elevations within the palpebral fissure. Morax-Axenfeld conjunctivitis is characterized by a subacute or chronic course and predominant localization in the corners of the palpebral fissure.
When chronic conjunctivitis itching, burning, feeling of "sand behind the eyelids", eye fatigue is noted.
According to recent studies, people with blue eyes, which are significantly more sensitive to light, are at greater risk of long-term visual damage from conjunctivitis.
Causes
Often conjunctivitis are viral in nature (usually adenoviral). other causes are bacteria, allergies, irritants and dry eye syndrome. Both viral and bacterial conjunctivitis are contagious. As a rule, conjunctivitis is transmitted from one person to another if personal hygiene is not followed.
Treatment
As a rule, conjunctivitis is contagious and, although the cause can be difficult to identify, all patients are advised to wash their hands thoroughly and follow other personal hygiene rules so as not to infect others. Adequate therapy is prescribed by an ophthalmologist.
Viral conjunctivitis... Warm compresses and artificial tear drops are used to relieve symptoms of viral conjunctivitis.
Specific antiviral drug for the treatment of viral conjunctivitis are eye drops containing recombinant interferon type alpha 2. When attaching a secondary bacterial infection drops containing antibiotics are prescribed. With conjunctivitis caused by the herpes virus (herpetic conjunctivitis). drugs containing acyclovir and ophthalmoferon drops are prescribed.
Bacterial conjunctivitis... Bacterial conjunctivitis does not always require treatment and may go away on its own. However, eye drops or ophthalmic ointments containing antibiotics can significantly speed up this process. Antibacterial agents (topically) are prescribed only for conjunctivitis with abundant purulent discharge and in the absence of characteristic symptoms of adenovirus infection (enlarged lymph nodes and the appearance of follicles on the conjunctiva).
Allergic conjunctivitis occur upon contact with an allergen in humans, with an increased sensitivity of the body to the allergen. For the treatment of allergic conjunctivitis, antihistamines are used in the form of eye drops and tablets.
These eye drops are effective for relieving itching, but can cause red eyes and swelling of the eyelids. Such drops, unlike antihistamine tablets, act faster and are less likely to cause dry eyes.
Side effects when using antihistamines: mild pain and burning eyes, headaches, insomnia. In addition, artificial tear drops help reduce discomfort. In difficult cases, nonsteroidal anti-inflammatory drugs are prescribed.
Some people with persistent allergic conjunctivitis are also prescribed steroid eye drops. In addition, for the treatment of conjunctivitis of an allergic nature, combined eye drops containing diphenhydramine, metacel (artificial tear) and interferon alfa 2 are prescribed.
With conjunctivitis, you should not touch your eyes with your hands, it is important for patients to follow the rules of personal hygiene, wash their hands thoroughly and use only their own towel so as not to infect other family members. Viral conjunctivitis usually resolves within 3 weeks. However, the treatment process can take more than a month.
Notes
^ 1.01.1 Conjunctivitis
Literature
a b Fisher, Bruce; Harvey, Richard P .; Champe, Pamela C. (2007). Lippincott's Illustrated Reviews: Microbiology (Lippincott's Illustrated Reviews Series). Hagerstown, MD: Lippincott Williams & Wilkins. ISBN 0-7817-8215-5.
Links
Material
MEDURFO. RU Allergic conjunctivitis
deterioration of vision; excruciating itching of the eyelids.
The conjunctiva or limbus, or both, are objectively changed, which makes it possible to distinguish between palpebral or tarsal, limbal or bulbar and mixed forms of catarrh.
The first form is characterized by slight ptosis (drooping of the eyelid). massive, flat, like a cobblestone pavement, polygonal, milky-pink or bluish-milky papillary growths on the conjunctiva of the upper eyelid cartilage, which last for years, but disappearing, do not leave a scar.
With limbal spring catarrh, dense vitreous, yellowish-gray or pink-gray growths of the conjunctiva along the upper limbus, sometimes waxy yellow nodes, are noted. The mixed form combines lesions of the conjunctiva of the superior cartilage and limbus. With all forms of discharge from the growths, there is little, it is viscous, stretches with threads, eosinophils are often found in smears and scrapings.
Most researchers in one way or another associate spring catarrh with ultraviolet radiation, hereditary predisposition, endocrine influences.
Diagnostics
A disease such as allergic conjunctivitis is in the sphere of interests of two medical specialties: an allergist-immunologist and an ophthalmologist (ophthalmologist). You should visit them first. You should start with an ophthalmologist, since a number of eye diseases are accompanied by symptoms similar to allergic conjunctivitis.
The ophthalmologist will certainly conduct an examination and make an anamnesis of the patient. In some cases, the typical picture of the disease or its clear connection with the effect of an external allergenic factor does not raise doubts about the diagnosis. In most cases, the diagnosis is fraught with great difficulties and requires the use of laboratory diagnostics.
A visit to an allergist will allow you to confirm the presence of an allergy and find the cause of the disease. To make the correct diagnosis, it is necessary to establish an allergic history - to find out about hereditary allergic burden, the characteristics of the course of diseases that can cause an allergic reaction, the frequency and seasonality of exacerbations, the presence of allergic reactions, in addition to eye reactions.
Doctors can refer a patient for research and tests:
With moderate severity of symptoms, erased clinical picture, scraping from the edge of the eyelid to the demodex microorganism is mandatory. It sounds scary, but you shouldn't be afraid. A doctor or laboratory technician will tear out one or two cilia and examine them under a microscope. Of course, you shouldn't wash your face and put on makeup before the test. Demodex is a fairly common microorganism that has the ability to cause similar symptoms. A specially conducted test is of great diagnostic value, in particular, the identification of eosinophils in scraping from the conjunctiva. If an infection is suspected, cultures of eye secretions for microflora may be required. Preparation of skin tests. Old enough, but, nevertheless, one of the most informative (if not the most informative) ways to find out what the allergy is. The optimal age of the patient is up to 50 years. Not for children under 3.5-4 years old. Antihistamines (Zyrtec, Diazolin, etc.) should not be taken before the examination. Contraindications for making skin tests: exacerbation of an allergic disease at the time of the study, pregnancy, breastfeeding, tuberculosis, the presence of cancer, skin diseases. Advantages of the method: very high diagnostic value, the result will be known in 30 minutes. Blood test for IgE-specific (specific immunoglobulins E). Allergic conjunctivitis is characterized by an increase in total IgE (total immunoglobulin E) in the blood test above the age norm (more than 100-150 IU). There are no contraindications for this method (it can be done at any age, against the background of an exacerbation and taking medications). Cons: relatively high cost and quite high (up to 13-20%, depending on the manufacturer of the reagents) the frequency of false results. Provocative tests. During the study, various solutions of allergens are instilled into the eyes and the reactions of the mucous membranes are assessed. If a local reaction occurs, the instilled solution contains a causally significant allergen. A rather dangerous method for the patient with a large number of complications. If a similar method is offered to you, then I recommend that you find an excuse to refuse and think about changing the medical institution.
Of the above methods of allergic examination, skin tests are the most preferred. If there are contraindications to them, then they choose a diagnosis by a blood test (blood for IgE to various allergens).
Treatment of allergic conjunctivitis is carried out only after the final confirmation of the diagnosis and confirmation of the allergic nature of conjunctivitis. Otherwise, the treatment will have no clinical effect and may contribute to the progression of inflammation and the development of complications.
Basic principles of therapy:
exclusion of the allergen, if possible; it is the most effective and safest method for the prevention and treatment of allergic conjunctivitis; a diet with limited carbohydrates and a high content of vitamins A, C, D and group B; symptomatic drug therapy (local, with the use of ophthalmic drugs, the general one involves the use of antihistamines by mouth for severe lesions) takes the main place in the treatment of allergic conjunctivitis; specific immunotherapy is carried out in hospitals, if drug therapy is not effective enough and it is impossible to exclude the "guilty" allergen.
Treatment of allergic conjunctivitis consists of a complex appointment of the following groups of drugs:
1. Antihistamines. Preference should be given to drugs of the second (claritin, kestin, cetrin, etc.) and third (erius, telfast, xizal, etc.) generations. The drugs are prescribed in an average age-specific dosage once a day.
The average duration of the course of treatment is 10-14 days. Some treatment regimens include long-term (several months) daily use of third-generation antihistamines due to their membrane-stabilizing effect.
Third-generation drugs certainly have a higher safety profile, but also more cost.
The use of tablets alone for the treatment of allergic conjunctivitis, as a rule, does not bring sufficient effect. In this regard, topical (local) therapy (treatment) is recommended.
2. Topical antihistamines. They are prescribed in the form of eye drops (allergodil, histimet, opatanol). The drug is instilled into the eyes two to four times a day. The duration of treatment is determined by the doctor.
3. Derivatives of cromoglycic acid. One of the most commonly used groups of drugs in the treatment of allergic conjunctivitis. Examples: eye drops cromohexal, hi-crom, opticrom. These drugs require long-term use.
The effect occurs no earlier than 10-14 days from the start of use.
They are issued in the form of eye drops and are prescribed 1-2 drops in each eye 3-4 times a day. They are considered one of the safest groups of drugs used in the treatment of allergic conjunctivitis. The disadvantages include the need frequent use (3-4 times a day). a long time from the start of treatment to the development of a therapeutic effect, moderate clinical efficacy.
4. Topical corticosteroid drugs. Prescribed for severe inflammatory process. Representatives of this pharmacological group medications: dexamethasone eye drops, hydrocortisone eye drops, hydrocortisone eye ointment.
The drugs are prescribed 1-3 times a day. The duration of the course of treatment is determined by the doctor.
When a causally significant allergen is identified and there are no contraindications, allergen-specific therapy is recommended (synonym: specific immunotherapy). This type of allergy treatment is carried out only by an allergist on the basis of an allergy office or an allergy hospital. Treatment consists in the introduction into the body of small doses of the allergen in gradually increasing concentrations.
As a result, the patient develops tolerance (addiction) to this allergen and the symptoms of the disease decrease or disappear completely. This is one of the most radical treatments for an allergic disease.
Prevention
Removal of the allergen that provokes exacerbation of allergic conjunctivitis from the patient's environment is an essential component of the treatment of allergic conjunctivitis. The list of allergens to be eliminated is identified after an allergic examination (for this, it is, by and large, necessary). If contact with the allergen is completely eliminated, then the symptoms of the disease will disappear without medication. Unfortunately, this does not always work.
The nature of elimination measures is determined by the type of allergen.
For example, if allergic conjunctivitis occurs as a result of an allergic reaction to a cat's fur, then the animal must be removed from the living quarters and then repeated wet spring cleaning should be carried out. Without thorough cleaning of the premises, animal allergens can remain in the apartment for up to six months. This is the most radical and effective option.
But there are times when you can't get rid of a cat. For example, a patient lives in a private house and the cat is the only factor holding back the mouse population.
Then the animal is not allowed into the bedroom of a person suffering from allergies, and special care products are used to reduce the concentration of animal allergens in the environment, and the animal is regularly washed (once a week) using special shampoos. Caring for a cat, of course, should be carried out by a person without allergies to it.
And in the patient's bedroom, you need to install an air purifier that should work around the clock. A very common cause of allergic conjunctivitis is allergy to household allergens and primarily to house dust and house dust mites (Dermatophagoides pteronyssinus and Dermatophagoides farinae). In this case, it is necessary to carry out a whole range of measures.
Pillows, blankets, mattresses should be made of artificial, hypoallergenic materials. If this is not possible, they are kept in special anti-allergic protective covers. Moreover, it is necessary to change all bedding.
A common mistake is that they change their pillow, and at the same time another family member is sleeping on a feather pillow next to him on the same bed.
It is necessary to regularly treat the apartment with anti-mite (acaricidal) drugs. The regularity of processing varies from once a month to 1 time in half a year and depends on the brand of the product you have chosen. The most popular acaricides today are Allergoff spray and ADS spray.
Wash bedding at 60 degrees. It also contributes to the death of ticks. All sources of house dust must be eliminated at home: carpets, heavy curtains, curtains, tapestries, large stuffed toys, etc.
Furniture should be made of materials that can be wiped down frequently. Use air purifiers in the apartment, while each room should have its own apparatus. You should not buy one cleaner for your entire apartment. It will be ineffective.
If you're on a budget, install a purifier in your bedroom first. Do a light damp mop daily. General cleaning at least once every 5-7 days.
Use vacuum cleaners with HEPA filters. Conventional vacuum cleaners with trash bags are ineffective for anti-allergic measures. They are not able to trap even the smallest dust particles, which cause allergies.
If cleaning is performed by a patient with allergic disease, which in principle is undesirable, then it must wear a mask and glasses tightly adjacent to the skin. After cleaning, rinse eyes with plenty of running water.
The TV, computer and other household appliances must be removed from the patient's bedroom, as a large amount of dust usually settles on them. Monitor the humidity in the apartment. The optimum moisture content is 40-50%. The increased humidity in the room (more than 75%) creates ideal conditions for the reproduction of house dust mites.
If this is not possible, it is necessary to minimize the time spent outside. It is better to leave the house after 11 am, when the pollen concentration is slightly lower. Outside, you should wear tight-fitting glasses.
After returning home, change your clothes, take a shower, rinse your eyes and nasal passages, rinse your mouth. Do not dry clothes after washing outside, there pollen settles on them. Open windows and vents must be closed with damp gauze, this will reduce the flow of the allergen into the room.
Use air purifiers. If you are using an air conditioner, it should also have an outlet air filter. Keep windows closed when driving around town.
Do not use phytopreparations, herbal cosmetics, bee products.
In any case, the nature of the activities carried out should be discussed with your treating allergist.
Portal editorial staff
More details on the website
The clinic of adenoviral conjunctivitis manifests itself 5-8 days after infection. At the beginning of the disease, there is an increase in body temperature with pronounced symptoms of pharyngitis and rhinitis, headache, dyspeptic disorders; submandibular lymphadenitis develops.
In the second wave of fever, signs of conjunctivitis appear first in the area of \u200b\u200bone eye, and after 2-3 days - in the other eye. Local symptoms in adenoviral conjunctivitis are characterized by edema and redness of the eyelids, abundant mucous or mucopurulent discharge, foreign body sensation, itching and burning, lacrimation, photophobia, moderate blepharospasm. Hyperemia is expressed in all parts of the conjunctiva, spreads to the lacrimal meatus, lunar and lower transitional fold.
The catarrhal form of adenoviral conjunctivitis proceeds with minor symptoms of local inflammation: slight redness of the mucous membrane of the eye, a moderate amount of discharge. The course of catarrhal adenoviral conjunctivitis is mild, the duration of the disease is about one week. There are usually no corneal complications.
The follicular form of adenoviral conjunctivitis is characterized by the presence of vesicular rashes (follicles) on the mucous membrane of the eye. Follicles can be small, punctate or large, translucent gelatinous; be located in the corners of the eyelids or cover all infiltrated and loosened mucosa, especially in the area of \u200b\u200bthe transitional fold. The follicular reaction looks like initial stage trachoma, however, diagnostic errors usually do not occur, since with trachoma there are no symptoms of nasopharyngitis, fever, and the rash is localized in the conjunctiva of the upper eyelid.
The membranous form of adenoviral conjunctivitis occurs in a quarter of cases. It proceeds with the formation of thin grayish-white films that cover the mucous membrane of the eye. Usually the films are delicate, easily removed with a cotton swab; but sometimes dense fibrinous overlays can form, adhered to the conjunctiva, which are difficult to remove from the inflamed mucosa. After removing the films, the exposed mucosa may bleed. Sometimes punctate subconjunctival hemorrhages and infiltrates are detected, which are completely absorbed after recovery. Scarring of the mucous membrane is often the outcome of filmy adenoviral conjunctivitis. With membranous adenoviral conjunctivitis, the general condition suffers: a high fever develops (up to 38 ° C-39 ° C), which can last from 3 to 10 days. The membranous form of adenoviral conjunctivitis can be mistaken for diphtheria.
Conjunctivitis is one of the most common eye diseases. Today it is difficult to find a person who has never stumbled upon the symptoms of this insidious disease. The treatment of conjunctivitis is complicated by the fact that viruses, fungi or bacteria can affect its development. So before prescribing treatment, you need to accurately determine the nature of the pathology.
Definition of disease
Acute conjunctivitis is an inflammatory process that affects the lining of the eye due to allergies or infections. The acute form of the disease is characterized by pronounced symptoms, which arise suddenly, and with proper and timely treatment, it quickly goes away.
Views
Given the cause of the development of the disease, conjunctivitis can be of the following types:

Taking into account which pathogen affects the development of conjunctivitis, the further therapy regimen is determined.
Causes of occurrence
Influence on the development of infectious conjunctivitis can be:

Among viral pathogens, the most common are:

If we are talking about bacterial conjunctivitis, then its development is influenced by such agents:
- staphylococci,
- pneumococci,
- escherichia coli
- streptococci,
- diphtheria sticks,
- gonococci,
- koch's sticks.
Allergic conjunctivitis can occur when exposed to allergens such as medicines, household chemicals, and cosmetics. The pathological process can occur when physical and chemical factors affect the mucous membrane of the organ of vision, the presence of a chronic disease. 
Symptoms
Acute conjunctivitis can be recognized by the following symptoms:

It happens, so that when one eye is damaged, the infection spreads to the second, which makes the situation worse.
Possible complications
If you do not start the treatment of acute conjunctivitis, which has arisen against the background of chlamydia, then this is fraught with deformation of the eyelids and pathology of eyelash growth. If other bacteria have influenced the development of the disease, the following complications may occur:
- meningitis;
- sepsis;
- otitis.
In newborn babies, eye diseases may progress after conjunctivitis. The result of adenovirus infection can also be a violation of the tear film. The most frequent complication of the allergic form of conjunctivitis is its chronicity. After frequently recurring herpesvirus conjunctivitis, scars remain. The infectious form of the disease can lead to. 
Diagnostics
Acute conjunctivitis can be diagnosed in several ways. An accurate and complete result can be obtained only after an external examination of the patient using a slit lamp. It is important to understand the history when making a diagnosis. The patient should carefully tell the doctor about the symptoms he is visiting.
Additional diagnostic methods include:

Treatment
Medicines
The doctor will be able to prescribe treatment only after an accurate diagnosis. It is from the cause of the development of pathology that the following therapy scheme can be determined:
- Bacterial conjunctivitis. For treatment, antibacterial drugs are used in the form of drops. Such drugs as Levomycetin, Sulfacil sodium remain effective. If mucus or pus is secreted from the eye, then it is necessary to use a solution of furacilin (1: 5000), potassium permanganate (1: 5000), 1% Oletetrin ointment for washing. The last drug should be placed on the eyelid 2-3 times a day.
- Viral conjunctivitis. For treatment, human leukocyte interferon or interferonogens are prescribed. This should include Pirogenal, Poludan. Dripping drops into the conjunctival sac 6-8 times a day. You can use ointments: 0.5% Florenal, 0.05% Bonafton.
- Chlamydial conjunctivitis. Prescribe a systemic intake of such drugs: Doxycycline, or.
- Fungal conjunctivitis. Local infusion of Nystatin, Levorin, Amphotericin B is used.

Tetracycline is used in the treatment of chlamydial conjunctivitis

Drops with conjunctivitis
When treating conjunctivitis, the doctor must prescribe eye drops to patients. The following medicines remain effective:
- The bacterial form is,. To get the maximum result, it is necessary to lay Tetracycline ointment on the eyelids.

Floxal is used in the treatment of bacterial conjunctivitis
If you use these drugs according to the indicated scheme, then you can very quickly cure a mild form of conjunctivitis at home.
- Allergic form. Use drops with an antihistamine effect - Lekrolin, Opatanol. In addition, hormonal ointments and drops are prescribed - Hydrocortisone eye ointment, Dexamethasone.
- Viral form. Drops with antiviral effect are prescribed. They should contain interferon - Poludan, Oftalmoferon.

Poludanum is used in the treatment of viral conjunctivitis
Often, the infection can be of a mixed form, then the doctor prescribes a set of drops.
Folk remedies
In some cases, perhaps. In addition to basic therapy, your doctor may advise you to use the following folk remedies:

After each procedure, the eyes should be thoroughly dried and then rinsed with boiled water.

If swelling is present, the sachet can be moistened with cool water.
Prevention
The prevention of acute conjunctivitis is based on hygiene. It is important to wash your hands with soap, do not touch your face and eyes, do not use other people's cosmetics and personal hygiene products. But the prevention of allergic conjunctivitis involves the timely detection of the allergen. Next, you need to try to avoid contact with him.
Video
conclusions
Acute conjunctivitis is a disease that is characterized by. To start dealing with a disease, you need to understand the nature of pathology. For the treatment of allergic, viral and bacterial conjunctivitis, completely different drugs are used.
Viral infection is common for human body process. Every day, millions of viruses attack it in an attempt to break through protective barriers and find a suitable habitat. In most cases, immune cells do their job successfully. However, people get sick, and most often these are lesions of the mucous membranes - the oral cavity, nose and nasopharynx, as well as the conjunctiva (mucous membrane of the eyes).
Definition of disease
For the adult population, a viral lesion of the eyes in 80% of cases means an adenovirus infection, and if later pus appears in the eyes, this means that bacteria have joined the disease through the patient's own fault.
IN childhood viral and bacterial lesions occur with approximately the same frequency, however, adenovirus predominates among viruses.
Most often, outbreaks of adenovirus infection occur in children's groups, where they spread very quickly in the spring-autumn period. This is due to a temporary decrease in immunity due to adaptation to climatic conditions. However, there are also sporadic (accidental) spread of infection, again in children's groups.
In the adult population, infection most often affects the elderly and, as a rule, is single.
Types and classifications
Depending on the strength of the symptoms, as well as their nature, the following forms of the disease are distinguished:
- Catarrhal. Most often, the disease takes exactly the catarrhal form, which is the easiest to cure and can last within 7 days. The healing period depends on the patient's age, as well as the state of his immunity. It is characterized by minimal symptoms: minor mucous discharge, slight swelling of the eyelids and redness of the eyes;
- Filmy. A characteristic feature is the formation of a gray-white film on the eye, which can be easily removed with a cotton swab. If there is no adequate treatment, then a scar may form on the mucous membrane. This form can last up to 12 days and be accompanied by general weakness and high t;

- Follicular. This form is characterized by the most severe symptoms and serious complications. The surface of the mucous membrane is covered with follicles (vesicles) of various sizes, which, without adequate treatment, cause scarring of the cornea.
The course of adenoviral conjunctivitis can be acute (pronounced symptoms and rapid progression) and subacute (moderate rate of development of the disease with symptoms of moderate severity).
Causes of occurrence
The main reason for the development of the disease is viral infection, which can proceed in 2 ways:
- Airborne. When a patient is nearby sneezing or coughing, the virus with droplets of sputum enters the mucous membrane of a healthy person, where it is successfully introduced. The source of infection can be healthy person - Carriage of viruses sometimes persists up to 4 weeks from the beginning of infection;
- Fecal-oral. This method of infection is typical for young children aged 0.5 to 5 years. Up to 6 months the baby is protected by transplacental immunity. Children on breastfeedingare also protected by antibodies derived from mother's milk.


Factors provoking the introduction of adenovirus include:
- Violation of personal hygiene;
- Hypothermia;
- Swimming in dirty water (pools or ponds);
- Failure to follow the rules of care or wearing contact lenses;
- Stress;
- ARVI;

Corneal surgery
Any condition that requires the immune system to work harder can weaken it and open the door for infection.
Symptoms
Adenovirus infection, penetrating the body, affects not only the mucous membrane of the eye. First of all, general symptoms appear: rhinitis and pharyngitis, dyspeptic disorders, increased t and headache, enlargement of the submandibular lymph nodes.
Later, signs of conjunctivitis appear: redness and swelling of the eyelids, sensation of a foreign body, burning and itching, photophobia and lacrimation, mucous (sometimes mixed) discharge, moderate. 
Symptoms may vary depending on the form of the disease:
- Catarrhal. Symptoms are mild and do not last more than a week;
- Follicular. A characteristic feature is numerous follicles on the mucous membrane, which can be point, large or small, localized in the corners of the eyelids or cover the entire mucosa
- Filmy. This form accounts for up to 25% of all cases of the disease. Greyish white films are usually easy to remove. However, sometimes they take the form of dense fibrinous overlays, which are fused to the conjunctiva and are difficult to remove. As a result of their removal, the mucous membrane may begin to bleed. Therefore, with this form of infection, scars are often formed on the surface of the mucous membrane.

When diagnosing, differentiation of the filmy form with diphtheria is carried out, and the follicular form with trachoma.
Possible complications
If the infection proceeds in a catarrhal form, and the treatment is carried out on time, then the risk of complications is minimal. With the development of more severe types of the disease, complications are possible:
- Toxic-allergic or. Attachment of bacterial infection or signs of allergic inflammation can develop as a result of a decrease in immunity or an increased susceptibility of the mucous membrane to toxins secreted by microorganisms;
- ... The defeat of the conjunctiva leads to a decrease in the production of tear fluid and the development of uncomfortable sensations: dryness and burning, increased eye fatigue, lacrimation and photophobia;

Dry eye syndrome
- ... Inflammatory lesions of the cornea, often leading to the formation of scars and ulcers, which invariably leads to a decrease in visual acuity;
- Otitis media, adenoiditis, tonsillitis. Inflammation of the middle ear, tonsils, as well as proliferation of lymphoid tissue in the nasopharynx can result from viral damage to the mucous membrane of the respiratory tract and the Eustachian tube.
A viral infection without adequate treatment can lead to serious changes in the transparency of the cornea and cause partial or complete loss of vision.
Diagnostics
When carrying out a diagnosis, the doctor finds out the duration and strength of the symptoms, as well as their nature. Moreover, not only signs of eye disease are important, but also a deterioration in the general condition of the body. The history data also includes information about the patient's suspected contact with people infected with adenovirus.
Particular attention is paid to bacteriological research:
- Conjunctival swab;
- Bacteriological culture;
- Cytological scraping.

Diagnostics of the adenoviral conjunctivitis
Such analyzes make it possible to differentiate with bacterial lesions. A mandatory item is a slit lamp examination, which allows you to assess the degree of damage to the eye tissues. To identify a viral infection, the most informative technique is PCR (polymerase chain reaction).
Treatment
Treatment is carried out mainly on an outpatient basis and does not present any particular difficulties when it comes to mild forms of the disease. With the development of complications of follicular or membranous conjunctivitis, hospitalization is possible.
Drug therapy
Conservative methods of treatment are the main ones when choosing therapeutic tactics. The choice of the necessary medicines is strictly individual under the supervision of a physician. Drugs from the following groups can be used:
- Antiviral: Interferon, Laferon;

Drops for eyes "Interferon"
- Antibacterial:,. Necessary when joining a bacterial infection or for its prevention - as prescribed by a doctor;
- Antibacterial ointments:, Levomycetinova. They are laid at night once a day to prevent secondary infection;
- Glucocorticosteroids:, Hydrocortisone, Dexamethasone. They are used to reduce the manifestations of inflammation: swelling, redness. They are used in extreme cases, since they suppress the immune system.
Treatment of adenoviral conjunctivitis should be timely and competent, and also take place only under the supervision of a doctor. Otherwise, the infection can spread to surrounding tissue and cause decreased vision.
Folk remedies
A viral infection in most cases with a good level of immunity is successfully suppressed by the forces of the organism itself. Typically, treatment does not require the use of potent drugs. Therefore, application folk remedies in some cases, it can be an effective adjunct to medications: 
- Grind burdock roots, pour boiling water over 3 tbsp. l. raw materials until fully covered, insist and rinse the eyes with filtered infusion;
- Blue cornflower flowers (1 tbsp. L.) Pour 250 ml of boiling water, boil for 10 minutes. over low heat and insist until it cools down almost completely. Use as a solution for washes and lotions. Additionally, introduce fish oil and liver into the diet;
- Dilute agave juice with boiled water (1: 10) and instill 2 drops in the eyes several times during the day;
- Make an infusion of chamomile or calendula flowers (1 tablespoon per 200 ml of water), strain and rinse your eyes;
- As antiviral agent use eucalyptus aromatic oil or chop the garlic into a saucer and place in the room;
- Use sour milk for washing, it perfectly removes inflammation of the mucous membrane.
When using even folk remedies, an ophthalmologist's consultation will not be superfluous. However, in the absence of such an opportunity, try to carefully observe all dosages and storage conditions of drugs, and even better - cook fresh ones daily.
Prevention
Measures to prevent adenoviral conjunctivitis are no different from the prevention of all viral infections:
- Strict adherence to the rules of personal hygiene;
- Timely isolation of an infected patient, especially in a children's team;
- Elimination of chronic foci of infection and treatment of viral diseases;
- Constant care of high level immunity: a balanced diet, the use of vitamins (natural and synthetic), hardening, playing sports or gymnastics, walking in the fresh air;
- Wet cleaning and airing.
In fact, the body is able to cope with viruses on its own, even if it has not encountered them before. However, for this he must have strong immunity, the presence of which is a guarantee of protection against viruses.
Video
conclusions
As a rule, adenoviral conjunctivitis develops after a runny nose and pharyngitis. Therefore, with the right actions at the very beginning, infection can be completely avoided.
However, if this does happen, do not let the illness take its course and pay a visit to your doctor, even if you are not going to take strong medications. After all, the virus can have a completely different nature and serious complications in the case of inadequate therapy.
The main obstacle to infection can be the immune system... Strengthen it in every way, and not only with pharmacy vitamins. After all, natural food gives the body not only vitamin components and essential trace elements, but also supplies tissues with building materials to create new cells to replace the dead. That is why give preference to natural fish and meat over ready-made sausages or canned food. This will help to avoid slagging of the body and this will also strengthen the immune system.
Conjunctivitis ICD 10 is a disease that causes inflammation of the mucous membrane of the eye. Its signs can be redness, itching, irritation, pain when exposed to light rays, profuse unreasonable lacrimation, etc.
Like most diseases, conjunctivitis is included in the ICD 10 - the international medical classification of diseases. It is confirmed by the relevant document and is applied all over the world.
How to find conjunctivitis by ICD
In the international classification, conjunctivitis corresponds to the H10 code. Moreover, as you know, this disease has several varieties, which are also indicated in the ICD:
- H10.0 - purulent;
- H10.1 -;
- H10.2 - all acute;
- H10.3 - acute, unspecified;
- H10.4 - chronic;
- H10.5 -;
- Н10.8 - others;
- H10.9 - unspecified.
A number of conjunctivitis, not listed in this list, are indicated in international documentation using the H10-H13 coding, depending on the characteristics.
The ICD classification allows doctors and pharmacists from different countries to determine the disease and methods of its treatment, which allows them to use methods of treatment that have already been tested in practice. And it is also used for export by some countries, and by others for purchase and use, knowing in which case they should be applied.
Types and features of the disease
Like other diseases, conjunctivitis is expressed in two forms:
- acute;
The acute form occurs suddenly and is characterized by a sharp manifestation of symptoms, severe pain, cramps, redness and itching appear. Chronic, however, provides for repeated re-manifestation of the disease, and it is not as pronounced as in the first case. In this case, both eyes are inflamed, symptoms appear gradually.

Also, conjunctivitis is divided into the following types:
- The viral develops, as a rule, in parallel with other viral diseases, proceeds quickly and affects both eyes, profuse lacrimation and purulent discharge are characteristic, and may also be accompanied by damage to other otolaryngic organs.
- Bacterial is a consequence of damage by coccal bacteria, it is distinguished by purulent discharge of a grayish color, due to their thick consistency, the eyelids stick together, and also affects the skin around the eyes.
- Fungal is a consequence of exposure to the mucous membrane of fungi.
- Allergic caused by an allergenic irritant, may be accompanied by damage to the respiratory tract mucosa.
- Chemical appears as a result of damage to the mucous membrane by toxic substances, of the symptoms, only pain is present.
- Medicinal is a side effect of the use of certain medications, from the symptoms there is a burning sensation and lacrimation.
This classification is used when setting a treatment method, which depends on the form and.
Treatment of the disease
Treatment for each type of conjunctivitis has its own characteristics. With the manifestation of an allergic or drug type, it is necessary to limit contact with the allergen, which will lead to a weakening of symptoms, and subsequently to complete elimination of them. In case it is impossible to break contact, antihistamine blockers are used.
Important! Despite the fact that conjunctivitis code, which is H10 according to the ICD, is a common disease, in no case should you self-medicate. In case of occurrence of the corresponding symptoms, be sure to undergo a medical examination.
Viral species are treated with special drops, but besides this, do not forget that, as a rule, in this case, conjunctivitis has concomitant diseases, which should also be eliminated.
In the case of bacterial diseases, the doctor without fail prescribes that affect the source of the problem, and ointments are used to relieve symptoms. Fluoroquinol preparations are also used.