Causative agents of infectious diseases and factors of their pathogenicity. Factors of pathogenicity of microorganisms infection infection totality Pathogenic factors
| " |
1. outer membrane protein invasin - provides resistance to phagocytosis;
2. enzyme superoxide dismutase - antiphagocytic activity of Salmonella;
3. endotoxin - the development of fever;
4. enterotoxin - has homology with cholera enterotoxin.
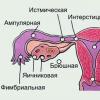
Salmonella can cause two groups of diseases in humans: 1) anthroponotic - typhoid fever and paratyphoid fever A and B; 2) zooanthroponic - salmonellosis.
The causative agents of typhoid fever are S. typhi, paratyphoid A - S. paratyphi A, and paratyphoid B - S. paratyphi B.
The main clinical manifestations: cyclic course, damage to the lymphatic apparatus of the small intestine, fever (fever by 4-7 days), intoxication, the appearance of a roseolous rash, the abdomen is swollen due to the accumulation of a large amount of gases in the intestines, delirium, hallucinations, drop in blood pressure, collapse, the tongue on the back is lined with a dirty-white coating, clean at the edges and from the tip, teeth marks are visible on the lateral surface of the tongue. Complications - perforation of the small intestine and intestinal bleeding. Immunity after an illness is tense and long.
Source of infection : a sick person and a bacteriocarrier that release the pathogen into the external environment with feces, urine, saliva. Ways of transmission: water, contact, food (milk, sour cream, cottage cheese, minced meat).
Laboratory diagnostics. The material for research is determined by the nature of the infectious process:
2. bowel movements
4. duodenal contents
6. corpse (pieces of parenchymal organs, blood from the heart, bile, contents and a segment of the small intestine).
Methods of laboratory diagnostics. 1 week of the disease and during the entire febrile period - the method of blood culture - blood culture in the bile broth, followed by transfer to solid nutrient media. From the end of the second week of the disease, a bacteriological method for examining feces and duodenal contents is carried out. Bacteriological examination of bile gives the best results. Starting from the second week of the disease, serological studies are carried out. In the blood of patients with typhoid fever and paratyphoid fever, antibodies to O- and H-antigens appear from 8-10 days of illness, which can be detected using the Vidal agglutination test (RA) and the passive Vi-hemagglutination test. The diagnostic titer in unvaccinated people is considered an agglutination titer of 1: 100 with appropriate clinical indications. In previously vaccinated patients, the H-AT titer of 1:200 is not a reliable diagnostic sign. In such patients, the diagnostic titer should be at least 1:400. An increase in the O-AT titer during the period of illness is a confirmation of an actively ongoing infectious process. By the end of the disease, the O-AT titer decreases, but H-agglutinins accumulate. To detect chronic carriage of typhoid bacteria, RNHA with erythrocyte Vi diagnosticum is used. Diagnostic value has a titer of 1:40 and above. All healthy people with a titer of 1:80 are considered suspicious for carrying typhoid fever.
Treatment. Etiotropic antibiotic therapy, taking into account the sensitivity of the pathogen.
Prevention. For the specific prevention of typhoid fever, a vaccine enriched with Vi-antigen is used; according to epidemic indications, a dry typhoid bacteriophage is prescribed. Non-specific prevention includes: sanitary and bacteriological control of water supply systems, compliance with sanitary and hygienic rules in food preparation, detection of bacteria carriers among workers in food processing units, trade, timely identification and isolation of patients.
The causative agents of Salmonella are numerous Salmonella serovars pathogenic for humans and animals. Most often, these are S. typhimurium, S. enteritidis, S. heidelberg, S. newport, S. dublin, S. choleraesuis. On the territory of Russia, S. enteritidis dominates as the causative agent of salmonellosis.
The main reservoir of infection is farm animals, poultry (waterfowl) and chickens. Ways of transmission: water, alimentary. Transmission factors: meat, milk, eggs, offal.
Salmonella infection usually occurs with a PTI clinic (gastroenteritis). However, it can occur along with the intestinal form and extraintestinal: meningitis, pleurisy, endocarditis, arthritis, abscesses of the liver, spleen, pyelonephritis. This is due to the increase in the number of people with immunodeficiency. With a decrease in the immune status, salmonella can break through the lymphatic barrier of the intestine and enter the bloodstream. Bacteremia develops and extraintestinal lesions become possible.
In recent years, hospital strains have formed, in particular, S. typhimurium. They differ from the rest in clinic, epidemiology, pathogenesis. Hospital strains cause outbreaks of nosocomial infections, mainly among newborns and debilitated children. These strains are characterized by multidrug resistance determined by the R plasmid.
Laboratory diagnostics. The research material is:
2. bowel movements
3. vomit and gastric lavage
4. duodenal contents
Methods of laboratory diagnostics: 1) bacteriological, 2) serological (RNGA).
Treatment. Pathogenetic therapy is used, aimed at normalizing the water-salt metabolism. In generalized forms - etiotropic antibiotic therapy.
Prevention. Non-specific: carrying out veterinary and sanitary measures aimed at preventing the spread of pathogens among farm animals and poultry, as well as observing sanitary and hygienic rules during slaughter at meat processing enterprises, during storage of meat and meat products, cooking, sufficient heat treatment of food products.
Specific prevention of salmonellosis in farm animals and poultry.
Shigella.
The causative agents of dysentery belong to the family Enterobacteriaceae, the genus Shigella, which includes 4 species that differ in biochemical properties and antigenic structure: S. dysenteriae, S. flexneri, S. boydii, S. sonnei.
Shigella are gram-negative, non-motile rods, do not form spores or capsules. On dense nutrient media Ploskirev, Levin, Endo form small smooth, shiny, translucent colonies. On liquid - diffuse turbidity.
Basic biochemical properties: no gas formation during glucose fermentation, no production of hydrogen sulfide, no lactose fermentation within 48 hours.
survival in the external environment. Shigella well tolerate drying, low temperatures, at 60 0 C they die after 30 minutes, at 100 0 C - instantly.
Antigenic structure. Shigella have a somatic O-antigen, depending on the structure of which they are divided into serovars. S. sonnei has a K antigen.
pathogenicity factors.
- plasmid invasion - provides the process of invasion of the colon mucosa;
- toxins - shiga and shiga-like - the toxin enters the bloodstream and, along with the submucosal endothelium, affects the glomeruli of the kidney, as a result, in addition to bloody diarrhea, hemolytic uremic syndrome develops with the development of renal failure;
Epidemiology. Source of infection - sick people and bacteria carriers.
Transfer mechanism . Fecal-oral. Transmission route: S. dysenteriae – contact household, S. flexneri – aquatic, S. sonnei – alimentary.
Shigellosis is ubiquitous. Most often occur in the form of outbreaks of alimentary and water nature.
Clinical manifestations. Shigella, bypassing the stomach and small intestine, attach to colonocyte receptors and penetrate inside with the help of outer membrane protein. Cell death leads to the formation of erosions and ulcers surrounded by perifocal inflammation. Bacterial dysentery is characterized by damage to the mucous membrane and tissue of the large intestine and characteristic symptoms from the gastrointestinal tract: tenesmus, frequent loose stools with impurities of mucus and blood. A complication of shigellosis may be the development of intestinal dysbacteriosis.
Microbiological diagnostics . The material for the study is feces. For sowing, purulent-mucous-blood formations are selected from the middle portion of feces.
The main methods of laboratory diagnostics include: 1) bacteriological; 2) serological (RPGA) - determination of antibodies in the blood serum.
Etiotropic therapy: in the moderate and severe degree of the disease, antibiotics are prescribed, taking into account the sensitivity of the pathogen.
specific prophylaxis. Dysenteric bacteriophage (used in foci of infection).
Escherichia.
The causative agent of escherichiosis belongs to the family Enterobacteriaceae, the genus Escherichia, which includes several species. In human pathology, only the type of E. coli matters.
Escherichia – Gram-negative rods of medium size, motile due to peritrichous flagella. They do not form spores, some strains have a microcapsule. On a nutrient medium, Endo form crimson-colored colonies with a metallic sheen, in a liquid medium they cause diffuse turbidity. They have high enzymatic activity. Breaks down hydrocarbons to form acid and gas (non-gas options available). They ferment lactose (there are lactose-negative variants). The main biochemical properties include: acid and gas production during glucose fermentation; lactose fermentation; inability to form hydrogen sulfide; indole production.
Antigenic structure. E. coli has a complex antigenic structure. It has a somatic O-antigen that determines the serogroup. About 171 varieties are known. O-antigen. Surface K-antigen can be represented by 3 antigens: A, B and L, differing in sensitivity to temperature and chemicals. More than 97 varieties of K-antigen are found in Escherichia. Type-specific H-antigen determines the serovar, of which there are more than 57.
The antigenic structure is indicated by the formulas of the serogroup as O:H, the serovar - O:K:H, for example: O12:B6:H2.
Distinguish conditionally pathogenic And pathogenic(diarrheogenic) Escherichia.
Conditionally pathogenic Escherichia are part of the normal intestinal and vaginal microflora in humans. Diseases that cause UP E. coli are called parenteral escherichiosis. With a decrease in immunological reactivity, Escherichia coli can leave its permanent habitat (intestine) and spread hematogenously or lymphogenously, causing purulent-inflammatory processes of various localization. UP Escherichia coli are detected in cystitis, pyelitis, cholecystitis, urethritis, meningitis, sepsis, pneumonia, tonsillitis, appendicitis, and cause food poisoning. 80% of neonatal meningitis is caused by E. coli, which the newborn becomes infected through the birth canal. The main factor of pathogenicity of E. coli UP is the formation of endotoxin. From opportunistic E. coli, strains multiresistant to antibiotics can be formed due to R-plasmids, which become nosocomial infections.
Pathogenic E.coli are causative agents of intestinal escherichiosis, AII. They are called diarrheal. They are divided into 4 main categories, based on the presence of pathogenicity factors in them.
1. ETCP- enterotoxigenic Escherichia coli - causative agents of cholera-like diseases. Pathogenicity is determined by the production of thermolabile structurally and functionally associated with cholera toxin and thermostable enterotoxin, which disrupt the water-salt metabolism in the intestine, leading to the development of watery diarrhea;
2. EICP- Enteroinvasive Escherichia coli will invade and multiply in the epithelial cells of the mucous wall of the large intestine, causing their destruction. The consequence of this is the development of a dysentery-like disease;
3. EPKP- Enteropathogenic Escherichia coli cause diarrhea in children of the first year of life. They produce Shiga-like toxins, affect the small intestine and cause colienteritis. The disease often occurs as nosocomial infections in neonatal and infant wards.
4. EGCP- can cause bloody diarrhea in people (hemorrhagic colitis) with a subsequent complication in the form of hemolytic uremic syndrome. The source of infection are cattle and sheep. The main route of transmission is alimentary through meat that has undergone insufficient heat treatment. The blind, ascending and transverse colons are affected. Pathogenicity is determined with the production of Shiga-like toxins, the synthesis of hemolysin
Immunity. Parenteral escherichiosis often occurs against the background of immunodeficiency states. Reliable immunity to them is not developed. With intestinal escherichiosis, the development of local immunity mediated by secretory Ig A is observed.
Laboratory diagnostics. The main method is bacteriological.
Specific prophylaxis not developed.
Non-specific prophylaxis comes down to compliance with sanitary and hygienic rules, sanitary control over the source of water supply, food enterprises, food products.
Antibiotics are used for etiotropic therapy.
Vibrio cholerae.
Cholera - especially dangerous quarantine disease caused by Vibrio cholerae, serogroups O1 and O139, characterized by toxic damage to the small intestine, a violation of the water-salt balance and high mortality.
The causative agent of cholera is Vibrionaceae family, Vibrio genus, Vibrio cholerae species.
Vibrio cholerae - a small curved rod, very mobile due to the polar flagellum. Spore, does not form capsules. Grammar negative. Aerobe or facultative anaerobe. It belongs to halophilic microorganisms, therefore it grows well at pH 8.5-9.0. The elective media for it are 1% peptone water and alkaline agar. On peptone water, a film forms already after 6-8 hours of growth; on alkaline agar, after 12 hours, smooth, transparent colonies with a bluish tint are formed.
Biochemical properties: ferments glucose, sucrose to acid, does not ferment arabinose, rhamnose, dulcite. To determine the genus, amino acids are used: arginine, ornithine, lysine.
According to Heiberg, all vibrios are divided into 6 groups in relation to sugars (mannose, sucrose, arabinose). Vibrio cholerae belongs to Heiberg group I and decomposes mannose and sucrose, but does not decompose arabinose.
Antigenic structure. Vibrio cholerae have thermostable O-antigens and thermolabile H-antigens. According to the structure of O-AG, more than 150 serogroups are identified, determined in agglutination reactions. O-antigen Vibrio cholerae O1 consists of three components , depending on the combination of which, three serovars are distinguished: Ogawa, Inaba, Gikoshima. In addition to serovars, two biovars are distinguished within Vibrio cholerae O1: classical and el-tor. They differ in sensitivity to specific bacteriophages, polymyxin, the ability to agglutinate chicken erythrocytes and cause hemolysis.
Pathogenic factors:
1. the ability to adhere and colonize the intestine;
2. the presence of enzymes (mucinase, protease, neuraminidase,
lecitovetylase) - the ability to invade the pathogen;
- production of exoenterotoxin - determines the main clinical manifestation of cholera - profuse diarrhea.
Epidemiology. The source of the infection is a sick person and a carrier. The reservoir of infection is the aquatic environment. The transmission mechanism is fecal-oral. The route of transmission is water, food, less often contact-household. Transmission factors can be fresh and sea water, food products (dairy, vegetables, fruits, hydrobionts).
Clinical manifestations. The disease usually begins with the phenomena of enteritis. Initially, the stool retains a fecal character and smell, but soon takes on the appearance of a whitish watery liquid with floating flakes - rice water. The frequency of stools per day is different, but in about 1/3 of patients from 3 to 10 times. The appearance of vomiting - the transition to the next phase of the disease - cholera gastroenteritis. Vomiting is usually profuse and watery. Due to the loss of a large amount of fluid, the patient becomes dehydrated, cramps appear, especially in the fingers and toes. The skin is cyanotic, cold to the touch. Skin turgor is reduced: the skin easily gathers into a non-expanding fold. The fingers and toes are wrinkled, resembling the hands of a laundress. The patient's voice becomes weak, hoarse, then he speaks only in a whisper, later complete aphonia develops. Body temperature usually drops to subnormal numbers.
Immunity. With recovery, a tense, short-lived immunity arises.
The main method of laboratory diagnostics is bacteriological.
Research material there may be discharge from patients and carriers (feces, vomit, bile), environmental objects (water, food, linen, wastewater, aquatic organisms, washings from environmental objects).
Treatment carried out in two directions: 1) rehydration (replenishment of fluid and electrolyte losses by the introduction of isotonic, apyrogenic saline solutions, as well as plasma-substituting fluids intravenously or orally; 2) antibacterial therapy (broad-spectrum antibiotics: tetracyclines, chloramphenicol, and fluoroquinolones).
Prevention. Non-specific prophylaxis is aimed at 1) disrupting transmission routes (preventing the introduction of infection into the country, sanitary and educational work with the population, providing the population with good-quality drinking water, sewage, food, disinfection); 2) timely identification of the patient and carrier, hospitalization, treatment, quarantine.
Specific prophylaxis- Vaccination. The modern vaccine is a complex preparation consisting of cholerogen toxoid (70%) and chemical O-antigen (30%) of both biovars and serovars. Vaccination ensures the production of vibriocidal antibodies and antitoxins in high titers. Vaccination of the population is carried out according to epidemic indications.
Yersinia.
Enteropathogenic yersinia include pathogens of pseudotuberculosis and intestinal yersiniosis. The causative agents of these diseases are family Enterobacteriaceae, genus Yersinia, types Y. Pseudotuberculosis, And Y. Enterocolitica.
Yersinia- straight gram-negative rods sometimes acquiring a spherical shape. Dispute, capsules do not form. They are immobile at 37 0 С, but below 30 0 С they are mobile due to peritrichous flagella. They grow well on normal nutrient media. On Endo they form ... .., on Yersinia medium Y. Pseudotuberculosis forms dry blue colonies with a scalloped edge, and Y. Enterocolitica blue juicy smooth colonies.
Biochemical activity for Y. Pseudotuberculosis: 1) urease production; 2) fermentation of rhamnose; 3) lack of fermentation of sucrose; 4) no indole production. For Y. Enterocolitica: 1) splitting of urea; 2) fermentation of sucrose; 3) lack of fermentation of rhamnose; 4) production of ornithine decarboxylase.
Antigenic structure. Yersinia have O-, K- and H-antigens. According to the O-antigen within the species, they are divided into serovars.
Pathogenic factors: 1) endotoxin production; 2) protein invasion; 3) thermolabile enterotoxin.
Epidemiology. Intestinal yersiniosis and pseudotuberculosis are sapronose infections. Yersinia is widely distributed in nature. The reservoir of the pathogen in nature is soil, water, plants infected through them. Infected water and plants contribute to the spread of infection among farm animals. The reservoir and source of infection can be cattle, pigs, dogs, cats, birds, rodents (mice, rats). The main ways of transmission are water and alimentary, through water, milk, vegetables.
Clinical manifestations. The pathogenesis and clinic of these diseases are largely similar. Intestinal yersiniosis and pseudotuberculosis are characterized by a polymorphism of clinical manifestations. Having invaded the intestinal mucosa, the pathogen enters the mesenteric lymph nodes, causing mesenteric lymphadenitis - pain in the epigastric region, symptoms of peritoneal irritation that mimic the symptoms of acute appendicitis. In the event of a breakthrough of the lymphatic barrier, bacteremia occurs, as a result of which the microbe spreads throughout the body, causing the formation of granulomas and microabscesses in the macrophage elements of the liver, spleen, lungs, and joints. In this case, the allergization of the body occurs. On days 1-6, a roseolous rash appears. Possible death. With all the variety of clinical manifestations, two clearly defined types of clinical forms of infections can be distinguished: in the first, the disease proceeds as gastroenterocolitis or mesenteric lymphadenitis; in the second, it develops as a result of bacteremia with symptoms of secondary foci and allergic manifestations.
Microbiological diagnostics. Bacteriological and serological research methods are used. The material for bacteriological examination is: feces, cerebrospinal fluid, blood, urine, appendix. For serodiagnosis in RNHA, the material is the patient's blood serum.
Specific prophylaxis is not carried out. Etiotropic therapy: antibiotics, sulfonamides.
Professor KafarskayaL.I.
"infection" (infection)
totalitybiological processes
ongoing
V
macroorganism
at
implementation
V
him
pathogenic
microorganisms, whether
Will this implementation entail
development
explicit
or
hidden
pathological
process
or
it
limited
only
temporary
carriage
or
lengthy
persistence of the pathogen.
Infection
infectiousdisease
consider
How
phenomena,
including
biological
And
social
factors.
So,
transmission mechanisms of infectious
diseases,
their
gravity,
Exodus
conditioned
main
way
social conditions of life
of people.
Infection
Differencesfrom other diseases
Contagiousness (contagiousness)
Cyclicity (periods)
Development of anti-infective
immunity
Incubation
period
pathogenic microorganisms
characteristicproperties
pathogenic
microorganisms
are
specificity
(ability
call
certain infectious disease
after entering the body)
organotropism
(ability
preferably
hit
certain organs or tissues). Place
penetration
pathogen
called the entrance gate.
How
the rule is - fabrics devoid of
physiological
protection
against
a specific type of microorganism
place
his
penetration
V
macroorganism or entry gate
infections.
Cylindrical epithelium for gonococci.
Staphylococci,
streptococci
may
penetrate in several ways
The infectious dose of the pathogen
infectiousdose of pathogen
minimal amount of microbes
cells,
able
call
infectious
process. Value
infectious dose depends on
virulent properties of the pathogen.
The higher the virulence, the lower
infectious dose.
infectious dose
Forhighly virulent
pathogen
Yersinia pestis (plague) enough a few
bacterial cells.
Shigella dysenteriae - dozens of cells.
For some pathogens, thousands to hundreds
thousand - cholera
infectious
dose
low-virulence
strains is equal to 105-106 microbial cells.
1 period - Incubation - from the moment
infection before the onset of clinical
symptoms
Localization of the pathogen - in the input
gates of infection and/or l/nodes
Periods of infectious disease
4thperiod - Outcome of the disease
(outcome) Reconvalescence
Transition to the chronic form
Formation of bacteriocarrier
Death
Periods of infectious disease
2ndperiod - prodromal
(prodrome) is
manifestation
“general
symptoms”discomfort, fatigue, chills.
Clinically, it is intoxication.
Localization of the pathogen penetrates into the blood, lymph,
secretion of toxins occurs
appears
activity
factors
congenital
immunity IN
currently there is a shift from
traditional concept of bacteria
as strictly unicellular organisms to
understanding of microbial communities
as integral structures regulating
their behavioral responses
from changing living conditions.
Enough data has now been accumulated on
mechanisms,
through
which
carried out
intrapopulation,
interstrain and interspecies contacts in
microorganisms,
A
Also
their
interaction with the host
Ways of penetration of the pathogen into the macroorganism
Factors of pathogenicity of microorganisms
Adhesion and colonization factorsInvasion factors
Antiphagocytic factors
Factors that impair immune
protection
Toxic factors Adhesion
going on
on
surfaces
mucous membranes of various organs and
systems.
Adhesion begins as a reversible process,
then goes into irreversible
On
forces involved in the first stages
electrostatic
interactions,
hydrophobic bonds, active mobility
microorganisms.
The presence of flagella allows effective
approach the surface of the cell
Flagella promote approach to the cell surface
Vibrio cholerae
Adhesion.
Onhost cell
there are receptors for a variety of molecules (glycolipids, mannose
residues, proteoglycans).
Receptors for adhesins of gram (+) bacteria more often
of all are fibronectin and intercellular proteins
matrix.
Ligand-receptor
interaction
highly specific process, while the cell
host is an active participant.
Pathogens activate transduction signaling pathways,
further activation of receptors occurs.
Adhesion factors
Adhesionends
ligand-receptor
interaction. This is a highly specific process.
In which adhesins are complementary to cell receptors.
Microbial tropism is associated with the specificity of adhesion -
the ability of microorganisms to infect certain
organs and tissues.
(Gonococci
–
cylindrical
epithelium
mucous
urethral tract or conjunctiva of the eye).
The presence of a capsule or mucus may promote adhesion.
Some
bacteria can interfere with motor
ciliary activity of the ciliary epithelium of the respiratory
pathways (synthesis of ciliotoxic/ciliostatic molecules in
Bordetella pertussis, pneumococci, Pseudomonas Colonization of the tracheal epithelium by Bordetella
(cells without cilia free from bacteria)
pertussis
Adhesion factors
AtAdhesion factors
gram-negative bacteria function
recognition and attachment of bacteria more often
carry out pili or fimbriae. They are shorter
and thinner flagella. Their length can reach
10 nm (sometimes up to 2 µm). Most types
fimbria, encoded by chromosomal genes,
rarely plasmids.
Pili - protein structures consisting of
pilin protein, to which they can attach
carbohydrate and protein components.
Behind
irreversible
adhesion
meet
highly specific
structures,
glycoproteins and glycolipids.
fimbriae in gonococci. Quantity 100-500. Consist of pilin.
In Gram-negative bacteriafimbria serve as adhesion factors
(fimbrial adhesins) or proteins
outer membrane. (A) Electron micrograph of negatively stained E coli. Curved flagella are shown
and numerous short thin and more rigid hair-like structures, pili. (B)
Long F-pills can be distinguished from short regular (plain) pili by cell mixing
E coli with specific bacteriophages capable of selectively binding to F pili
Drank E.coli
Adhesins
Athimbrialadhesins
–
filamentous haemagglutinin in Bordetella
pertussis responsible for attachment to
ciliated epithelium of the respiratory tract.
Fimbrial adhesins provide more
effective adhesion than afimbriae.
They
turn out
localized
on
long thin stem, which makes them easier
contact with the receptor and probably allows
overcome
barrier
"normal"
microflora and other protective mechanisms.
Adhesion
Colonizationtracheal epithelium
Bordetella
pertussis
(cells without
cilia are free
from bacteria)
Adhesion factors in Gram-positive bacteria
Cellular proteinsTeichoic acids
walls
Lipo-teichoic
acids
Peptidoglycan
CPM
Teichoic and lipoteichoic acids,
outer cell wall proteins
adhesion factors
gram-positive
bacteria Figure 2-9. Structure of teichoic acids (A) Ribitol teichoic acid with repeating fragments linked by 1,5-phosphodiester bonds of D-ribitol and D-alanyl ester in position 2 and glycosyl radicals (R) in position 4.
The glycosyl groups can be N-acetylglucosaminyl (or) as in S aureus or -glucosyl as in B subtilis W23. (B)
Teichoic acid glycerol with 1,3-phosphodiester bonds between repeating glycerol subunits
(1,2-bonds in some species
Adhesion
In Gram-positive bacteria,Teichoic and lipoteichoic acids.
Fibronectin binding proteins
(staphylococci, streptococci).
M-protein in group A streptococci.
Streptococcus pyogenes. cell surface fibrils
M protein and fimbriae of Group A streptococci - adhesion and protection against phagocytosis
M protein and fimbriae of Group A streptococcifrom phagocytosis
– adhesion and protection Uropathogenic
Escherichia
express
two
kind
villi:
P-villi
And
type I villi, bind
with different receptors
Adhesion serves as a signal to
launch
cascade
difficult
reactions in both bacteria and
macroorganism. By binding
R-piley
intensifies
iron absorption
Villi
Type I
connection
With
released by the receptor
ceramides
– activators
serine/threonine kinases,
stimulating the synthesis of a number
cytokines (IL 1, IL 6, IL 8). invasion-spread
his cells.
Invasion
Ateukaryotic receptor invasion
cells are their membrane molecules,
whose main function is intercellular
interactions.
Invasive
enterobacteria
V
quality
receptors
use
integrins
eukaryotic cells.
Listeria is used as a receptor
cadherin. These epithelial cell molecules
play a major role in maintaining the structure
fabrics,
providing
physical
contact
eukaryotic cells.
Invasion
Adhesion is a signal for protein synthesis(IpaB, IpaC and IpaD) performing
functions of invaders. Their transport
inside
eukaryotic
cells
carried out by a special system
secretion related to type III.
These proteins cause
intense polymerization of actin
inside the M cell, leading to
formation
pseudopodia,
covering
bacterial
cells, and vacuoles.
Bacterium
"forces"
epithelium seize itself
cage Yersinia
spp., Salmonella spp. And
Shigella
spp.
carry out
invasion
intestinal
epithelium,
the main gates are
M cells.
One of the main functions of M cells
is
transport
macromolecules and larger
particles from the intestinal lumen
submucosal areas
Invasion
Shigellamigrates to the submucosa
layer,
V
region
lymphoid
follicles
Where
exposed
phagocytosis
mononuclear
phagocytes.
Shigella
cause
apoptosis
phagocytes,
again
released into the submucosa
and can penetrate intact
enterocytes through their basolateral
membranes. Mechanism of bacterial invasion in some Gram-negative (D) Scanning electron micrograph of enteropathogenic E.
coli attached to support-like cell outgrowths on
surface of HeLa cells. (E) Environment of Shigella flexneri
cytoplasmic outgrowths of cells (like ripples), during
bacterial invasion of HeLa epithelial cells. WITH
biofilm formation
starts
development of any infection.
Biofilm is a thin layer of microorganisms
the polymers they secrete, which
adhered
To
organic
or
inorganic surface.
Microorganisms included in
Biofilms exist in two forms:
fixed to the surface, and planktonic,
free-floating, being a substrate
spread of infection from its primary
locus.
The composition of the surface shell and matrix
biofilms include proteins, polysaccharides,
lipids and nucleic acids (DNA and RNA)
Biofilms
Thisbasic phenotype of almost all bacteria in
natural habitats, as in the outer
environment, and in the human body in pathology.
Biofilms provide protection against factors
environment and may include microorganisms
different kingdoms (for example, bacteria and fungi).
Among the pathogens that form biolens,
have the greatest clinical significance.
P. aeruginosa, S. aureus, K. pneumoniae,
Coagulasae-negative
staphylococcus(CNS), Enterococcus
spp., Candida spp.
Biofilms
Existencebacteria in the form of biofilms
enhances its defense against phagocytosis,
ultraviolet radiation, viruses and
dehydration, as well as from antibiotics
(to maintain concentrations of antibiotics in
100-1000 times more than overwhelming
planktonic cells) and factors of immune
macroorganism protection. Therapeutic
effects on biofilms can be
aimed at the mechanisms of initial
adhesion of bacteria to the surface
Adhesion of microorganisms to implantable devices.
Neitherone used to create
implantable device materials are not
is
biologically
inert.
Microorganisms
get in touch
With
their
surfaces
V
result
non-specific
adhesion,
are happening
deposition of macroorganism proteins, more often
total fibrin, and film formation, in
which contains molecules
are receptors for adhesins
microorganisms, there are no factors
anti-adhesion.
Formation of biofilms
Formation of biofilmsATTACHMENT
COLONIZATION
BREEDING
SURFACE
- Colonization (environmental objects, valves
-hearts, tooth enamel and more, catheters, ....)
- Resistance to phagocytosis
- Antibiotic resistance
Invasion factors
Invasion - penetration of the pathogen throughmucosal and connective tissue barriers
Aggression is the suppression of the natural
resistance and adaptive immunity.
They act together.
Many are invasive and aggressive
surface structures of a bacterial cell
(flagella, surface proteins, lipopolysaccharide
cell wall of Gram-bacteria), as well as enzymes
secreted by bacteria
Invasion factors
invasion-spreadmicroorganisms in intercellular
body tissue spaces
host and their penetration
his cells.
Distribution factors
-row
enzymes
produced
bacterial
cells.
Most of them are hydrolases.
Invasion factors
Hyaluronidase–
depolymerizes
hyaluronic acid, high polymer
compound consisting of residues N acetylglucosamine and D - glucuronic
acids.
The glycosidic bond is broken.
Hyaluronic acid - the main component
connective tissue found in
cellular
membranes
intercellular
substance, the viscosity decreases.
Produced by staphylococci, streptococci,
clostridia, vibrio cholerae.
Invasion factors
Neuraminidase - hydrolyzes glycosidic bonds intoglycoproteins, gangliosides, splits off from them
residues of sialic (neuraminic acids),
which consist of residues of D-mannosamine and
pyruvic acid.
Sialic acids are part of mucin,
mucous secretions, gives them viscosity,
hinders the progress of the microorganism
epitheliocytes.
Are on the surface
tissues, leukocytes.
Neuraminidase - destroys the mucin barrier,
reduced activity of phagocytosis
Work out
staphylococci,
streptococci,
cholera vibrios, clostridia.
Factors of invasion and aggression
Lecithinase- hydrolyzes lecithin
(phosphoglyceride
phosphatidylcholine)
basic
component
membranes
mammals,
destroys
lipids
cell membranes.
Produced by staphylococci, clostridia,
bacilli, listeria.
Lecithinase activity
proteolytic enzymes.
Basictarget of proteolytic enzymes,
formed by bacteria are signal and
immune defense effector molecules
Coagulase catalyzes the hydrolysis of peptide
connections.
Fibrinolysin is a hydrolase
This enzyme is able to dissolve fibrin,
Contributes to the generalization of infection.
Proteases - elastase (elastin of lung tissue)
gelatinase.
Collagenases – tendon collagen (contains
glycine). IgA proteases - hydrolysis of secretory
immunoglobulins
Neisseria meningitidis
serine protease
Haemophilus spp. serine protease
Streptococcus spp.
Zinc protease
Enzymes.
DNAasehydrolysis of DNA molecules
phosphodiester bonds the breakdown of DNA and RNA
molecules
on
oligonucleotides
And
mononucleotides
the viscosity of the medium decreases, contributes to
reproduction
microorganisms.
Staphylococcus, streptococcus.
Plasmocoagulase - transfers soluble
fibrinogen to fibrin, causes clotting
blood plasma. Produced in inactive
condition.
Produced by Staphylococcus aureus
DNA test.
Plasma coagulase test
Enzymes
Ureasebreakdown of urea, ammonia causes
alkalization of the medium, direct toxic effect.
Toxic to the central nervous system.
Suppresses
cellular
breath.
going on
restorative
amination
ketoglutaric acid in mitochondria
glutamic acid, which leads to the removal of ketoglutaric acid from the tricarboxylic acid cycle
acids, suppression
cellular
breathing.
Brucella and Helicobacter are produced. Antiphagocytic factors
Stages of phagocytosis
Antiphagocytic factors
Havesurface localization.
capsules, capsule-like structures
are not vital to
bacterial cell
have a macromolecular structure
hydrophilic
Antiphagocytic factors
Protectionfrom phagocytosis can occur on
various stages of the process:
At the stage of recognition-absorption
Capsules, capsule-like polysaccharide
M-protein
streptococci,
K antigen
gram-negative bacteria.
Staphylococcus aureus has an A-protein and an enzyme
plasmacoagulase, under the action of which around
cells
formed
fibrinous
case,
obstructive
recognition
bacteria
phagocytes. Number (figure) 11. Negative staining of Streptococcus pyogenes by electron microscopy (28,000X). Halo
around the chain of cells - a capsule of hyaluronic acid, which surrounds the bacteria from the outside. It may also be
a septum was seen between a dividing pair of cells. Bacillus anthracis colonies. Growth of mucoid or mucoid bacterial colonies - usually indicative of production
capsules. In the case of B. anthracis, the capsule consists of poly-D-glutamine. The capsule is an essential determinant of pathogenicity
bacteria. In the early stages of colonization and infection, the capsule protects bacteria from antibacterial activity.
immune and phagocytic systems. Bacterial
capsules,
contrasted
Chinese
ink,
considered in
light microscope.
This
true
capsule,
isolated layer
polysaccharides,
around
cells.
Sometimes
bacterial
cells
surrounded
more messy
polysaccharide
matrix
called slime
or biofilm.
Antiphagocytic factors
Capsule – Burri-Gins method MicroorganismThe nature of the capsule
Capsule polymer subunits
Acetobacter xylinum
Cellulose
Glucose
Azotobacter vinelandii
Polyuronide
Glucuronic and mannuronic
acids
bac. anthracis
Polypeptide
D-Glutamic acid
bac. licheniformis
Separate species from the family
Enterobacteriacceae
Many types of complex
polysaccharides, colanic
acid
Complex polysaccharide
galactose, glucose,
glucuronic acid, PVC,
fucose
and etc.
Galactose
galacturonic
Leuconostoc mesenteroides
Glucan (dextran)
acid, fucose
Glucose
Pseudomonas aerugenosa
Polyuronide or others
polysaccharides
Hyaluronic acid
Klebsiella pneumoniae
Streptococcus haemoliticus
Streptococcus pyogenes
Sterptococcus pneumoniae
Many types of complex polymers,
for example: Type I
Type II
Sterptococcus salivarius
Fructan (levan)
N. meningitidis
Polysaccharide
H. influenzae
Polysaccharide
Glucuronic. mannuronic
acid
N-acetylglucosamine,
glucuronic acid
3-Deoxygalactose,
galacturonic acid,
glucose, glucuronic acid
Fructose
N-acetylmannosamine polymer
phosphate (group A); polymer
sialic acid (group B and
WITH)
Polyribose Phosphate
Antiphagocytic factors
Survivalmicrobial cells after absorption
phagocyte.
Prevention of fusion of phagosome with lysosome
cord factor of mycobacteria
Suppression of acidification processes in the phagolysosome
leads to disruption of the action of lysosomal
enzymes, genes are localized in the islet
pathogenicity (SpI2), are expressed only after
entry of microorganisms into phagocytes.
Destruction of the phagosome membrane prior to fusion with
lysosome - listeria, rickettsia. In formation
pores
V
membrane
phagosomes
participate
listeriolysin and phospholipases.
incomplete phagocytosis
Invasion of non-phagocytic cells
Activeinvasion of cells not related to
phagocytes, especially epithelial:
micro-organisms inside these cells
exposed to any adverse
influences.
described
strategy
Salmonella and Shigella are used.
Staphylococci, pyogenic streptococci and
mycobacteria, penetrate into phagocytes,
using
receptors
To
complement.
Phagocytosis,
mediated
these
receptors, does not lead to pronounced
activation of bactericidal systems of phagocytes.
Evasion of the immune response
Variabilityantigenic properties
Antigenic mimicry
Formation of L-shapes
Screening antigenic
determinant with capsules Streptococcus sp.
Pseudomonas
Pseudomonas aeruginosa
Bacterial toxins
Provide directpathological action
Exotoxins (protein toxins) -
stand out predominantly in
environment.
Endotoxins - associated with the structure
bacterial cell
Bacterial toxins
Characteristic properties of proteintoxins
Toxicity
Specificity
Thermolability
Immunogenic - form toxoids
Bacterial toxins
Simple - polypeptide chainComplex - several linked polypeptides
chains connected to each other.
Simple toxins are produced in the inactive
form (protoxin) - activated by proteases.
The biological meaning of activation is education
bifunctional system of subunit A and B.
B-transport and receptor function
A- has enzymatic properties,
has a specific effect
Classification by mechanism of action
Inhibit protein synthesis - cytotoxinsdamage
cellular
membranes -
membrane toxins
Violate
transfer
signals
–
functional blockers
toxins
proteasesfunctional
blockers
Superantigen toxins - immunotoxins
Mechanism of action of toxins Disrupting protein synthesis
Diphtheria toxin is simple. PossessesRibosyl transferase
activity,
transports ADF-ribose
On the target elongation factor, transferase-2,
disrupt the elongation of polypeptide chains
Toxins that interfere with protein synthesis
Shiga toxin- Subunit A, which has
enzymatic activity,
as N-glycosidase, cleaving off a single
adenine residue from the 28S ribosomal
RNA.
Causes enzymatic damage
28s ribosomal RNA of epithelial cells
thick
intestines,
violated
functioning
ribosome,
factors
elongation
Not
may
contact
With
ribosomes disrupt protein synthesis
the cell dies.
Pore-forming toxins.
Bacterialtoxins that function
through
inserts
V
plasmatic
host membrane and forming in it
transmembrane pores leading the cell to
lysis.
Toxins that damage cell membranes.
Pore-forming hemolysins andleukocidin.
Can damage monocytes, platelets.
Staphylococcal alpha toxin
Violating the integrity of the membranes
cells using an enzymatic
hydrolysis of phospholipids -
C. perfringens phospholipase
Toxins that damage cells
membranes.
Types of hemolysis on blood agar
group A β-hemolytic streptococci (Streptococcus pyogenes)
Functional blockers (activators of metabolic pathways of second messengers
Violating the function of adanylate cyclase -cholera
toxin is a complex toxin
subunits A and 5 subunits B, in the form of a ring
A1
has
glycohydrolase
And
ribosyl transferase activity.
ADF-ribose is transferred to GTP
Activated
adenylate cyclase,
leads
To
excessive accumulation of cAMP
The transport of electrolytes is impaired
An excess in the intestine leads to an increase
osmotic pressure in the intestine, from the cell
water is secreted
cholera toxin
C.botulinum neurotoxins (BoNT serotypes A vG) and C.tetani proteases
neurotoxinssynthesized
V
form
inactive polypeptides with molecular
weighing up to 150 kDa. Each active molecule
neurotoxin consists of a heavy (100 kDa) and a light
(50 kDa) chains connected by a single
bisulfide bond. The heavy chain contains two
domain: site responsible for translocation
toxin at the N-terminus, and a region at the C-terminus
regulating the binding of toxin to the cell. Lungs
chains
contain
zinc-binding
sequences to carry out protease
activity of the toxin, dependent on zinc ions.
Cellular targets - a group of proteins necessary for the connection of synaptic vesicles with presynaptic plasma membranes with
Tetanospasmin - tetanus toxin, simple toxinActivation requires proteolytic
cleavage into light and heavy chains
Cellular targets
- a group of proteins
necessary for
connections
synaptic
bubbles with
presynaptic
plasmatic
membranes with
subsequent
release
neurotransmitters
Neurotoxin
tetanusthe toxin affects two types
neurons. It binds to receptors
presynaptic
membranes
motor
neurons,
then using reverse
vesicular transport moves to
spinal cord, where it is introduced into the inhibitory and
intercalary neurons.
Cleavage of the vesicle-associated
membrane protein and synaptobrevin
these neurons leads to disruption
release
glycine
And
gamma-aminobutyric acid, which are capable of
stop muscle contraction
proteolytic toxins neurotoxins
Possessesprotease
activity,
destroys
protein
synaptobrevin,
blocks the braking system - convulsions
Botulinum toxin
–
valid
How
endoprotease, destroys target proteins,
violates
secretion
acetylcholine,
blockade of motor neurons, flaccid paralysis.
Toxins-superantigens, activators of the immune response
Immunostimulatingthe potential of toxins is
consequence of their ability to link different
regions of proteins of the main complex
type II histocompatibility expressed on
surfaces of antigen-presenting cells; and Vbeta elements on the T-cell receptor.
Linking TSST-1 to Vbeta2 results in massive
proliferation of more than 20% of peripheral T cells.
The consequence of T-cell expansion is
massive release of cytokines
Cytokines cause hypotension, high
fever and diffuse erythematous rash
Toxins-superantigens
Endotoxin
Difficultlipopolysaccharide
complex,
contained
V
cellular
wall
Gram-negative bacteria and
released into the environment
at
lysis
bacteria.
LPS
includes
3
covalently bound component:
Endotoxins
Lipid ACentral
oligosaccharide
O antigen
Endotoxins
Endotoxinsdo not possess
specificity
thermostable, less
toxic, weak
immunogenicity.
 “Infection” (infection) is a set of biological processes occurring in a macroorganism when pathogenic microorganisms are introduced into it, regardless of whether this introduction will entail the development of an overt or latent pathological process or whether it will be limited only to temporary carriage or long-term persistence of the pathogen.
“Infection” (infection) is a set of biological processes occurring in a macroorganism when pathogenic microorganisms are introduced into it, regardless of whether this introduction will entail the development of an overt or latent pathological process or whether it will be limited only to temporary carriage or long-term persistence of the pathogen.
 Infection Infectious diseases are considered as phenomena involving biological and social factors. Thus, the mechanisms of transmission of infectious diseases, their severity, outcome are mainly determined by the social conditions of people's lives.
Infection Infectious diseases are considered as phenomena involving biological and social factors. Thus, the mechanisms of transmission of infectious diseases, their severity, outcome are mainly determined by the social conditions of people's lives.

 Pathogenic microorganisms The characteristic properties of pathogenic microorganisms are specificity (the ability to cause a certain infectious disease after entering the body) and organotropism (the ability to preferentially affect certain organs or tissues).
Pathogenic microorganisms The characteristic properties of pathogenic microorganisms are specificity (the ability to cause a certain infectious disease after entering the body) and organotropism (the ability to preferentially affect certain organs or tissues).
 The place of penetration of the pathogen is called the entrance gate. As a rule, these tissues, deprived of physiological protection against a particular type of microorganisms, serve as a place for its penetration into a macroorganism or an entrance gate for infection. Cylindrical epithelium for gonococci. Staphylococci, streptococci can penetrate in several ways
The place of penetration of the pathogen is called the entrance gate. As a rule, these tissues, deprived of physiological protection against a particular type of microorganisms, serve as a place for its penetration into a macroorganism or an entrance gate for infection. Cylindrical epithelium for gonococci. Staphylococci, streptococci can penetrate in several ways
 The infectious dose of the pathogen is the minimum number of microbial cells that can cause an infectious process. The value of the infectious dose depends on the virulent properties of the pathogen. The higher the virulence, the lower the infectious dose.
The infectious dose of the pathogen is the minimum number of microbial cells that can cause an infectious process. The value of the infectious dose depends on the virulent properties of the pathogen. The higher the virulence, the lower the infectious dose.
 Infectious dose A few bacterial cells are sufficient for the highly virulent Yersinia pestis (plague) pathogen. Shigella dysenteriae - dozens of cells. For some pathogens - thousands to hundreds of thousands - cholera The infectious dose of low-virulence strains is 105 -106 microbial cells.
Infectious dose A few bacterial cells are sufficient for the highly virulent Yersinia pestis (plague) pathogen. Shigella dysenteriae - dozens of cells. For some pathogens - thousands to hundreds of thousands - cholera The infectious dose of low-virulence strains is 105 -106 microbial cells.
 Periods of an infectious disease 1 period - Incubation - from the moment of infection to the onset of clinical symptoms. Localization of the pathogen - at the entrance gate of the infection and / or l / nodes
Periods of an infectious disease 1 period - Incubation - from the moment of infection to the onset of clinical symptoms. Localization of the pathogen - at the entrance gate of the infection and / or l / nodes
 Periods of an infectious disease 4th period - The outcome of the disease (outcome) - Reconvalescence Transition to a chronic form Formation of a bacteriocarrier Lethal outcome
Periods of an infectious disease 4th period - The outcome of the disease (outcome) - Reconvalescence Transition to a chronic form Formation of a bacteriocarrier Lethal outcome
 Periods of an infectious disease 2nd period - Prodrome (prodrome) is a manifestation of "general symptoms" - discomfort, fatigue, chills. Clinically, it is intoxication. Localization of the pathogen - penetrates into the blood, lymph, secretion of toxins occurs, the activity of innate immunity factors is manifested
Periods of an infectious disease 2nd period - Prodrome (prodrome) is a manifestation of "general symptoms" - discomfort, fatigue, chills. Clinically, it is intoxication. Localization of the pathogen - penetrates into the blood, lymph, secretion of toxins occurs, the activity of innate immunity factors is manifested
 Currently, there is a transition from the traditional idea of bacteria as strictly unicellular organisms to the idea of microbial communities as integral structures that regulate their behavioral responses depending on changes in environmental conditions. Today, enough data has been accumulated on the mechanisms by which intrapopulation, interstrain and interspecies contacts are carried out in microorganisms, as well as their interaction with the host organism.
Currently, there is a transition from the traditional idea of bacteria as strictly unicellular organisms to the idea of microbial communities as integral structures that regulate their behavioral responses depending on changes in environmental conditions. Today, enough data has been accumulated on the mechanisms by which intrapopulation, interstrain and interspecies contacts are carried out in microorganisms, as well as their interaction with the host organism.
 Ways of penetration of the pathogen into the macroorganism Through the mucous membranes There are factors of natural protection Overcoming this protection, microorganisms attach to the cells of the epithelium and colonize it, Then they penetrate into the lymphatic system, blood, tissues of internal organs Through microtraumas of the skin - Possibly transmissively. The causative agent, bypassing the natural barriers of the skin and mucous membranes, penetrates into the lymphatic system and into the blood
Ways of penetration of the pathogen into the macroorganism Through the mucous membranes There are factors of natural protection Overcoming this protection, microorganisms attach to the cells of the epithelium and colonize it, Then they penetrate into the lymphatic system, blood, tissues of internal organs Through microtraumas of the skin - Possibly transmissively. The causative agent, bypassing the natural barriers of the skin and mucous membranes, penetrates into the lymphatic system and into the blood
 Microbial pathogenicity factors Adhesion and colonization factors Invasion factors Antiphagocytic factors Factors that impair immune defense Toxic factors
Microbial pathogenicity factors Adhesion and colonization factors Invasion factors Antiphagocytic factors Factors that impair immune defense Toxic factors
 Adhesion factors Adhesion occurs on the surface of the mucous membranes of various organs and systems. Adhesion begins as a reversible process, then turns into an irreversible one. At the first stages, electrostatic interaction forces, hydrophobic bonds, and active mobility of microorganisms are involved. The presence of flagella allows you to effectively approach the surface of the cell
Adhesion factors Adhesion occurs on the surface of the mucous membranes of various organs and systems. Adhesion begins as a reversible process, then turns into an irreversible one. At the first stages, electrostatic interaction forces, hydrophobic bonds, and active mobility of microorganisms are involved. The presence of flagella allows you to effectively approach the surface of the cell


 Adhesion. The host cell has receptors for various molecules (glycolipids, mannose residues, proteoglycans). The most common receptors for gram (+) bacteria adhesins are fibronectin and extracellular matrix proteins. Ligand-receptor interaction is a highly specific process, with the host cell being an active participant. Pathogens activate transduction signaling pathways, followed by activation of receptors.
Adhesion. The host cell has receptors for various molecules (glycolipids, mannose residues, proteoglycans). The most common receptors for gram (+) bacteria adhesins are fibronectin and extracellular matrix proteins. Ligand-receptor interaction is a highly specific process, with the host cell being an active participant. Pathogens activate transduction signaling pathways, followed by activation of receptors.
 Adhesion factors Adhesion is completed by ligand-receptor interaction. This is a highly specific process in which adhesins are complementary to cell receptors. The specificity of adhesion is associated with microbial tropism - the ability of microorganisms to infect certain organs and tissues. (Gonococci - cylindrical epithelium of the mucous membrane of the urethral tract or conjunctiva of the eye). The presence of a capsule or mucus may promote adhesion. Some bacteria can disrupt the motor activity of the cilia of the ciliary epithelium of the respiratory tract (synthesis of ciliotoxic / ciliostatic molecules in Bordetella pertussis, pneumococci, Pseudomonas
Adhesion factors Adhesion is completed by ligand-receptor interaction. This is a highly specific process in which adhesins are complementary to cell receptors. The specificity of adhesion is associated with microbial tropism - the ability of microorganisms to infect certain organs and tissues. (Gonococci - cylindrical epithelium of the mucous membrane of the urethral tract or conjunctiva of the eye). The presence of a capsule or mucus may promote adhesion. Some bacteria can disrupt the motor activity of the cilia of the ciliary epithelium of the respiratory tract (synthesis of ciliotoxic / ciliostatic molecules in Bordetella pertussis, pneumococci, Pseudomonas

 Adhesion factors In gram-negative bacteria, the function of recognition and attachment of bacteria is more often carried out by pili fimbriae. They are shorter and thinner than flagella. Their length can reach 10 nm (sometimes up to 2 microns). Most types of fimbriae are encoded by chromosomal genes, less often by plasmids. Pili are protein structures consisting of pilin protein, to which carbohydrate and protein components can be attached. Highly specific structures, glycoproteins and glycolipids are responsible for irreversible adhesion.
Adhesion factors In gram-negative bacteria, the function of recognition and attachment of bacteria is more often carried out by pili fimbriae. They are shorter and thinner than flagella. Their length can reach 10 nm (sometimes up to 2 microns). Most types of fimbriae are encoded by chromosomal genes, less often by plasmids. Pili are protein structures consisting of pilin protein, to which carbohydrate and protein components can be attached. Highly specific structures, glycoproteins and glycolipids are responsible for irreversible adhesion.
 fimbriae in gonococci. Quantity 100 -500. Consist of pilin. In Gram-negative bacteria, pili (fimbriae adhesins) or outer membrane proteins serve as adhesion factors.
fimbriae in gonococci. Quantity 100 -500. Consist of pilin. In Gram-negative bacteria, pili (fimbriae adhesins) or outer membrane proteins serve as adhesion factors.
 (A) Electron micrograph of negatively stained E coli. Curved flagella and numerous short thin and more rigid hair-like structures are shown, pili. (B) Long F pili can be distinguished from short normal (simple) pili by mixing E coli cells with specific bacteriophages capable of selectively binding to F pili.
(A) Electron micrograph of negatively stained E coli. Curved flagella and numerous short thin and more rigid hair-like structures are shown, pili. (B) Long F pili can be distinguished from short normal (simple) pili by mixing E coli cells with specific bacteriophages capable of selectively binding to F pili.

 Adhesins Athimbrial adhesins are filamentous haemagglutinins in Bordetella pertussis responsible for attachment to the ciliated airway epithelium. Fimbrial adhesins provide more effective adhesion than afimbriae. They are localized on a long thin stalk, which facilitates their contact with the receptor and, probably, allows them to overcome the barrier of the "normal" microflora and other protective mechanisms.
Adhesins Athimbrial adhesins are filamentous haemagglutinins in Bordetella pertussis responsible for attachment to the ciliated airway epithelium. Fimbrial adhesins provide more effective adhesion than afimbriae. They are localized on a long thin stalk, which facilitates their contact with the receptor and, probably, allows them to overcome the barrier of the "normal" microflora and other protective mechanisms.

 Cell wall proteins Teichoic acids Lipo-teichoic acids Peptidoglycan CPM Teichoic and lipoteichoic acids, outer cell wall proteins Adhesion factors in Gram-positive bacteria
Cell wall proteins Teichoic acids Lipo-teichoic acids Peptidoglycan CPM Teichoic and lipoteichoic acids, outer cell wall proteins Adhesion factors in Gram-positive bacteria
 Adhesion In gram-positive bacteria - teichoic and lipoteichoic acids. Fibronectin binding proteins (staphylococci, streptococci). M-protein in group A streptococci.
Adhesion In gram-positive bacteria - teichoic and lipoteichoic acids. Fibronectin binding proteins (staphylococci, streptococci). M-protein in group A streptococci.


 Uropathogenic Escherichia express two types of villi: P-villi and type I villi, bind to different receptors. Adhesion serves as a signal to launch a cascade of complex reactions both in bacteria and in the macroorganism. The binding of P-piles enhances the absorption of iron Villi type I bound. with the receptor are released, ceramides are activators of serine/threonine kinases that stimulate the synthesis of a number of cytokines (IL 1, IL 6, IL 8).
Uropathogenic Escherichia express two types of villi: P-villi and type I villi, bind to different receptors. Adhesion serves as a signal to launch a cascade of complex reactions both in bacteria and in the macroorganism. The binding of P-piles enhances the absorption of iron Villi type I bound. with the receptor are released, ceramides are activators of serine/threonine kinases that stimulate the synthesis of a number of cytokines (IL 1, IL 6, IL 8).
 Invasion - the spread of microorganisms in the intercellular spaces of the tissues of the host organism and their penetration into its cells.
Invasion - the spread of microorganisms in the intercellular spaces of the tissues of the host organism and their penetration into its cells.
 Invasion During invasion, the receptors of eukaryotic cells are their membrane molecules, the main function of which is intercellular interactions. Invasive enterobacteria use integrins of eukaryotic cells as receptors. Listeria use cadherin as a receptor. These epithelial cell molecules play a major role in maintaining tissue structure by providing physical contact between eukaryotic cells.
Invasion During invasion, the receptors of eukaryotic cells are their membrane molecules, the main function of which is intercellular interactions. Invasive enterobacteria use integrins of eukaryotic cells as receptors. Listeria use cadherin as a receptor. These epithelial cell molecules play a major role in maintaining tissue structure by providing physical contact between eukaryotic cells.
 Invasion Adhesion is a signal for the synthesis of proteins (Ipa. B, Ipa. C and Ipa. D) that perform the functions of invasins. Their transport into the eukaryotic cell is carried out by a special type III secretion system. These proteins cause intense polymerization of actin inside the M-cell, leading to the formation of pseudopodia, covering the bacterial cell, and vacuoles. The bacterium "forces" the epithelial cell to capture itself
Invasion Adhesion is a signal for the synthesis of proteins (Ipa. B, Ipa. C and Ipa. D) that perform the functions of invasins. Their transport into the eukaryotic cell is carried out by a special type III secretion system. These proteins cause intense polymerization of actin inside the M-cell, leading to the formation of pseudopodia, covering the bacterial cell, and vacuoles. The bacterium "forces" the epithelial cell to capture itself
 Yersinia spp. , Salmonella spp. and Shigella spp. carry out invasion of the intestinal epithelium, the main "gates" are M-cells. One of the main functions of M cells is the transport of macromolecules and larger particles from the intestinal lumen to the region of the submucosal layer.
Yersinia spp. , Salmonella spp. and Shigella spp. carry out invasion of the intestinal epithelium, the main "gates" are M-cells. One of the main functions of M cells is the transport of macromolecules and larger particles from the intestinal lumen to the region of the submucosal layer.
 Shigella invasion migrates to the submucosal layer, to the region of the lymphoid follicles, where it undergoes phagocytosis by mononuclear phagocytes. Shigella cause apoptosis of phagocytes, are again released into the submucosal layer and can penetrate into intact enterocytes through their basolateral membranes.
Shigella invasion migrates to the submucosal layer, to the region of the lymphoid follicles, where it undergoes phagocytosis by mononuclear phagocytes. Shigella cause apoptosis of phagocytes, are again released into the submucosal layer and can penetrate into intact enterocytes through their basolateral membranes.

 (D) Scanning electron micrograph of enteropathogenic E. coli attaching to support-like cell outgrowths on the surface of He. La cells. (E) Surrounding of Shigella flexneri by cytoplasmic cell outgrowths (ripple-like) during bacterial invasion of He. La epithelial cells.
(D) Scanning electron micrograph of enteropathogenic E. coli attaching to support-like cell outgrowths on the surface of He. La cells. (E) Surrounding of Shigella flexneri by cytoplasmic cell outgrowths (ripple-like) during bacterial invasion of He. La epithelial cells.
 With the formation of biofilms, the development of any infection begins. Biofilms are a thin layer of microorganisms with polymers secreted by them, which is adhered to an organic or inorganic surface. Microorganisms that make up the biofilm exist in two forms: fixed to the surface, and planktonic, free-floating, which is the substrate for the spread of infection from its primary locus. The composition of the surface shell and matrix of biofilms includes proteins, polysaccharides, lipids and nucleic acids (DNA and RNA)
With the formation of biofilms, the development of any infection begins. Biofilms are a thin layer of microorganisms with polymers secreted by them, which is adhered to an organic or inorganic surface. Microorganisms that make up the biofilm exist in two forms: fixed to the surface, and planktonic, free-floating, which is the substrate for the spread of infection from its primary locus. The composition of the surface shell and matrix of biofilms includes proteins, polysaccharides, lipids and nucleic acids (DNA and RNA)
 Biofilms This is the main phenotype of almost all bacteria in natural habitats, both in the external environment and in the human body in pathology. Biofilms provide protection from environmental factors and may include microorganisms from different kingdoms (eg bacteria and fungi). Among the pathogens that form biolens, P. aeruginosa, S. aureus, K. pneumoniae, Coagulasae - negative staphylococcus (CNS), Enterococcus spp. have the greatest clinical significance. , Candida spp.
Biofilms This is the main phenotype of almost all bacteria in natural habitats, both in the external environment and in the human body in pathology. Biofilms provide protection from environmental factors and may include microorganisms from different kingdoms (eg bacteria and fungi). Among the pathogens that form biolens, P. aeruginosa, S. aureus, K. pneumoniae, Coagulasae - negative staphylococcus (CNS), Enterococcus spp. have the greatest clinical significance. , Candida spp.
 Biofilms The existence of bacteria in the form of biofilms enhances their protection against phagocytosis, ultraviolet radiation, viruses and dehydration, as well as against antibiotics (withstanding concentrations of antibiotics 100-1000 times greater than inhibiting planktonic cells) and host immune defense factors. Therapeutic effect on biofilms can be directed to the mechanisms of initial adhesion of bacteria to the surface.
Biofilms The existence of bacteria in the form of biofilms enhances their protection against phagocytosis, ultraviolet radiation, viruses and dehydration, as well as against antibiotics (withstanding concentrations of antibiotics 100-1000 times greater than inhibiting planktonic cells) and host immune defense factors. Therapeutic effect on biofilms can be directed to the mechanisms of initial adhesion of bacteria to the surface.
 Adhesion of microorganisms to implantable devices. None of the materials used to create implantable devices are biologically inert. Microorganisms bind to their surfaces as a result of nonspecific adhesion, macroorganism proteins, most often fibrin, are deposited, and a film is formed, which contains molecules that are receptors for microbial adhesins, there are no factors that counteract adhesion.
Adhesion of microorganisms to implantable devices. None of the materials used to create implantable devices are biologically inert. Microorganisms bind to their surfaces as a result of nonspecific adhesion, macroorganism proteins, most often fibrin, are deposited, and a film is formed, which contains molecules that are receptors for microbial adhesins, there are no factors that counteract adhesion.
 Formation of biofilms ATTACHMENT COLONIZATION REPRODUCTION SURFACE - Colonization (environmental objects, heart valves, tooth enamel and others, catheters, ....) - Resistance to phagocytosis - Resistance to antibiotics
Formation of biofilms ATTACHMENT COLONIZATION REPRODUCTION SURFACE - Colonization (environmental objects, heart valves, tooth enamel and others, catheters, ....) - Resistance to phagocytosis - Resistance to antibiotics
 Factors of invasion Invasion - penetration of the pathogen through the mucous and connective tissue barriers Aggression - suppression of natural resistance and adaptive immunity. They act together. Many surface structures of a bacterial cell (flagella, surface proteins, Gram-bacterium cell wall lipopolysaccharide), as well as enzymes secreted by bacteria, are invasive and aggressive.
Factors of invasion Invasion - penetration of the pathogen through the mucous and connective tissue barriers Aggression - suppression of natural resistance and adaptive immunity. They act together. Many surface structures of a bacterial cell (flagella, surface proteins, Gram-bacterium cell wall lipopolysaccharide), as well as enzymes secreted by bacteria, are invasive and aggressive.
 Factors of invasion Invasion is the spread of microorganisms in the intercellular spaces of the tissues of the host organism and their penetration into its cells. Distribution factors - a number of enzymes produced by bacterial cells. Most of them are hydrolases.
Factors of invasion Invasion is the spread of microorganisms in the intercellular spaces of the tissues of the host organism and their penetration into its cells. Distribution factors - a number of enzymes produced by bacterial cells. Most of them are hydrolases.
 Invasion factors Hyaluronidase - depolymerizes hyaluronic acid, a high-polymer compound consisting of N-acetylglucosamine and D-glucuronic acid residues. The glycosidic bond is broken. Hyaluronic acid - the main component of connective tissue, is contained in cell membranes, intercellular substance, viscosity decreases. Produce staphylococci, streptococci, clostridia, cholera vibrio.
Invasion factors Hyaluronidase - depolymerizes hyaluronic acid, a high-polymer compound consisting of N-acetylglucosamine and D-glucuronic acid residues. The glycosidic bond is broken. Hyaluronic acid - the main component of connective tissue, is contained in cell membranes, intercellular substance, viscosity decreases. Produce staphylococci, streptococci, clostridia, cholera vibrio.
 Invasion factors Neuraminidase - hydrolyzes glycosidic bonds in glycoproteins, gangliosides, splits off sialic (neuraminic acids) residues from them, which consist of D-mannosamine and pyruvic acid residues. Sialic acids are part of mucin, mucosal secretions, give them viscosity, hinder the movement of the microorganism to epitheliocytes. They are located on the surface of tissues, leukocytes. Neuraminidase - destroys the mucin barrier, the activity of phagocytosis decreases. They produce staphylococci, streptococci, cholera vibrios, clostridia.
Invasion factors Neuraminidase - hydrolyzes glycosidic bonds in glycoproteins, gangliosides, splits off sialic (neuraminic acids) residues from them, which consist of D-mannosamine and pyruvic acid residues. Sialic acids are part of mucin, mucosal secretions, give them viscosity, hinder the movement of the microorganism to epitheliocytes. They are located on the surface of tissues, leukocytes. Neuraminidase - destroys the mucin barrier, the activity of phagocytosis decreases. They produce staphylococci, streptococci, cholera vibrios, clostridia.
 Factors of invasion and aggression Lecithinase - hydrolyzes lecithin (phosphoglyceride phosphatidylcholine), the main component of mammalian membranes, destroys lipids of cell membranes. Produce staphylococci, clostridia, bacilli, listeria.
Factors of invasion and aggression Lecithinase - hydrolyzes lecithin (phosphoglyceride phosphatidylcholine), the main component of mammalian membranes, destroys lipids of cell membranes. Produce staphylococci, clostridia, bacilli, listeria.

 proteolytic enzymes. The main purpose of the proteolytic enzymes formed by bacteria is the signal and effector molecules of the immune defense. Coagulase catalyzes the hydrolysis of peptide bonds. Hydrolases include fibrinolysin. This enzyme is able to dissolve fibrin, contributes to the generalization of infection. Proteases - elastase (elastin of lung tissue) gelatinase. Collagenases – tendon collagen (contains glycine).
proteolytic enzymes. The main purpose of the proteolytic enzymes formed by bacteria is the signal and effector molecules of the immune defense. Coagulase catalyzes the hydrolysis of peptide bonds. Hydrolases include fibrinolysin. This enzyme is able to dissolve fibrin, contributes to the generalization of infection. Proteases - elastase (elastin of lung tissue) gelatinase. Collagenases – tendon collagen (contains glycine).
 Ig. A protease - hydrolysis of secretory immunoglobulins Neisseria meningitidis Haemophilus spp. Streptococcus spp. serine protease Zinc protease
Ig. A protease - hydrolysis of secretory immunoglobulins Neisseria meningitidis Haemophilus spp. Streptococcus spp. serine protease Zinc protease
 Enzymes. DNase - hydrolysis of DNA molecules, breaking of phosphodiester bonds, breakdown of DNA and RNA molecules into oligonucleotides and mononucleotides, the viscosity of the medium decreases, promotes the reproduction of microorganisms. Staphylococcus, streptococcus. Plasmocoagulase - converts soluble fibrinogen into fibrin, causes blood plasma to coagulate. Produced in an inactive state. Produced by Staphylococcus aureus
Enzymes. DNase - hydrolysis of DNA molecules, breaking of phosphodiester bonds, breakdown of DNA and RNA molecules into oligonucleotides and mononucleotides, the viscosity of the medium decreases, promotes the reproduction of microorganisms. Staphylococcus, streptococcus. Plasmocoagulase - converts soluble fibrinogen into fibrin, causes blood plasma to coagulate. Produced in an inactive state. Produced by Staphylococcus aureus


 Enzymes Urease - the breakdown of urea, ammonia causes alkalization of the environment, a direct toxic effect. Toxic to the central nervous system. Suppresses cellular respiration. Reductive amination of ketoglutaric acid in mitochondria to glutamic acid occurs, which leads to the removal of ketoglutaric acid from the tricarboxylic acid cycle, suppression of cellular respiration. Brucella and Helicobacter are produced.
Enzymes Urease - the breakdown of urea, ammonia causes alkalization of the environment, a direct toxic effect. Toxic to the central nervous system. Suppresses cellular respiration. Reductive amination of ketoglutaric acid in mitochondria to glutamic acid occurs, which leads to the removal of ketoglutaric acid from the tricarboxylic acid cycle, suppression of cellular respiration. Brucella and Helicobacter are produced.



 Antiphagocytic factors Have a superficial localization - capsules, capsule-like structures Are not vital for a bacterial cell Have a macromolecular structure Hydrophilic
Antiphagocytic factors Have a superficial localization - capsules, capsule-like structures Are not vital for a bacterial cell Have a macromolecular structure Hydrophilic
 Antiphagocytic factors Protection against phagocytosis can occur at various stages of the process: At the stage of recognition-absorption Capsules, capsule-like polysaccharide M-protein of streptococci, K-antigen of gram-negative bacteria. Staphylococcus aureus has A-protein and the plasmacoagulase enzyme, under the action of which a fibrin sheath is formed around the cells, which prevents the recognition of bacteria by phagocytes.
Antiphagocytic factors Protection against phagocytosis can occur at various stages of the process: At the stage of recognition-absorption Capsules, capsule-like polysaccharide M-protein of streptococci, K-antigen of gram-negative bacteria. Staphylococcus aureus has A-protein and the plasmacoagulase enzyme, under the action of which a fibrin sheath is formed around the cells, which prevents the recognition of bacteria by phagocytes.

 Number (figure) 11. Negative staining of Streptococcus pyogenes by electron microscopy (28,000 X). The halo around the chain of cells is a capsule of hyaluronic acid that surrounds the bacteria from the outside. A septum may also be seen between a dividing pair of cells.
Number (figure) 11. Negative staining of Streptococcus pyogenes by electron microscopy (28,000 X). The halo around the chain of cells is a capsule of hyaluronic acid that surrounds the bacteria from the outside. A septum may also be seen between a dividing pair of cells.
 Bacillus anthracis colonies. Growth of mucoid or mucoid bacterial colonies usually indicates capsule production. In the case of B. anthracis, the capsule consists of poly-D-glutamine. The capsule is an essential determinant of bacterial pathogenicity. In the early stages of colonization and infection, the capsule protects bacteria from the antibacterial activity of the immune and phagocytic systems.
Bacillus anthracis colonies. Growth of mucoid or mucoid bacterial colonies usually indicates capsule production. In the case of B. anthracis, the capsule consists of poly-D-glutamine. The capsule is an essential determinant of bacterial pathogenicity. In the early stages of colonization and infection, the capsule protects bacteria from the antibacterial activity of the immune and phagocytic systems.
 Bacterial capsules contrasted with Chinese ink, viewed under a light microscope. This is a true capsule, a separate layer of polysaccharides around the cells. Sometimes bacterial cells are surrounded by a more random polysaccharide matrix called mucus or biofilm.
Bacterial capsules contrasted with Chinese ink, viewed under a light microscope. This is a true capsule, a separate layer of polysaccharides around the cells. Sometimes bacterial cells are surrounded by a more random polysaccharide matrix called mucus or biofilm.

 Microorganism Capsule nature Capsule polymer subunits Acetobacter xylinum Cellulose Glucose Azotobacter vinelandii Polyuronide Glucuronic and mannuronic acids Bac. anthracis Polypeptide D-Glutamic acid Bac. licheniformis Species from the Enterobacteriacceae family Many types of complex polysaccharides, colanoic acid Complex polysaccharide Galactose, glucose, glucuronic acid, PVC, fucose, etc. Galactose, galacturonic acid Leuconostoc mesenteroides Glucan (dextran) acid, fucose Glucose Pseudomonas aerugenosa Polyuronide or other polysaccharides ides Hyaluronic acid Klebsiella pneumoniae Streptococcus haemoliticus Streptococcus pyogenes Sterptococcus pneumoniae Many types of complex polymers, for example: Type I Type II Sterptococcus salivarius Fructan (levan) N. meningitidis Polysaccharide H. influenzae Polysaccharide Glucuronic. Mannuronic acid N-acetylglucosamine, glucuronic acid 3-deoxygalactose, galacturonic acid, glucose, glucuronic acid Fructose N-acetylmannosamine phosphate polymer (group A); sialic acid polymer (group B and C) Polyribose phosphate
Microorganism Capsule nature Capsule polymer subunits Acetobacter xylinum Cellulose Glucose Azotobacter vinelandii Polyuronide Glucuronic and mannuronic acids Bac. anthracis Polypeptide D-Glutamic acid Bac. licheniformis Species from the Enterobacteriacceae family Many types of complex polysaccharides, colanoic acid Complex polysaccharide Galactose, glucose, glucuronic acid, PVC, fucose, etc. Galactose, galacturonic acid Leuconostoc mesenteroides Glucan (dextran) acid, fucose Glucose Pseudomonas aerugenosa Polyuronide or other polysaccharides ides Hyaluronic acid Klebsiella pneumoniae Streptococcus haemoliticus Streptococcus pyogenes Sterptococcus pneumoniae Many types of complex polymers, for example: Type I Type II Sterptococcus salivarius Fructan (levan) N. meningitidis Polysaccharide H. influenzae Polysaccharide Glucuronic. Mannuronic acid N-acetylglucosamine, glucuronic acid 3-deoxygalactose, galacturonic acid, glucose, glucuronic acid Fructose N-acetylmannosamine phosphate polymer (group A); sialic acid polymer (group B and C) Polyribose phosphate


 Antiphagocytic factors Survival of microbial cells after absorption by a phagocyte. Interference between phagosome and lysosome fusion – the cord factor of mycobacteria Suppression of acidification processes in the phagolysosome leads to disruption of the action of lysosomal enzymes, genes are localized in the pathogenicity island (Sp. I 2), are expressed only after the microorganism enters the phagocytes. Destruction of the phagosome membrane before merging with the lysosome - listeria, rickettsia. Listeriolysin and phospholipases are involved in the formation of a pore in the phagosome membrane.
Antiphagocytic factors Survival of microbial cells after absorption by a phagocyte. Interference between phagosome and lysosome fusion – the cord factor of mycobacteria Suppression of acidification processes in the phagolysosome leads to disruption of the action of lysosomal enzymes, genes are localized in the pathogenicity island (Sp. I 2), are expressed only after the microorganism enters the phagocytes. Destruction of the phagosome membrane before merging with the lysosome - listeria, rickettsia. Listeriolysin and phospholipases are involved in the formation of a pore in the phagosome membrane.

 Invasion of non-phagocytic cells Active invasion of non-phagocytic cells, primarily epithelial cells: inside such cells, microorganisms are not exposed to any adverse effects. The described strategy is used by Salmonella and Shigella. Staphylococci, pyogenic streptococci and mycobacteria penetrate phagocytes using complement receptors. Phagocytosis mediated by these receptors does not lead to pronounced activation of the bactericidal systems of phagocytes.
Invasion of non-phagocytic cells Active invasion of non-phagocytic cells, primarily epithelial cells: inside such cells, microorganisms are not exposed to any adverse effects. The described strategy is used by Salmonella and Shigella. Staphylococci, pyogenic streptococci and mycobacteria penetrate phagocytes using complement receptors. Phagocytosis mediated by these receptors does not lead to pronounced activation of the bactericidal systems of phagocytes.
 Evasion of the immune response Variability of antigenic properties Antigenic mimicry Formation of L-forms Shielding of antigenic determinants using capsules
Evasion of the immune response Variability of antigenic properties Antigenic mimicry Formation of L-forms Shielding of antigenic determinants using capsules



 Bacterial toxins Have a direct pathological effect Exotoxins (protein toxins) - are released mainly into the environment. Endotoxins - associated with the structure of the bacterial cell
Bacterial toxins Have a direct pathological effect Exotoxins (protein toxins) - are released mainly into the environment. Endotoxins - associated with the structure of the bacterial cell

 Bacterial toxins Simple - a polypeptide chain Complex - several linked polypeptide chains interconnected. Simple toxins are produced in an inactive form (protoxin) - activated by proteases. The biological meaning of activation is the formation of a bifunctional system of subunits A and B. B- transport and receptor function A- has enzymatic properties, has a specific effect
Bacterial toxins Simple - a polypeptide chain Complex - several linked polypeptide chains interconnected. Simple toxins are produced in an inactive form (protoxin) - activated by proteases. The biological meaning of activation is the formation of a bifunctional system of subunits A and B. B- transport and receptor function A- has enzymatic properties, has a specific effect
 Classification by mechanism of action Inhibit protein synthesis - cytotoxins Damage cell membranes - membrane toxins Disrupt signaling - functional blockers Protease toxins - functional blockers Superantigen toxins - immunotoxins
Classification by mechanism of action Inhibit protein synthesis - cytotoxins Damage cell membranes - membrane toxins Disrupt signaling - functional blockers Protease toxins - functional blockers Superantigen toxins - immunotoxins
 The mechanism of action of toxins Violating protein synthesis Diphtheria toxin is simple. Possesses Ribosyl-transferase activity, transfers ADF-ribose On the target, the elongation factor, transferase-2, disrupts the elongation of polypeptide chains
The mechanism of action of toxins Violating protein synthesis Diphtheria toxin is simple. Possesses Ribosyl-transferase activity, transfers ADF-ribose On the target, the elongation factor, transferase-2, disrupts the elongation of polypeptide chains

 Protein Synthesis Interfering Toxins Shiga-toxin - Subunit A, which has enzymatic activity, acts as N-glycosidase, cleaving off a single adenine residue from 28 S ribosomal RNA. It causes enzymatic damage to 28 s ribosomal RNA of colon epithelial cells, disrupts the functioning of ribosomes, elongation factors cannot bind to ribosomes, disrupts protein synthesis, and the cell dies.
Protein Synthesis Interfering Toxins Shiga-toxin - Subunit A, which has enzymatic activity, acts as N-glycosidase, cleaving off a single adenine residue from 28 S ribosomal RNA. It causes enzymatic damage to 28 s ribosomal RNA of colon epithelial cells, disrupts the functioning of ribosomes, elongation factors cannot bind to ribosomes, disrupts protein synthesis, and the cell dies.
 Pore-forming toxins. Bacterial toxins that function by inserting into the host plasma membrane and forming transmembrane pores in it, leading the cell to lysis.
Pore-forming toxins. Bacterial toxins that function by inserting into the host plasma membrane and forming transmembrane pores in it, leading the cell to lysis.
 Pore-forming hemolysins and leukocidin. Can damage monocytes, platelets. Alpha toxin of staphylococci Violating the integrity of cell membranes by enzymatic hydrolysis of phospholipids - phospholipase C. perfringens Toxins that damage cell membranes.
Pore-forming hemolysins and leukocidin. Can damage monocytes, platelets. Alpha toxin of staphylococci Violating the integrity of cell membranes by enzymatic hydrolysis of phospholipids - phospholipase C. perfringens Toxins that damage cell membranes.



 Functional blockers (activators of metabolic pathways of secondary messengers Disrupting the function of adanylate cyclase - Cholera toxin - a complex toxin, consists of subunit A and 5 subunits B, in the form of ring A 1 it has glycohydrolase and ribosyl transferase activity. ADF-ribose is transferred to GTP Adenylate cyclase is activated, leads to excessive accumulation of c.
Functional blockers (activators of metabolic pathways of secondary messengers Disrupting the function of adanylate cyclase - Cholera toxin - a complex toxin, consists of subunit A and 5 subunits B, in the form of ring A 1 it has glycohydrolase and ribosyl transferase activity. ADF-ribose is transferred to GTP Adenylate cyclase is activated, leads to excessive accumulation of c.

 C. botulinum neurotoxins (Bo. NT serotypes A v. G) and C. tetani proteases Neurotoxins are synthesized as inactive polypeptides with a molecular weight of up to 150 kDa. Each active neurotoxin molecule consists of heavy (100 kDa) and light (50 kDa) chains connected by a single bisulfide bond. The heavy chain contains two domains: a site responsible for the translocation of the toxin at the N-terminus, and a region at the C-terminus that regulates the binding of the toxin to the cell. The light chains contain zinc binding sequences to carry out the zinc ion dependent protease activity of the toxin.
C. botulinum neurotoxins (Bo. NT serotypes A v. G) and C. tetani proteases Neurotoxins are synthesized as inactive polypeptides with a molecular weight of up to 150 kDa. Each active neurotoxin molecule consists of heavy (100 kDa) and light (50 kDa) chains connected by a single bisulfide bond. The heavy chain contains two domains: a site responsible for the translocation of the toxin at the N-terminus, and a region at the C-terminus that regulates the binding of the toxin to the cell. The light chains contain zinc binding sequences to carry out the zinc ion dependent protease activity of the toxin.
 Tetanospasmin - tetanus toxin, a simple toxin Activation requires proteolytic cleavage into light and heavy chains Cellular targets a group of proteins necessary for the connection of synaptic vesicles with presynaptic plasma membranes, followed by the release of neurotransmitters
Tetanospasmin - tetanus toxin, a simple toxin Activation requires proteolytic cleavage into light and heavy chains Cellular targets a group of proteins necessary for the connection of synaptic vesicles with presynaptic plasma membranes, followed by the release of neurotransmitters
 Neurotoxin Tetanus toxin affects two types of neurons. It binds to receptors on the presynaptic membrane of motor neurons, then, with the help of reverse vesicular transport, moves to the spinal cord, where it is introduced into inhibitory and intercalary neurons. Cleavage of vesicle-associated membrane protein and synaptobrevin in these neurons leads to impaired release of glycine and gamma-aminobutyric acid, which are able to stop muscle contraction.
Neurotoxin Tetanus toxin affects two types of neurons. It binds to receptors on the presynaptic membrane of motor neurons, then, with the help of reverse vesicular transport, moves to the spinal cord, where it is introduced into inhibitory and intercalary neurons. Cleavage of vesicle-associated membrane protein and synaptobrevin in these neurons leads to impaired release of glycine and gamma-aminobutyric acid, which are able to stop muscle contraction.
 Proteolytic toxins neurotoxins It has protease activity, destroys synaptobrevin protein, blocks the inhibitory system - convulsions Botulinum toxin - acts as an endoprotease, destroys target proteins, disrupts the secretion of acetylcholine, blockade of motor neurons, flaccid paralysis.
Proteolytic toxins neurotoxins It has protease activity, destroys synaptobrevin protein, blocks the inhibitory system - convulsions Botulinum toxin - acts as an endoprotease, destroys target proteins, disrupts the secretion of acetylcholine, blockade of motor neurons, flaccid paralysis.
 Toxins-superantigens, immune response activators The immunostimulatory potential of toxins is a consequence of their ability to bind various regions of proteins of the type II major histocompatibility complex expressed on the surface of antigen-presenting cells and Vbeta elements on the T-cell receptor. Binding of TSST-1 to Vbeta 2 results in massive proliferation of over 20% of peripheral T cells. Massive release of cytokines results from T-cell expansion Cytokines cause hypotension, high fever, and diffuse erythematous lesions
Toxins-superantigens, immune response activators The immunostimulatory potential of toxins is a consequence of their ability to bind various regions of proteins of the type II major histocompatibility complex expressed on the surface of antigen-presenting cells and Vbeta elements on the T-cell receptor. Binding of TSST-1 to Vbeta 2 results in massive proliferation of over 20% of peripheral T cells. Massive release of cytokines results from T-cell expansion Cytokines cause hypotension, high fever, and diffuse erythematous lesions


The phenotypic feature of a pathogenic microorganism is its virulence., i.e. a property of a strain that manifests itself under certain conditions (with the variability of microorganisms, changes in the susceptibility of a macroorganism, etc.). Virulence can be increased, decreased, measured, i.e. it is a measure of pathogenicity. Quantitative indicators of virulence can be expressed in DLM (minimum lethal dose), DL" (dose that causes the death of 50% of experimental animals). At the same time, the type of animals, sex, body weight, method of infection, time of death are taken into account.
To pathogenicity factors include the ability of microorganisms to attach to cells (adhesion), be placed on their surface (colonization), penetrate cells (invasion) and resist the body's defense factors (aggression).
Adhesion is the starting mechanism of the infectious process. Adhesion is understood as the ability of a microorganism to be adsorbed on sensitive cells with subsequent colonization. The structures responsible for binding a microorganism to a cell are called adhesins and they are located on its surface. Adhesins are very diverse in structure and cause high specificity - the ability of some microorganisms to attach to the epithelial cells of the respiratory tract, others - of the intestinal tract or genitourinary system, etc. The adhesion process can be influenced by physicochemical mechanisms associated with the hydrophobicity of microbial cells, the sum of the energy of attraction and repulsion. In gram-negative bacteria, adhesion occurs due to pili I and common types. In Gram-positive bacteria, adhesins are proteins and teichoic acids of the cell wall. In other microorganisms, this function is performed by various structures of the cellular system: surface proteins, lipopolysaccharides, etc.
Invasion. Invasiveness is understood as the ability of microbes to penetrate through the mucous membranes, skin, connective tissue barriers into the internal environment of the body and spread through its tissues and organs. The penetration of a microorganism into a cell is associated with the production of enzymes, as well as with factors that suppress cellular defense. So the enzyme hyaluronidase breaks down hyaluronic acid, which is part of the intercellular substance, and thus increases the permeability of the mucous membranes and connective tissue. Neuraminidase breaks down neuraminic acid, which is part of the surface receptors of mucous membrane cells, which contributes to the penetration of the pathogen into tissues.
Aggression. Under the aggressiveness understand the ability of the pathogen to resist the protective factors of the macroorganism. Aggression factors include: proteases - enzymes that destroy immunoglobulins; coagulase - an enzyme that coagulates blood plasma; fibrinolysin - dissolving fibrin clot; lecithinase is an enzyme that acts on the phospholipids of the membranes of muscle fibers, erythrocytes and other cells. Pathogenicity can also be associated with other enzymes of microorganisms, while they act both locally and generalized.
Toxins play an important role in the development of the infectious process. According to their biological properties, bacterial toxins are divided into exotoxins and endotoxins.
Exotoxins produce both Gram-positive and Gram-negative bacteria. According to their chemical structure, they are proteins. According to the mechanism of action of exotoxin on the cell, several types are distinguished: cytotoxins, membrane toxins, functional blockers, exfoliants and erythrohemins. The mechanism of action of protein toxins is reduced to damage to vital processes in the cell: increased membrane permeability, blockade of protein synthesis and other biochemical processes in the cell, or disruption of interaction and coordination between cells. Exotoxins are strong antigens that produce the formation of antitoxins in the body.
Exotoxins are highly toxic. Under the influence of formalin and temperature, exotoxins lose their toxicity, but retain their immunogenic properties. These toxins are called toxoids and are used for the prevention of tetanus, gangrene, botulism, diphtheria, and are also used as antigens for immunizing animals in order to obtain anatoxic sera.
Endotoxins in their chemical structure, they are lipopolysaccharides, which are contained in the cell wall of gram-negative bacteria and are released into the environment during bacterial lysis. Endotoxins do not have specificity, are thermostable, less toxic, and have weak immunogenicity. When large doses enter the body, endotoxins inhibit phagocytosis, granulocytosis, monocytosis, increase capillary permeability, and have a destructive effect on cells. Microbial lipopolysaccharides destroy blood leukocytes, cause degranulation of mast cells with the release of vasodilators, activate the Hageman factor, which leads to leukopenia, hyperthermia, hypotension, acidosis, and disseminated intravascular coagulation (DVC).
Endotoxins stimulate the synthesis of interferons, activate the complement system in the classical way, and have allergic properties.
With the introduction of small doses of endotoxin, the body's resistance increases, phagocytosis increases, and B-lymphocytes are stimulated. The serum of an animal immunized with endotoxin has weak antitoxic activity and does not neutralize endotoxin.
The pathogenicity of bacteria is controlled by three types of genes: genes - by their own chromosomes, genes introduced by plasmids by temperate phages.