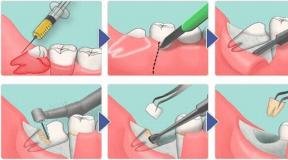
Diabetes insipidus is treated. Diabetes insipidus - what is it? The main characteristics of the disease How diabetes insipidus manifests itself
Diabetes insipidus - a disease caused by an absolute or relative deficiency of the hypothalamic hormone vasopressin (ADH-antidiuretic hormone).
The frequency of the disease is not known, it occurs in 0.5-0.7% of endocrine patients.
Regulation of vasopressin release and its effects
Vasopressin and oxytocin are synthesized in the supraoptic and paraventicular nuclei of the hypothalamus, packed into granules with the corresponding neurophysins and transported along axons to the posterior lobe of the pituitary gland (neurohypophysis), where they are stored until their release. The reserves of vasopressin in the neurohypophysis during chronic stimulation of its secretion, for example, with prolonged abstinence from drinking, are sharply reduced.
The secretion of vasopressin is caused by many factors. The most important of these is osmotic blood pressure, i.e. osmolality (or otherwise osmolarity) of plasma. In the anterior hypothalamus, near, but separately from the supraoptic and paraventicular nuclei, is located osmoreceptor ... When plasma osmolality is at a certain normal minimum, or threshold, the concentration of vasopressin in it is very low. If the plasma osmolality exceeds this setting threshold, the osmocenter perceives this, and the vasopressin concentration rises sharply. The osmoregulation system reacts very sensitively and very accurately. Some increase osmoreceptor sensitivity is associated with age.
The osmoreceptor is unequally sensitive to various plasma substances. Sodium(Na +) and its anions are the most potent stimulants of the osmoreceptor and vasopressin secretion. Na and its anions normally determine 95% of plasma osmolality.
Very effective in stimulating the secretion of vasopressin through the osmoreceptor sucrose and mannitol... Glucose practically does not stimulate the osmoreceptor, as well as urea.
The most reliable evaluative factor in the stimulation of vasopressin secretion is the determinationNa + and plasma osmolality.
The secretion of vasopressin is influenced by blood volume and blood pressure... These influences are carried out through baroreceptors located in the atria and the aortic arch. Stimuli from the baroreceptor along afferent fibers go to the brain stem as part of the vagus and glossopharyngeal nerves. From the brain stem, signals are transmitted to the neurohypophysis. A decrease in blood pressure, or a decrease in blood volume (eg, blood loss), significantly stimulates the secretion of vasopressin. But this system is much less sensitive than osmotic stimuli to the osmoreceptor.
One of the most effective factors that stimulate the release of vasopressin is nausea, spontaneous, or caused by procedures (vomiting, alcohol, nicotine, apomorphine). Even with the coming nausea, without vomiting, the level of vasopressin in plasma rises 100-1000 times!
Less effective than nausea, but an equally persistent stimulus for vasopressin secretion is hypoglycemia, especially sharp. A decrease in glucose levels by 50% of the initial in the blood increases the content of vasopressin by 2-4 times in humans, and in rats by 10 times!
Increases the secretion of vasopressin renin-angiotensin system... The level of renin and / or angiotensin required to stimulate vasopressin is not yet known.
It is also believed that nonspecific stress caused by factors such as pain, emotions, exercise stress, enhances the secretion of vasopressin. However, it remains unknown how stress stimulates the secretion of vasopressin - in any special way, or through a decrease in blood pressure and nausea.
Inhibit the secretion of vasopressin vasoactive substances such as norepinephrine, haloperidol, glucocorticoids, opiates, morphine. But it is not yet clear whether all these substances act centrally, or by increasing blood pressure and volume.
Once in the systemic circulation, vasopressin is rapidly distributed throughout the extracellular fluid. Equilibrium between the intra- and extravascular space is achieved within 10-15 minutes. Vasopressin is inactivated mainly in the liver and kidneys. A small part is not destroyed and is excreted in the urine intact.
Effects. The most important biological effect of vasopressin is water retention in the body by reducing urine output. The point of application of its action is the epithelium of the distal and / or collecting tubules of the kidneys. In the absence of vasopressin, the cell membranes lining this part of the nephron form an insurmountable obstacle to the diffusion of water and soluble substances. Under such conditions, the hypotonic filtrate formed in the more proximal parts of the nephron passes unchanged through the distal tubule and collecting ducts. The specific gravity (relative density) of such urine is low.
Vasopressin increases the permeability of the distal and collecting tubules to water. Since water is reabsorbed without osmotic substances, the concentration of osmotic substances in it increases, and its volume, i.e. quantity decreases.
There is evidence that a local tissue hormone, prostaglandin E, inhibits the action of vasopressin in the kidneys. In turn, non-steroidal anti-inflammatory drugs (for example, Indomethacin), which inhibit the synthesis of prostaglandins in the kidneys, increase the effect of vasopressin.
Vasopressin also acts on various extrarenal systems such as blood vessels, gastrointestinal tract, central nervous system.
Thirst serves as an irreplaceable addition to the antidiuretic activity of vasopressin ... Thirst is the conscious sensation of the need for water. Thirst is stimulated by many factors that cause the secretion of vasopressin. The most effective of these is hypertensive environment. The absolute level of plasma osmolality, at which the feeling of thirst appears, is 295 mosmol / kg. With this osmolality of blood, urine is normally excreted with a maximum concentration. Thirst is a kind of brake, the main function of which is to prevent a degree of dehydration that exceeds the compensatory capacity of the antidiuretic system.
The feeling of thirst rapidly increases in direct proportion to the plasma osmolality and becomes unbearable when the osmolality is only 10-15 mosmol / kg above the threshold level. Water consumption is proportional to the feeling of thirst. A decrease in blood volume or blood pressure also makes you thirsty.
Etiology
The development of central forms is not based on diabetes mellitus lies the defeat of various parts of the hypothalamus or the posterior lobe of the pituitary gland, i.e. neurohypophysis. The reasons may include the following factors:
infections acute or chronic: influenza, meningoencephalitis, scarlet fever, whooping cough, typhus, sepsis, tonsillitis, tuberculosis, syphilis, rheumatism, brucellosis, malaria;
traumatic brain injury : accidental or surgical; defeat electric shock; birth trauma during childbirth;
mental trauma ;
pregnancy;
hypothermia ;
tumor of the hypothalamus or pituitary gland : metastatic, or primary. Metastasizes to the pituitary gland more often breast cancer and thyroid glands, bronchi. Infiltration with tumor elements in lymphogranulomatosis, lymphosarcoma, leukemia, generalized xanthomatosis (Hend-Schüller-Crispen disease). Primary tumors: adenoma, glioma, teratoma, craniopharyngioma (especially common), sarcoidosis;
endocrine diseases : Syndromes of Simmonds, Sheehn, Lawrence-Moon-Biedl, pituitary dwarfism, acromegaly, gigantism, adinosogenital dystrophy;
idiopathic: in 60-70% of patients, the cause of the disease remains unclear. Among idiopathic forms, hereditary diabetes mellitus, traced in several generations, has a noticeable representation. The type of inheritance is autosomal dominant and recessive;
autoimmune : destruction of the nuclei of the hypothalamus as a result of an autoimmune process. This form is thought to occur among idiopathic diabetes insipidus, in which autoantibodies to vasopressin-secreting cells appear.
With peripheral In diabetes insipidus, the production of vasopressin is preserved, but the sensitivity of the receptors of the renal tubules to the hormone is reduced or absent, or the hormone is intensively destroyed in the liver, kidneys, placenta.
Nephrogenic diabetes insipidus more often observed in children, and is caused by anatomical inferiority of the renal tubules (congenital deformities, cystic-degenerative processes), or damage to the nephron (amyloidosis, sarcoidosis, lithium poisoning, methoxyfluramine). or a decrease in the sensitivity of the receptors of the epithelium of the renal tubules to vasopressin.
Clinic for diabetes insipidus
Complaints
thirsty from moderately expressed to painful, does not let go of patients either day or night. Sometimes patients drink 20-40 liters of water per day. In this case, there is a desire to take ice water;
polyuria and increased urination. The urine is excreted light, without urochromes;
physical and mentalweakness;
decreased appetiteslimming; development is possible obesity if diabetes insipidus develops as one of the symptoms of primary hypothalamic disorders.
dyspeptic disorders from the stomach - a feeling of fullness, belching, epigastric pain; intestines - constipation; gallbladder - heaviness, pain in the right hypochondrium;
mental and emotional disorders: headaches, emotional imbalance, insomnia, decreased mental activity, irritability, tearfulness; sometimes psychoses develop.
violation of menstruation, in men - potency.
Anamnesis
The onset of the disease can be acute, sudden; less often - gradual, and the symptoms increase as the disease worsens. Craniocerebral or mental injuries, infections, and surgical interventions on the brain can be the cause. Most often, the cause cannot be identified. Sometimes a burdened heredity for diabetes insipidus is established.
Flow chronic disease.
Inspection
emotional lability;
dry skin, reduced salivation and sweating;
body weight can be reduced, normal or increased;
the tongue is often dry due to thirst, the borders of the stomach are lowered due to constant fluid overload. With the development of gastritis or dyskinesia of the biliary tract, increased sensitivity and soreness on palpation of the epigastrium and right hypochondrium is possible;
cardiovascular and respiratory systems, the liver is usually not affected;
urinary system: frequent urination, polyuria, nocturia;
signsdehydration organism, if the fluid lost with urine is not replenished for some reason - lack of water, testing with "dry eating", or the sensitivity of the center of "thirst" decreases:
severe general weakness, headaches, nausea, repeated vomiting, aggravating dehydration;
hyperthermia, convulsions, psychomotor agitation;
cardiovascular system disorder: tachycardia, hypotension up to collapse and coma;
blood clotting: an increase in the number of Hb, erythrocytes, Na + (N136-145 mmol / l, or meq / l) creatinine (N60-132 μmol / l, or 0.7-1.5 mg%);
the specific gravity of urine is low - 1000-1010, polyuria persists.
These phenomena of hyperosmolar dehydration are especially characteristic of congenital nephrogenic diabetes insipidus in children.
The diagnosis is made based on the classic signs of diabetes insipidus and laboratory and instrumental studies:
polydipsia, polyuria
low specific gravity of urine - 1000-1005
plasma hyperosmolarity,> 290 mosm / kg (N280-296 mosm / kg water, or mmol / kg water);
hypoosmolarity of urine,< 100-200 мосм/кг;
hypernatremia,> 155 meq / l (N136-145 meq / l, mmol / l).
If necessary, carried out samples :
Dry food test. This test is carried out in a hospital, its duration is usually 6-8 hours, with good tolerance - 14 hours. No liquid is given. The food should be protein. Urine is collected every hour, and the volume and specific gravity of each hourly portion are measured. Measure the body weight after each 1 liter of urine excreted.
Grade: the absence of significant dynamics of the specific gravity of urine in two subsequent portions with a loss of 2% of body weight indicates the absence of stimulation of endogenous vasopressin.
Test with intravenous injection of 50 ml of 2.5% solutionNaCl within 45 minutes. In diabetes insipidus, the volume and density of urine do not change significantly. With psychogenic polydipsia, an increase in the osmotic concentration of plasma rapidly stimulates the release of endogenous vasopressin and the amount of urine excreted decreases, and its specific gravity increases.
A test with the introduction of vasopressin preparations - 5 IU intravenously or intramuscularly. In true diabetes insipidus, health improves, polydipsia and polyuria decrease, plasma osmolarity decreases, and urine osmolarity increases.
Differential diagnosis of diabetes insipidus
According to the main signs of diabetes insipidus - polydipsia and polyuria, this disease is differentiated from a number of diseases occurring with these symptoms: psychogenic polydipsia, diabetes mellitus, compensatory polyuria in CRF (chronic renal failure).
Nephrogenic vasopressin-resistant diabetes insipidus (congenital or acquired) is differentiated on the basis of polyuria with primary aldosteronism, hyperparathyroidism with nephrocalcinosis, malabsorption syndrome in chronic enterocolitis.
With diabetes
Table 22
With psychogenic polydipsia
Table 23
|
Sign |
Diabetes insipidus |
Psychogenic polydipsia |
|
Craniocerebral infections, traumas (including surgical) |
Gradual Psychotrauma, psychogenic stress |
|
|
The presence of a tumor |
Tumors of the pituitary gland, sarcoma, lymphogranulomatosis, etc. |
Missing |
|
Osmolarity: | ||
|
Dry food test (no more than 6-8 hours) |
No dynamics |
The amount of urine decreases, the specific gravity and osmolality are normalized |
|
Well-being with this test |
Deteriorates, thirst becomes excruciating |
Condition and well-being are not violated |
|
Intravenous injection test 50 ml 2.5% NaCl |
The amount of urine and its density without dynamics |
The amount of urine decreases, and the specific gravity |
|
Well-being is improved, polydipsia and polyuria are reduced |
Feeling worse (headaches) |
Central (hypothalamo-pituitary) with nephrogenic diabetes insipidus
Table 24
|
Sign |
Central diabetes insipidus |
Diabetes insipidus nephrogenic |
|
Cranial trauma, infections, tumors. |
Family; hyperparathyroidism; taking drugs - lithium carbonate, demeclocycline, methoxyflurane |
|
|
Test with intravenous administration of 5 IU of vasopressin |
The state of health improves, polydipsia and polyuria decrease. Plasma osmolality , and urine |
No dynamics |
|
Changes are found in urine |
Absent |
Albuminuria, cylindruria |
|
Blood creatine | ||
|
Arterial hypertension |
BP often |
Diabetes insipidus treatment
Etiological : for tumors of the hypothalamus or pituitary gland - surgery, or radiation therapy, cryodestruction, introduction of radioactive ytrium.
For infectious processes - antibacterial therapy.
With hemoblastosis - cytostatic therapy.
Substitution therapy - drugs that replace vasopressin:
Adiuretin(synthetic analogue of vasopressin) intranasally 1-4 drops in each nostril 2-3 times a day; available in 5 ml vials, 1 ml - 0.1 mg of active substance;
Adiurecrin(extract of the posterior lobe of the pituitary gland of a large cattle). Available in powder form. Inhale 0.03-0.05 2-3 times a day. The duration of action of one inhalation is 6-8 hours. In inflammatory processes in the nasal cavity, the absorption of adiurecrine is disrupted and its effectiveness is sharply reduced;
RP: adiurecrini 0.05Dsd # 30.S. inhale through the nose, 1 ml ampoules;
Pituitrin. Release form 5 units of activity. Water-soluble extract of the posterior lobe of the pituitary gland of cattle. Introduced in 5 units (1 ml) 2-3 times a day / m. Often causes symptoms water intoxication(headaches, abdominal pain, diarrhea, fluid retention) and allergies;
DDAVP(1 desamino-8D-arginine-vasopressin) - a synthetic analogue of vasopressin;
diuretics of the thiazide group(Hypothiazide and others). Hypothiazide 100 mg per day reduces glomerular filtration, Na + excretion with a decrease in the amount of urine. The effect of thiazide diuretics is not detected in all patients with diabetes insipidus and weakens over time;
Chlorpropamide(an oral hypoglycemic drug) is effective in some people with diabetes insipidus. Tablets 0.1 and 0.25. Assign in daily dose 0.25 in 2-3 doses. The mechanism of antidiuretic action is not fully understood, it is assumed that it potentiates vasopressin, at least with minimal amounts in the body.
To avoid hypoglycemia and hyponatremia, it is necessary to control the level of glucose and Na + in the blood.
("Diabetes") - a disease that develops when there is insufficient release of antidiuretic hormone (ADH) or a decrease in the sensitivity of the renal tissue to its action. As a result, there is a significant increase in the amount of fluid excreted in the urine, an insatiable feeling of thirst arises. If fluid losses are not fully compensated for, then dehydration of the body develops - dehydration, distinctive feature which is concomitant polyuria. The diagnosis of diabetes insipidus is based on clinical picture and determining the level of ADH in the blood. To find out the reason for the development of diabetes insipidus, a comprehensive examination of the patient is carried out.
ICD-10
E23.2

General information
("Diabetes") - a disease that develops when there is insufficient release of antidiuretic hormone (ADH) or a decrease in the sensitivity of the renal tissue to its action. Violation of the secretion of ADH by the hypothalamus (absolute deficiency) or its physiological role with sufficient formation (relative deficiency) causes a decrease in the processes of reabsorption (reabsorption) of fluid in the renal tubules and its excretion in the urine of low relative density. With diabetes insipidus, due to the release of a large volume of urine, an insatiable thirst and general dehydration of the body develop.
Diabetes insipidus is a rare endocrinopathy that develops regardless of gender and age group of patients, more often in people 20-40 years old. In every 5th case, diabetes insipidus develops as a complication of neurosurgical intervention.

Classification
Complications
Diabetes insipidus is dangerous by the development of dehydration of the body, in cases where the loss of fluid in the urine is not adequately replenished. Dehydration manifests itself abruptly general weakness, tachycardia, vomiting, mental disorders, blood clots, hypotension up to collapse, neurological disorders. Even with severe dehydration, polyuria persists.
Diagnosis of diabetes insipidus
Typical cases allow one to suspect diabetes insipidus by insatiable thirst and the release of more than 3 liters of urine per day. To assess the daily amount of urine, the Zimnitsky test is carried out. When examining urine, its low relative density is determined (<1005), гипонатрийурию (гипоосмолярность мочи - 100-200 мосм/кг). В крови выявляются гиперосмолярность (гипернатрийемия) плазмы (>290 mosm / kg), hypercalcemia and hypokalemia. Diabetes mellitus is excluded by the determination of fasting blood glucose. With the central form of diabetes insipidus, a low content of ADH is determined in the blood.
The results of the dry-eating test are indicative: abstinence from fluid intake for 10-12 hours. With diabetes insipidus, weight loss of more than 5% occurs, while maintaining a low specific gravity and hypoosmolarity of urine. The causes of diabetes insipidus are clarified during X-ray, neuropsychiatric, ophthalmological examinations. Volumetric formations of the brain are excluded by conducting an MRI of the brain. To diagnose the renal form of diabetes insipidus, ultrasound and CT of the kidneys are performed. Nephrologist consultation is required. Sometimes a kidney biopsy is required to differentiate renal pathology.
Diabetes insipidus treatment
Treatment for symptomatic diabetes insipidus begins by addressing the cause (eg, tumor). For all forms of diabetes insipidus, substitution therapy with a synthetic analogue of ADH, desmopressin, is prescribed. The drug is administered orally or intranasally (by instillation into the nose). A prolonged-release preparation from an oily solution of pituitrin is also prescribed. In the central form of diabetes insipidus, chlorpropamide, carbamazepine are prescribed, which stimulate the secretion of antidiuretic hormone.
Correction in progress water-salt balance by infusion of saline solutions in large volumes. Sulfanilamide diuretics (hypochlorothiazide) significantly reduce urine output in diabetes insipidus. Nutrition for diabetes insipidus is based on protein restriction (to reduce the load on the kidneys) and an adequate intake of carbohydrates and fats, frequent meals, and an increase in the number of vegetable and fruit dishes. From drinks it is recommended to quench thirst with juices, fruit drinks, compotes.
Forecast
Diabetes insipidus developing in postoperative period or during pregnancy, often has a transient (transient) character, idiopathic - on the contrary, persistent. With appropriate treatment, there is no danger to life, although recovery is rarely recorded.
The recovery of patients is observed in cases of successful removal of tumors, specific treatment of diabetes insipidus of tuberculous, malarial, syphilitic genesis. With the correct appointment of hormone replacement therapy, the ability to work is often preserved. The least favorable course of the nephrogenic form of diabetes insipidus in children.

What is diabetes insipidus?
Diabetes insipidus is a disease manifested by the secretion of 3 to 20 liters of urine per day (urine is clear, with little content salts and low density). The amount of liquid drunk by a patient with diabetes insipidus also ranges from 3 to 20 liters (corresponding to the volume of urine excreted by him). The most obvious and early signs of diabetes insipidus are polyuria, dehydration, and intense thirst. This disease is detected most often in people aged 18 to 25 years. The incidence of the disease is 3 people per 100 thousand people.
Causes of occurrence


The onset of this disease is most often associated with dysfunction of either the hypothalamus or the pituitary gland. If their functions are impaired, a decrease in the synthesis of antidiuretic hormone (absolute deficiency) may occur. A relative deficiency can develop with normal secretion of the hormone, but its insufficient physiological effect on the body. This disease develops in 20% of cases as a result of neurosurgical intervention.
Since the maintenance of the water-salt balance is normally regulated in the human body with the help of thirst, renal excretory function and the hormone vasopressin, a serious disruption in the functioning of one of these components leads to the development of diabetes insipidus.
Diabetes insipidus can occur:
- in the presence of neoplasms in the brain, vascular lesions or metastases that affect the functioning of the pituitary gland or hypothalamus;
- with traumatic brain injury;
- with primary tubulopathy (inflammatory, degenerative or cystic kidney damage, in which tubular transport is impaired);
- when transmitted by genetic means;
- due to infectious disease(syphilis, encephalitis, malaria, tuberculosis, etc.)
Types of diabetes insipidus
Diabetes insipidus is divided into the following types:
- neurogenic;
- nephrogenic;
- insipidary syndrome;
- gestagenic (during pregnancy);
- idiopathic diabetes insipidus.


Diabetes insipidus of the neurogenic type develops with violations of the synthesis of the hormone vasopressin. Vasopressin is the only hormone that regulates the reabsorption of fluid by the kidney. With inadequate secretion of this hormone by the hypothalamus in the collecting ducts of the kidneys, the reabsorption of water is significantly reduced, due to which a large amount of urine is excreted and excreted from the body.
In the nephrogenic type of diabetes mellitus, the cause of its development is a reduced renal response to the effects of vasopressin. Symptoms of diabetes insipidus can develop against a background of nervous stress (insipidus syndrome).
Progestogenic diabetes insipidus develops in pregnant women, usually in the third trimester as a result of the destruction of vasopressin by the enzyme arginine aminopeptidase and disappears after delivery. Symptoms of this disease during pregnancy are especially acute.
Idiopathic diabetes insipidus is a disease whose causes cannot be determined. In such cases, most often it turns out that diabetes insipidus is in the patient's immediate family. Idiopathic diabetes insipidus develops suddenly, rapidly and in acute form... The cause of diabetes insipidus remains unclear in about a third of cases.
Symptoms
Symptoms of diabetes insipidus, in addition to polyuria (increased urine production) and severe thirst, include:
- nausea and vomiting;
- lack of appetite;
- weight loss;
- the occurrence of seizures;
- insomnia;
- decreased mental alertness;
- irritability;
- dry skin;
- decreased sweating.
In this case, urination occurs mostly at night. The volume of urine in diabetes insipidus exceeds 3 liters per day. As a result of diabetes insipidus, in men there is a decrease in potency, in women - a violation of the monthly cycle, and in children - a lag in sexual and physical development. All of the listed symptoms of diabetes insipidus in children can be supplemented by enuresis.
Complications
With a restriction in the use of fluids in patients with diabetes insipidus, headache, tachycardia, dry mucous membranes, fever, nausea and vomiting, blood clots, mental disorders occur.
In this disease, the renal pelvis, ureters and bladder expand, the stomach stretches and sinks, chronic intestinal irritation and dyskinesia (impaired motility) of the biliary tract develop.
Diagnosis of the disease
Diagnosis of diabetes insipidus does not cause any difficulties, since the symptoms of this disease are too obvious. Even when examined by a doctor, such a patient cannot part with a bottle containing a drink. And yet, in the diagnosis, it is necessary to exclude diabetes mellitus, uncontrolled intake of diuretics (both medicinal and in the form of teas), metabolic disorders and the intake of drugs that inhibit the effect of vasopressin.


With diabetes insipidus, the urine excreted by the body is observed increased content sodium, the relative density of urine is lowered. The main task of the doctor is to determine the source that provoked the development of the disease (brain, kidneys, pregnancy or a nervous disorder). To recognize the relationship of diabetes insipidus to stress exposure, you can use the dry food test: with dry food (refusal to take fluids for 10-12 hours), polyuria stops.
To determine the cause of diabetes insipidus, the patient:
- an MRI of the brain may be prescribed;
- an ophthalmological examination is carried out;
- X-ray examination is carried out;
- an ultrasound or CT scan of the kidneys is prescribed;
- a neuropsychiatric examination is carried out;
- the weight, pulse and pressure of the patient are measured.
In the blood of patients with diabetes insipidus, plasma hyperosmolarity, a lack of potassium and an excess of calcium are detected. Since diabetes mellitus and diabetes insipidus have similar symptoms, differentiation from diabetes mellitus is made by determining the level of fasting glucose.
In order to confirm the diagnosis, a dry eating test is performed. In the case of diabetes insipidus, there is a sharp loss of body weight, an increase in the osmolarity of blood and urine, the patient feels unbearable thirst.
Diabetes insipidus treatment


Treatment depends on the underlying cause of the symptoms of diabetes insipidus. For all forms, the antidiuretic desmopressin is used in the form of tablets or drops for instillation into the nose. The dose of this drug largely depends on the body weight, age of the patient and the severity of his disease, therefore, it is determined by the attending physician on an individual basis. Studies have shown that desmopressin treatment is safe for pregnant women and fetuses.
It is also carried out by introducing large volumes of saline solutions into the body to correct the water-volitional balance. With the psychogenic nature of diabetes insipidus, its symptoms can also disappear with psychotherapy or taking psychotropic drugs.
With diabetes insipidus, except drugs, a diet is prescribed. It is necessary to reduce salt intake to 5 g per day and protein intake to reduce the burden on the kidneys. The consumption of fats and carbohydrates can be left on normal level... The diet can be expanded with vegetables, fruits and lactic acid products. And to quench your thirst, you can use juices, compotes, fruit drinks containing a small amount of carbohydrates.
Forecast
The prognosis of diabetes insipidus depends on what disease provoked it. If the disease is provoked by a neoplasm in the brain, then with successful removal of the tumor, the symptoms of diabetes insipidus disappear. With the development of diabetes insipidus due to an infectious disease, complete recovery is possible with the cure of the underlying disease. However, such cases are rare. The resulting diabetes insipidus in pregnant women most often disappears after childbirth.
Diabetes insipidus can be sick all your life, while maintaining your ability to work with the help of hormone replacement therapy. If there are symptoms of diabetes insipidus in children, the origin of which is nephrogenic, the chances of survival are small.
This is rare endocrine disease... It is very serious and is associated with a lack of the hormone vasopressin in the blood. This hormone performs protective functions, the composition of sodium in the blood and body fluids is stabilized. If vasopressin levels begin to decline, symptoms of illness appear immediately.
Symptoms of diabetes insipidus
The main clinical symptoms diseases - polyuria and polydipsia (excessive thirst).
One of the first symptoms of diabetes insipidus is frequent urination... Up to 5 liters of urine can be excreted per day, moreover, it does not have a characteristic odor and is transparent. The patient develops dryness of the mucous membrane, as well as the skin.
Weight drops sharply, thirst torments.
The patient complains about headache, dizziness. Nausea and vomiting may occur. This disease is a consequence of damage to some parts of the brain that occurs during trauma, with the occurrence of tumor neoplasms, as well as infection.
Diabetes insipidus occurs, most often with a hereditary predisposition to this disease. The heirs of the patient should remember this and take all preventive measures.
The main symptoms of diabetes insipidus include the following:
- profuse urination (up to 3-15 liters of urine per day);
- the main volume of urination occurs at night;
- thirst and increased fluid intake;
- dry skin, nausea and vomiting, convulsions;
- mental disorders (insomnia, emotional lability, decreased mental activity).
Even if the patient is limited in fluid intake, urine will still be excreted in large quantities, which will lead to general dehydration.
In addition to common symptoms, there are a number of individual symptoms that occur in patients of different sex and age:
| Symptoms and Signs | |
| Diabetes insipidus in women symptoms | Men get diabetes insipidus as often as women. Most of all new cases of pathology are observed in young people. Usually the disease debuts in patients between the ages of 10 and 30. The main symptoms indicating impaired vasopressin secretion and the development of diabetes insipidus are:
|
| Diabetes insipidus in men | The development of this disease begins suddenly, accompanied by such phenomena as polydipsia and polyuria - a strong feeling of thirst, as well as an increase in the frequency and volume of urination. More detailed clinical signs in women may include:
The presence of a woman with diabetes insipidus is indicated following signs:
If a renal form of diabetes is detected, a consultation with a urologist is required. If the genitals are involved in the process and the flow of the menstrual cycle is disturbed, a consultation with a gynecologist is necessary. |
| In children | Differences in the symptoms of diabetes insipidus in adult patients and adolescent children are insignificant. In the latter case, a more striking manifestation of pathology is possible:
|
Causes of diabetes insipidus in women
The causes depend on the type of disease in women. In the first type, they are:
- a tumor in the hypothalamus;
- complications after brain surgery;
- encephalitis;
- various injuries and injuries to the head;
- circulatory disorders in the hypothalamus;
- metastases in malignant tumor(cancer) to the brain (they are ways to interfere with the full activity of the pituitary gland);
- genetic factors contributing to the appearance of this pathology.
Diabetes insipidus during pregnancy
In pregnant women, diabetes insipidus occurs in a more complex form, which is generally associated with changes in the body.
When this disease is detected, it is necessary to systematically visit a doctor in order to timely diagnose, provide assistance and choose the right treatment. Thirst at night and urinary incontinence during sleep are added to the common symptoms of kidney disease in pregnant women.
The manifestation of this disease in the absence of constant medical supervision and treatment leads to certain complications during pregnancy.
These include possible dehydration associated with low level sodium in the blood, brain damage, arrhythmia, problems with blood pressure and insufficient production of oxytocin, necessary for labor (its lack affects the weakening of contractions).
What drugs to treat diabetes insipidus
- Vasopressin is a hormone produced by the hypothalamus that increases the reabsorption of water by the kidneys, thus preventing dehydration.
- Desmopressin is a synthetic analogue of vasopressin that helps to reduce urine output; used to treat diabetes insipidus.
The drug of choice in the treatment of CND is synthetic (genetically engineered) arginine-vasopressin (desmopressin; 1-deamino-8, D). The soluble form of the drug is applied either intranasally, 1-2 drops (10-20 mcg) 1-2 times a day, or subcutaneously, 5-10 IU 2-3 times a day. The tablet form contains 100 or 200 mcg in 1 tablet. The dose is selected individually. It is 1 to 3 tablets per day.
An oily solution of long-acting vasopressin, vasopressin tannate, is injected intramuscularly, at a dose of 2.5-5 U, slightly heated beforehand and thoroughly shaking the ampoule.
In cases of a relatively mild course of CDI (type 2, 3, 4), the anticonvulsant drug finlepsin (tegretol) can be used at a dose of 200-600 mg 2 times a day, clofibrate 500 mg 4 times a day or chlorpropamide 200-300 mg 1 time in a day. In nephrogenic diabetes insipidus, hypothiazide 50-100 mg per day or other diuretics that increase sodium excretion are used. This treatment requires mandatory restriction of salt in the diet and constant monitoring of serum potassium.
Timely diagnosis and effective therapy diabetes insipidus is necessary not only to improve the quality of life of patients, but also to prevent atony Bladder followed by hydronephrosis.
Adequate treatment is especially important for the elderly, who, due to dysfunction of the thirst center, have a real danger of severe dehydration with damage to the central nervous system and even death.
Treatment of diabetes insipidus in children
Diabetes insipidus in a child is referred to as idiopathic. It can start at any age. In the idiopathic form, the deficiency of antidiuretic hormone depends on dysfunction of the hypothalamic-pituitary axis. It is assumed that there is a congenital biochemical defect in this area, which manifests itself in symptoms if the body is influenced by unfavorable environmental factors.
Diabetes insipidus in children can have a post-traumatic etiology. It can occur as a result of injuries that occur above the pituitary stalk in a skull injury with a fracture of the skull base and rupture of the pituitary stalk, or after neurosurgical operations and manipulations.
Permanent polyuria can appear after a long time after injury - 1-2 years. In such cases, doctors find out the child's condition during this time, trying to find short periods when typical symptoms could appear. Accidental trauma to the skull is a very rare cause of diabetes insipidus.
The reason for the absolute deficiency of the antiduretic hormone may be damage to the neurohypophysis of any of the following reasons:
- histiocytosis
- tumors over the Turkish saddle and in the area of the chiasm optic nerve
- fracture of the base of the skull, surgery
- infections (tuberculosis, encephalitis)
- Wolfram syndrome
- hereditary forms
- 2-3 times a day, the child is given 0.5 cups of sauerkraut brine, which contains a lot of lactic acid. Or give 4 times a day fresh red beet juice, 1/4 cup.
- In 250 grams of water, put 1 tbsp. l. leaves and young shoots of blueberries, boil over low heat for 10 minutes, cool and season. Give the child 6 times a day for a quarter of a glass.
- In 250 grams of water put 1 tbsp. l. plantain seeds, boiled for 5 minutes, set to cool, then filtered. Give the child one tablespoon 3 times a day.
- In one glass of water, dilute 2 tbsp. spoons of juice from the roots and leaves of burdock. The resulting mixture is divided into 3 doses, you need to drink it in 1 day (3 times). May root burdock is sometimes made into a salad, which is considered good remedy phytotherapy of diabetes insipidus.
- At the beginning of the disease, 1 tbsp. a spoonful of chopped aspen bark is poured with two glasses of water and boiled over low heat for half an hour. Then they wrap it up, insist for about 3 hours, filter and give the child 3 times a day for a sixth of a glass, you need to give the infusion before meals, the course is from 2 to 3 months.
The course of treatment of diabetes insipidus is selected individually for children.
Congenital disease will require regular intravenous glucose. Such procedures are prescribed for children under three years of age.
In this case, substitution therapy is not performed. Other drugs are used to treat babies over three years old. In the presence of complications, it becomes necessary to perform an operation.
Drugs for the treatment of diabetes insipidus in children
Drugs used in the treatment of diabetes insipidus in children:
- Intravenous administration of a synthetic substitute for vasopressin (Desmopressin).
- Therapy with drugs that stimulate the production of its own hormone vasopressin (Chlorpropamide).
- Treatment with drugs that reduce the amount of sodium in the blood (Klopamid, Indapamide).
- Reception of antidiuretic hormone analogues (Vazomirin, Minirin, Adiuretin SD).
Diagnosis of diabetes insipidus
A doctor can correctly diagnose and distinguish between a certain type of diabetes and polydipsia by conducting a diagnosis in several stages.
Differential diagnosis of diabetes insipidus on an outpatient basis begins with interviewing the patient and finding out the following:
- the amount of fluid you drink, urine excretion per day;
- the presence of night thirst and nocturnal enuresis;
- the presence of a psychological cause of thirst, a private urge to urinate (when a person is distracted, the symptoms disappear);
- are there any provoking diseases (tumors, trauma, endocrinological disorders).
If, after the survey, all the symptoms indicate the presence of a disease, then a medical examination is carried out, based on the results of which a diagnosis is made and treatment is prescribed.
The survey includes:
- Ultrasound of the kidneys;
- blood analysis,
- urine (osmolarity, density);
- computed tomography of the brain;
- the Zimnitsky test is carried out;
- the level of sodium, potassium, nitrogen, glucose, urea in the blood serum is determined.
Treatment of renal diabetes insipidus
First of all, a sufficient flow of fluid into the body is ensured, then, if necessary, medications are prescribed.Medication treatment
Treatment of renal diabetes insipidus is the practice of prescribing medicinal substances that, paradoxically, reduce the amount of urine - thiazide diuretics (diuretics):
- Hydrochlorothiazide,
- Indapamide,
- Triampur.
Their use is based on the fact that they prevent the reabsorption of chlorine in the urinary tubules of the nephron. As a result, the sodium content in the blood decreases slightly, and the reabsorption of water is enhanced.
Anti-inflammatory drugs (Ibuprofen, Indomethacin, and Aspirin) are sometimes prescribed as an adjunct to treatment.
Their use is based on the fact that they reduce the flow of certain substances into the urinary tubules of the nephron, thereby reducing the volume of urine and increasing its osmolality. but successful treatment diabetes insipidus is impossible without observing certain dietary rules.
Diet
Nutrition for diabetes insipidus has the goal of reducing the volume of urine excreted and thirst, as well as replenishing the nutrients that are lost in the urine.
Therefore, first of all, the use of salt is limited (no more than 5-6 grams per day), and it is handed out, and food is prepared without adding it.
Dried fruits are beneficial because they contain potassium, which enhances the production of endogenous (internal) vasopressin. In addition, it is necessary to give up sweets so as not to increase thirst. It is also recommended to refrain from drinking alcoholic beverages.
A sufficient amount of fresh vegetables, berries and fruits, milk and lactic acid products.
In addition, juices, compotes, fruit drinks are useful.
It is very important that phosphorus enters the body (it is necessary for the normal functioning of the brain), therefore it is recommended to consume lean fish, seafood and fish oil. In addition, lean meats and eggs (yolk) are beneficial.
However, it must be remembered that with diabetes insipidus, you should still limit proteins, so as not to increase the burden on the kidneys. Whereas fats (for example, butter and vegetable oil), as well as carbohydrates (potatoes, pasta, and others) must be present in the diet in sufficient quantities. It is advisable to eat fractionally 5-6 times a day. Most of all, table number 7 or number 10 corresponds to all these recommendations.
Diabetes insipidus treatment with folk remedies
Treatment of diabetes insipidus with folk remedies cannot produce the desired effect if not accompanied by drug therapy. When traditional medicine is combined with traditional methods, the effect can be enhanced, and the amount of medication is reduced over time, but not reduced to zero.
The first thing that traditional medicine suggests is to sharply limit salt in the patient's diet and increase the dose of milk. Instead of fried meat, it is recommended to eat boiled meat, as well as more egg yolks and fish. Desirable in the menu of patients with diabetes insipidus cancer and brains.
Nuts

Very useful in the treatment of folk remedies for diabetes insipidus, walnuts... The daily rate is 100 grams of nucleoli. But until the nuts are ripe, an infusion of young walnut leaves can be a good thirst quencher.
Five grams of leaves are crushed, poured with boiling water in a volume of 200 milliliters, insisted and drunk instead of tea. All this helps to stop the development of the disease.
Popular recipes include:
- Combine 1 part calamus root and valerian, 2 parts each fennel seeds and blue cyan herb, 5 parts each veronica, thyme and meadowsweet grass. In the evening 1 tbsp. brew the resulting mixture in a thermos with 500 ml of boiling water, insist overnight, strain. Take the next day, in three doses, half an hour before meals. The course of treatment lasts 2-3 months.
- Combine 1 part of tricolor violet flowers, 2 parts each of linden flowers and white mistletoe grass, 3 parts of wild rosemary flowers, 4 parts each of St. John's wort, oregano and plantain. In the evening 1 tbsp. brew the resulting mixture in a thermos with 500 ml of boiling water, insist overnight, strain. Take the next day, in three divided doses, half an hour before meals. The course of treatment lasts 2-3 months.
- Combine 1 part of fragrant rue herb, 2 parts each of chamomile flowers and dill seeds, 3 parts each of St. John's wort and a medicinal letter, 4 parts of licorice root, 5 parts of oregano herb. In the evening 1 tbsp. brew the resulting mixture in a thermos with 500 ml of boiling water, insist overnight, strain. Take the next day, in three doses, half an hour before meals. The course of treatment lasts 2-3 months.
Defeating thirst
Plants help to quench the thirst of the sick.
Burdock
Burdock serves as a savior until autumn.
More precisely, its roots. If you grind them into powder, then a teaspoon of such powder, diluted in half a glass of heated milk, will quench your thirst.
You can make a burdock drink in the evening for the next day. To do this, grind 60 grams of roots, pour a liter of boiling water and leave overnight. In the morning, the filtered infusion can be drunk, if thirst arises, 130 milliliters each.
Elder

The infusion of black elderberry flowers helps well. 20 grams of flowers are infused in 200 milliliters of boiling water for at least an hour, filtered, a teaspoon of honey is added and drunk three times between meals.
Defeats thirst and propolis
Before you swallow propolis, you need to chew it for a couple of minutes. Effective remedy in folk medicine, it is considered an infusion of collecting herbs.
You need to take crushed dandelion root, lingonberry leaves - three tablespoons each, two each - dioecious nettle leaves, chamomile flowers, veronica grass, birch buds. Mix everything well.
A mixture in the volume of a tablespoon is poured with boiling water in a volume of 200-250 milliliters, insisted for three hours. The filtered infusion should be drunk half an hour before a meal, 100 milliliters each.
Pea flour, motherwort herb
In folk medicine, in the treatment of diabetes insipidus, pea flour and motherwort herb are used. The disease is difficult, with seizures.
Pharmaceutical glycerin is used to remove them.
A tablespoon of glycerin is enough to relieve pain.
It is possible and necessary to fight the disease, this disease is not a sentence and is treatable.
To do this, you must follow the advice of specialists, including representatives of traditional medicine.
Video: Life is great! Diabetes insipidus
Diabetes insipidus (or diabetes insipidus) is a rare chronic disease associated with dysfunction of the hypothalamus or pituitary gland, which is characterized by profuse urination and thirst. Why does this disease appear and is it possible to cope with this problem?
Diabetes insipidus(diabetes insipidus) is a rare condition in which the body cannot properly regulate fluids. This can lead to severe dehydration. People with diabetes insipidus tend to be very thirsty and excrete much more urine than usual due to hormonal imbalances.
Epidemiology
There is not much data on the epidemiology. However, this rare condition affects about 1 in 100,000 people, in equal numbers in both women and men.
What is the difference between diabetes mellitus and diabetes insipidus?
Diabetes insipidus (Diabetes mellitus) should not be confused with (DM), which is the result of a deficiency or immunity to, due to which the body cannot regulate the level of glucose (sugar) in the blood. ND is a completely different type of disease associated with the regulation of body fluids.
When the body's fluid regulation system is working properly, the kidneys filter the blood, excreting waste and excess fluids, which then becomes urine (urine).
Typically, a person produces 800-1500 ml of urine per day.
From the kidneys, urine travels through small tubes called ureters to the bladder, where it is stored until the bladder is full and urges to urinate.
A hormone called vasopressin (or antidiuretic hormone [ADH]) is the key to all of these processes. Antidiuretic hormone is produced by the hypothalamus, a small gland at the base of the brain. It is then stored in the pituitary gland, which is next to the hypothalamus, and released into the bloodstream when the body's fluid levels decrease.
In the bloodstream, the antidiuretic hormone signals the kidneys not to absorb all fluid from the body and excrete it through urine so that dehydration does not occur.
The pituitary gland secretes less vasopressin, or even no vasopressin at all, when fluid levels in the body are high. At that time, the person will produce more urine.
In diabetes insipidus, this system does not work properly.
Classification
The disease is divided into several main types:
- central diabetes insipidus - occurs when the production of vasopressin (a hormone that controls water exchange in the body) in the hypothalamus (the hemisphere in the diencephalon, which includes a large number of groups of cells that regulate the neuroendocrine activity of the brain) is insufficient;
- nephrogenic diabetes insipidus (NNSD) - occurs due to the inability to concentrate urine due to the impaired response of the renal tubules to vasopressin, which leads to the excretion of a significant amount of unconcentrated urine from the body;
- insipidary syndrome -characterized by polydipsia (intense thirst), polyuria (an increase in the volume of urine excreted per day);
- gestagenic diabetes insipidus - associated with increased activity of the placental enzyme that destroys vasopressin.
Most often, there are two types: central and nephrogenic.
According to the severity of the course, the following forms of diabetes insipidus are distinguished:
- easy - the allocation of up to 8 liters of urine per day;
- medium - the release of 8-14 liters / day;
- severe - discharge more than 14 liters / day.
Also, the disease is congenital or acquired forms.
Diabetes insipidus causes

While all diabetes insipidus is caused by dysregulation of vasopressin (an antidiuretic hormone), this dysregulation can be caused by many different factors. The cause of this disorder is the definition of each of the four types of disease.
Central diabetes insipidus is a consequence of insufficient production of antidiuretic hormone (ADH) in the hypothalamus or their inability to accumulate in the posterior lobe of the pituitary gland, from where they are secreted into the blood. Most often this is due to hypothalamic syndrome or brain lesions, due to:
- craniopharyngiomas;
- tuberculous;
Blunt head injuries and surgeries can also damage the hypothalamus, as can metastatic pituitary tumors.
Nephrogenic diabetes insipidus occurs due to malfunctioning of the renal tubules, they do not process antidiuretic hormone. This is due to kidney damage as a result of genetics, metabolic disorders (such as hypokalemia and hypercalcemia), heavy metal poisoning. It can also be caused by other medical conditions, such as:
- chronic type;
- renal;
Insipidary syndrome arises from a defect in the mechanism of thirst - a signal from the body that controls fluid intake in the hypothalamus. This defect causes continually abnormal thirst.
When someone is excessively thirsty, they drink much more than usual. Their high fluid intake causes the body to secrete less vasopressin, and this causes the kidneys to produce more urine.
As with the central type, the hypothalamic thirst mechanism can be damaged:
- head trauma;
- operation;
- infection;
- inflammation;
- brain tumors.
People can also suffer from the syndrome as a result of taking certain medications or mental health problems.
Gestational diabetes insipidus occurs during pregnancy and can be caused by two different factors:
- The placenta produces an enzyme that breaks down vasopressin in the mother's body, resulting in excessive urine production because the kidneys draw too much fluid from the bloodstream.
- The mother's body produces large amounts of a chemical called prostaglandin, which makes the kidneys less sensitive to vasopressin, as in the nephrogenic type of disease.
In many cases of gestational diabetes insipidus, the symptoms are mild and subtle, especially since the pregnancy itself causes many women to urinate frequently. However, dehydration during pregnancy can lead to complications, including:
- neural tube defects;
- low amniotic fluid;
- premature birth.
If you suspect you have a gestational type of illness, be sure to keep yourself hydrated and talk to your doctor right away.
Since it is directly caused by factors related to pregnancy, the gestational type of the disease usually disappears after the baby is born, but is likely to return in future pregnancies.
Approximately about 1/3 of cases of diseases are of unexplained origin. Doctors still fail to understand the causes of the disease in the body of a perfectly healthy person.
Signs and symptoms of diabetes insipidus

The disease leads to frequent thirst and urination, these are the most common and overt symptoms.
In extreme cases, urination may exceed 20 liters per day. The urine has no color, and there is a small amount of salt precipitation in the volume.
Also, with diabetes insipidus, a patient may experience the following chain of symptoms:
- headache;
- sleep is disturbed, insomnia appears;
- weight is lost (very often with diabetes insipidus, the patient rapidly loses weight);
- decreased libido, disrupted menstrual cycle in women.
If you find several similar signs and symptoms in your body, an urgent appeal to an endocrinologist is required. .
Children's symptoms of the disease are almost the same as in adults. Symptoms of the disease in newborns:
- vomit;
- the child is losing weight greatly and noticeably;
- abnormally low or very high body temperature;
- baby to urinate repeatedly and abundantly.
Only in newborn children, the disease can be expressed clearly and have all the ensuing consequences.
Complications
The disease is dangerous by the development of dehydration of the body, in cases where the loss of fluid in the urine is not replenished.
With the disease, activity is also disrupted of cardio-vascular system, arise mental disorders as well as neurosis. In women, it can be disturbed.
Female body suffers especially, complications from the ureters and bladder are likely, manifested in the night. In rare cases, the disease can lead to visual impairment up to blindness.
Complications of diabetes insipidus occur only when the patient does not pay attention to the symptoms that bother him.
Important! With diabetes insipidus, you should not stop drinking, however, you cannot drink too much, this will only aggravate the patient's situation. You need to determine for yourself the golden mean of daily fluid intake. It is advisable to give preference only to clean water, drink in moderation, in small sips.
Diagnostics
At the first visit, an endocrinologist / nephrologist will conduct an examination. The examination will help to find out the amount of water that a person drinks per day, whether there are problems with urination and with the menstrual cycle.
From the information received, the specialist will either prescribe treatment or send the patient to laboratory diagnostics to once again verify the correctness of the diagnosis.
Diagnostics includes:
- ultrasound examination of the kidneys;
- detailed biochemical analysis blood;
- X-ray examination of the skull;
- computed tomography of the brain;
- a Zimnitsky test is assigned (an accurate calculation of the daily drunk and secreted fluid).
The diagnosis of diabetes insipidus is based on the following laboratory findings:
- high sodium content in the blood;
- low relative density of urine;
- high level of osmolarity of blood plasma;
- low urine osmolarity.
Also, doctors may ask for a blood test for C-peptide in order to exclude diabetes mellitus.
Additionally, the patient can be examined by a neurologist and neurosurgeon.
Diabetes insipidus treatment

Treatment is often carried out by nephrologists, who are doctors specializing in kidney disease, or endocrinologists who specialize in conditions involving hormone-producing glands (including the hypothalamus and pituitary gland).
The main remedy is to drink enough fluids to prevent dehydration. However, beyond this, treatment is tailored to the specific type of disease.
Central diabetes insipidus therapy.
Medicines needed to treat the central type of disease:
- Miskleron, Carbamazepine, Chlorpropamide(drugs are used to stimulate the production of the hormone vasopressin);
- Minirin(desmopressin). A drug with a vasoconstrictor effect. The composition contains the substance desmopressin, which is similar in structure to the hormone vasopressin. During a meal, Minimirin should be taken orally, an hour before taking the medicine, the amount of fluid taken should be halved.
Therapy of nephrogenic diabetes insipidus.
Treatment for NDDM focuses on addressing the underlying cause of the disease, whenever possible. This may mean clearing a blockage in urination, stopping medication, or normalizing blood calcium or potassium levels.
When treating a nephrogenic type of disease, it will also be important to ensure the flow of fluid directly to the organs and tissues. Recommended the following drugs for treatment:
- Indapamide... This medication will provide reduced urine production, which will help replenish fluid in the body;
- Triampur... It also reduces urine production and helps replenish water in the body.
Data medicinal substances are used to stop the reverse absorption of chlorine in the kidney ducts. When taking these medications, the amount of sodium in the blood significantly decreases and occurs enhanced process, in which water is absorbed back into organs and tissues.
Treatment of the incipient syndrome.
The insipid syndrome does not yet have effective methods treatment, so symptom management is the mainstay of therapy. Doctors recommend sucking on hard candy or sour candy to keep your mouth full of saliva, which can help reduce your thirst. Small doses of desmopressin before bed can help reduce the number of times people need to get up to use the bathroom.
Therapy of gestagenic diabetes insipidus.
Desmopressin is also prescribed for this type of disease. The drug can help even in cases where the placental enzyme breaks down vasopressin, because the enzyme does not have the same effect on the synthetic hormone.
Important! Do not take medications as a therapy for the disease on your own, be sure to consult with a specialist before using.
Diet and nutrition

The main task health food with diabetes insipidus is a gradual decrease in the excreted urine per day and the fight against severe thirst.
It is necessary to refrain from eating foods that contain protein, and to introduce a sufficient amount of fats and carbohydrates into the diet. Food is prepared without adding salt.
Foods needed to include in the diet:
- Lean meat (such as chicken, red, or white)
- nuts;
- various cereals. It is recommended to give preference to buckwheat, oat and rice;
- vegetables and fruits;
- berries;
- milk;
- rosehip broth;
- seafood;
- green tea;
- water with lemon.
- black and red pepper;
- mustard;
- vinegar;
- smoked dishes;
- pickles and marinades;
- crackers, chips and fast food.
Diet for the day
With this disease, it is imperative to follow a certain diet. Approximate daily meals:
- the first breakfast - an omelette (steamed) of two eggs, vinaigrette (with vegetable oil), tea with lemon;
- second breakfast - oatmeal, three bars of dark chocolate, jelly;
- lunch - vegetable soup, boiled white meat, stewed carrots, milk;
- afternoon tea - salad of cucumbers and tomatoes on vegetable oil, one boiled egg;
- dinner - boiled fish, boiled potatoes, sour cream, tea with lemon.
Throughout the day, you need to pay special attention to drinking plenty of fluids. In diabetes insipidus, the body needs water more than ever to compensate for the loss of fluid during dehydration.
Food should be taken fractionally: 4-5 times a day.
Important! The patient must monitor the use, firstly, white bread, secondly, butter and, finally, thirdly, a particularly harmful product at the moment - sugar.
Compliance with the diet will help the patient speed up the healing process and return to a fulfilling life sooner.
Prophylaxis
For people who have a predisposition to the onset of pathology, it will not be superfluous to sometimes, at least at least 2 times a year, do an x-ray of the kidneys.
If you have or persistent thirst, you should immediately consult a doctor to avoid possible consequences.
Forecast
At correct treatment the prognosis for people suffering from diabetes insipidus is favorable. Central diabetes insipidus responds much more easily to treatment than nephrogenic diabetes.
Although patients with diabetes insipidus are rapidly dehydrated, mortality from this is rare in previously healthy adult patients. Children and the elderly, on the other hand, are at higher risk of dying from severe dehydration.
Interesting